Health Care > QUESTIONS & ANSWERS > Exam 2 Blueprint Fall 2021 health care study guide (All)
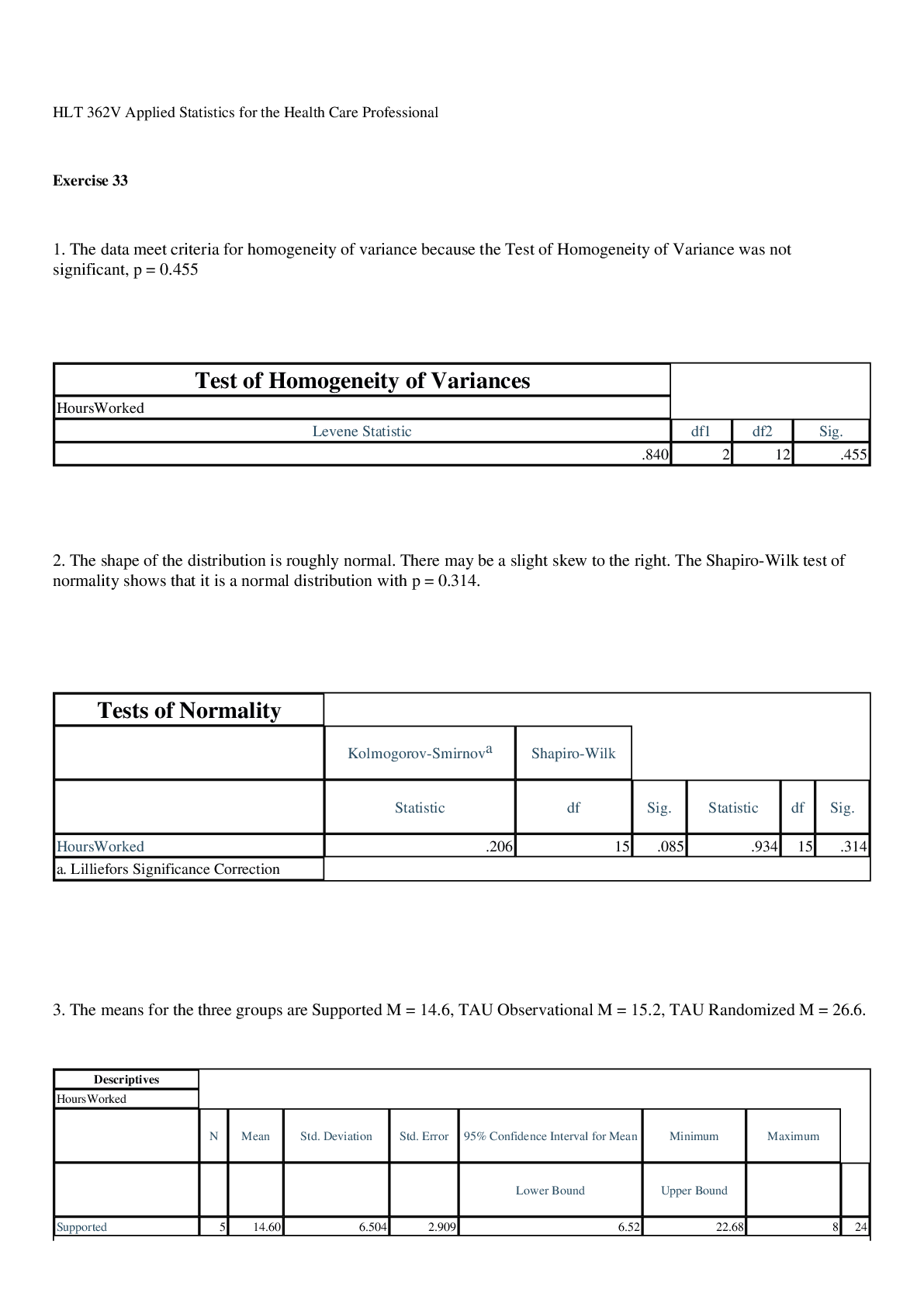
Exam 2 Blueprint Fall 2021 health care study guide
Document Content and Description Below
Dysphagia Difficulty swallowing o Causes Nero disease: Parkinson’s, dementias, muscular dystrophy, Huntington’s, ALS, MN, Guillain Barre Syndrome. Other: Congenital issues/cerebral palsy, Esopha... geal stenosis, esophageal diverticula, tumors, stroke, achalasia Vomiting – why and consequences Why: protect against substance, reverse peristalsis, increase intracranial pressure, severe pain. Consequences: lead to fluid, electrolyte, pH imbalance, aspiration o Emesis types and why the emesis would be a problem Hematemesis: blood in vomit (protein), Yellow/green: presence of bile. Deep brown: fecal matter. Undigested food o Treatment of vomiting disorders Antiemetic med., fluid replacement, correct electrolyte imbalance, restore acid-base Esophageal disorders o Hiatal hernia Stomach section protrudes through diaphragm Causes: Weakening of diaphragm muscle, trauma, congenital defects. Manifestation: Indigestion; heartburn; frequent belching; nausea; chest pain; strictures; dysphagia; and soft abdominal mass. diagnosis: H & P; barium swallow; upper GI Xrays; EGD, treatment: eat small meals, sleep elevated, antacid o GERD Causes: Certain foods: chocolate, caffeine, carbonated beverages, citrus fruit, tomatoes, spicy or fatty foods, peppermint , Alcohol consumption; nicotine, Hiatal hernia, Obesity; pregnancy, Certain medications – such as corticosteroids; beta blockers; calcium-channel blockers; anticholinergics, NG intubation, Delayed gastric emptying Manifestations: Heartburn, Epigastric pain, Dysphagia, Dry cough, Laryngitis Pharyngitis, Food regurgitation, Sensation of lump in throat Diagnosis: H & P; barium swallow; EGD; esophageal pH monitoring Treatments: Avoid triggers; avoid restrictive clothing, Eat small frequent meals; high Fowler’s positioning, Weight loss; stress reduction; Antacids; acid reducing agent; mucosal barrier agents, Herbal therapies (licorice, chamomile), Surgery Complications: Esophagitis; strictures; ulcerations; esophageal cancer; chronic pulmonary disease o Gastritis/gastroenteritis Acute: Can be mild, transient irritation or can be severe ulceration with hemorrhage, Usually develops suddenly, Likely to also have nausea & epigastric pain Chronic: Develops gradually May be asymptomatic but usually accompanied by dull epigastric pain and a sensation of fullness after minimal intake Complications: peptic ulcer; gastric cancer; hemorrhage H. pylori: Most common cause of chronic gastritis Bacteria embeds in mucous layer; activates toxins & enzymes that cause inflammation Genetic vulnerability & lifestyle behaviors (smoking, stress) may increase susceptible Other causes : Organisms through food/water contamination, LT NSAID use, Excess alcohol use, Severe stress, Autoimmune conditions Manifestations of GI bleeding : Indigestion; heart burn, Epigastric pain; abdominal cramping, N/V; anorexia, Fever; malaise, Hematemesis, Dark, tarry stools = ulceration & bleeding Essentials of Pathophysiology (NUR 2063) – Exam 2 blueprint 1 GI tract disorders o Peptic ulcer disease Duodenal: Most commonly associated with excess acid or H.pylori infections, Typically present with epigastric pain relieved by food Gastric: Less frequent; more deadly, typically associated with malignancy and NSAIDs, Pain worsens with food Symptoms: Curling’s ulcer from what: associated with burns Cushing’s ulcer from what: associated with head injuries Complications of ulcers: GI hemorrhage; obstruction; perforation; peritonitis Manifestations: Epigastric or abdominal pain, Abdominal cramping, Heartburn; indigestion, N/V Diagnosis: same as gastritis Treatment: Same as for gastritis, Surgical repair may be necessary for perforated or bleeding ulcers, Prevention is crucial – may need prophylactic medications (ex: acidreducers) for at-risk clients o Gallbladder disorders Cholelithiasis: Gallbladder stones Cholecystitis: Inflammation or infection in the biliary system caused by calculi Manifestations: Biliary colic; abdominal distension; N/V; jaundice; fever; leukocytosis Diagnosis: H & P; abdominal Xray; gallbladder US; laparoscopy Treatments: Low-fat diet, medications to dissolve calculi, Antibiotic therapy, NG tube with intermittent sxn, Lithotripsy, Choledochostomy, Laparoscopic surgery o Liver disorders Hepatitis – infectious: A, B, C, D, E vs. noninfectious: Giant cell hepatitis, Ischemic hepatitis, Non-alcoholic fatty liver hepatitis, Autoimmune hepatitis, Toxic & drug-induced hepatitis, Alcoholic hepatitis Transmission of viral hepatitis: If it’s a Vowel, it comes from the Bowel. All others are blood Define: acute: Proceeds through 4 stages—asymptomatic stage then 3 symptomatic stages chronic: Characterized by continued liver disease > 6 months, Symptom severity and disease progression vary by degree of liver damage, Can quickly deteriorate with declining liver integrity fulminant: Uncommon, rapidly progressing form that can quickly lead to Liver failure, hepatic encephalopathy, or death within 3 wks Diagnosis: H & P, Serum hepatitis profile, Liver enzymes, Clotting studies, Liver biopsy, Abdominal US treatment for viral hepatitis: treat with interferon & antiviral mediations Cirrhosis Common causes: Hep C and chronic alcohol abuse most common cause in U.S. Hepatitis and all factors that can lead to hepatitis What happens to liver: Leads to fibrosis, nodule formation, impaired blood flow, and bile obstruction liver failure Manifestations: Portal hypertension, Varicosities, Bleeding –slow or severe, Muscle wasting, Bile accumulation, Clay-colored stools, Dark urine, Ulcers/GI bleeding, Encephalopathy, Spontaneous bacterial peritonitis Essentials of Pathophysiology (NUR 2063) – Exam 2 blueprint 2 Diagnosis & treatments: H & P; liver biopsy; abdominal Xray; liver enzymes; EGD; clotting studies; stool exam for occult blood Hepatic encephalopathy: o Pancreatitis Causes: Cholelithiasis, Alcohol abuse, Biliary dysfunction, Hepatotoxic drugs, Metabolic disorders, Trauma, Renal failure, Endocrine disorders, Pancreatic tumors, Penetrating peptic ulcer What happens to the pancreas in the disorder? pancreatic enzymes to leak into the pancreatic tissue and initiate autodigestion - -results in edema, vascular damage, hemorrhage & necrosis Acute pancreatitis importance & complications: Acute respiratory distress syndrome (ARDS), DM, Infection, Septic or hypovolemic shock, Disseminated intravascular coagulation (DIC), Renal failure, Malnutrition, Pancreatic cancer Pseudocyst – pancreatic fluids & necrotic debris accumulate & eventually rupture, Abscess Manifestations: Upper abdominal pain that radiates to the back, worsens after eating, somewhat relieved by leaning forward or pulling knees to chest, N/V Mild jaundice, Low-grade fever, BP and pulse changes Chronic pancreatitis manifestations: Upper abdominal pain, Indigestion, Losing weight without trying, Steatorrhea, Constipation, Flatulence Pancreatitis diagnosis: H & P, Serum amylase & lipase, Serum calcium level, CBC, Liver enzymes, Serum bilirubin level, ABG, Stool analysis (lipid & trypsin levels), Abdominal Xray, CT/MRI, Abdominal US, ERCP (endoscopic retrograde cholangiopancreatography) treatment: Rest pancreas by fasting; administer IV nutrition; gradually advance diet from clears as tolerated to low fat, Pancreatic enzyme supplements when diet resumed Maintain hydration with IVF, NG to intermittent suction, Antiemetic agents, Pain management, Antacids/acid-reducing agents, Anticholinergic meds, Antibiotics, Insulin Bowel disorders o Diarrhea – acute: Often d/t bacterial or viral infections, Certain medications such as antibiotics, antacids, laxatives, usually self-limiting depending on cause o Chronic: Lasts longer than 4 weeks o Causes: Inflammatory bowel diseases, Malabsorption syndromes, Endocrine disorders, Chemo/radiation Manifestations: If small bowel: Large and loose, provoked by eating, Usually accompanied with pain in right lower quadrant, If large bowel: Stools are small and frequent, Frequently accompanied by pain and cramping in the left lower quadrant, Acute diarrhea is generally infectious, Accompanied by cramping, fever, chills, N/V Blood (may be frank, occult, or melena), pus, or mucus may be present Bowel sounds may be hyperactive, Fluid, electrolyte and pH imbalances, Metabolic alkalosis Diagnosis/Bristol stool chart: H & P, include usual bowel habits and complete Bristol Stool chart, Stool analysis –include cultures & occult blood, CBC, Blood chemistry ABG, Abdominal US Treatment: Fasting for acute diarrhea with infection, Antidiarrheal agents maybe or not Antibiotics may be needed, Anticholinergics, Antispasmodic agents, Clear liquid diet until diarrhea subsides, then advance diet as tolerated. Dietary fiber to manage chronic diarrhea, maintain hydration and correct electrolyte and pH imbalance, Meticulous skin care in presence of incontinence Essentials of Pathophysiology (N [Show More]
Last updated: 1 year ago
Preview 1 out of 18 pages

Buy this document to get the full access instantly
Instant Download Access after purchase
Add to cartInstant download
We Accept:

Reviews( 0 )
$7.50
Document information
Connected school, study & course
About the document
Uploaded On
Apr 30, 2022
Number of pages
18
Written in
Additional information
This document has been written for:
Uploaded
Apr 30, 2022
Downloads
0
Views
31









.png)