NURS 6551 Week 3 Soap note ob- gynecology 2022 update
Document Content and Description Below
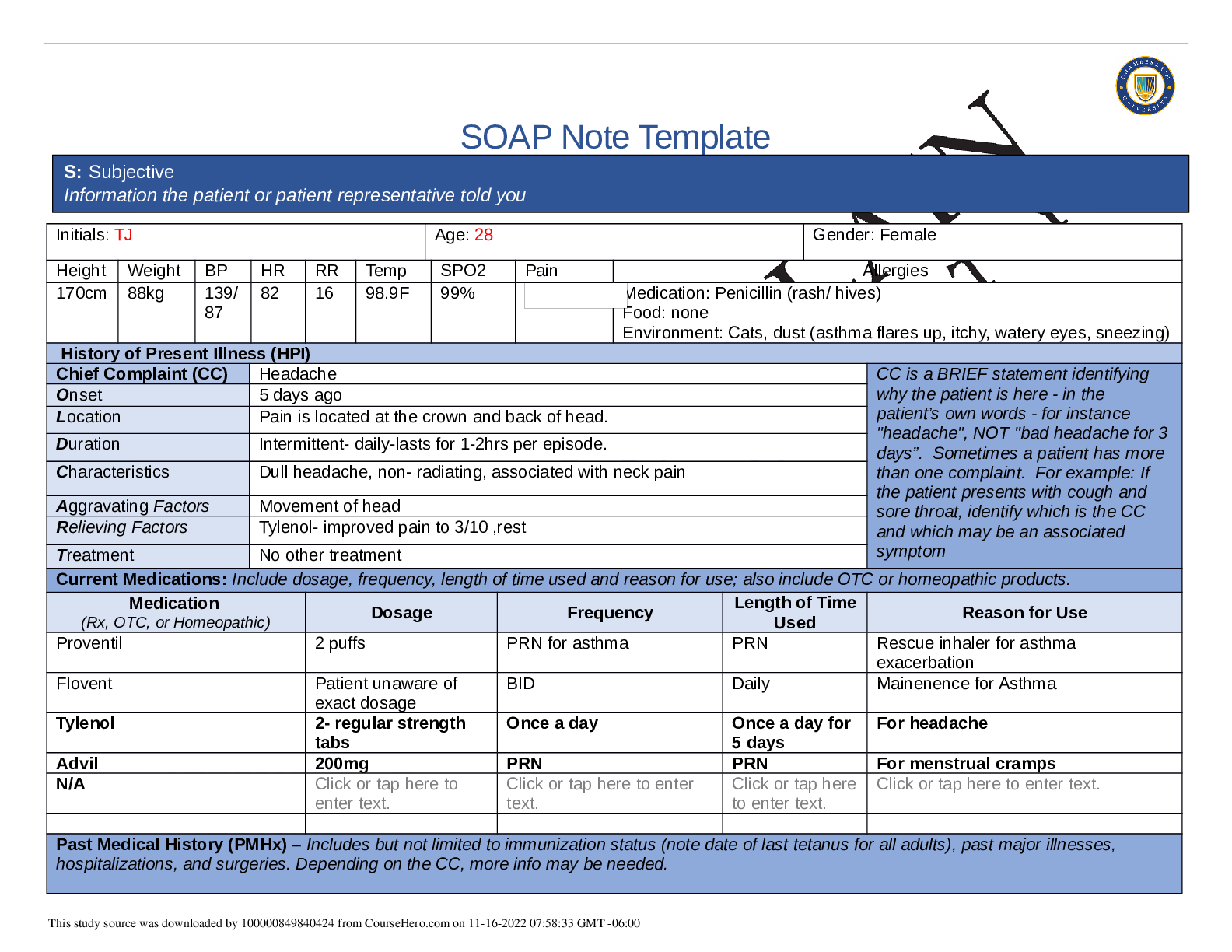
Subjective: What details did the patient provide regarding her personal and medical history? Objective: What observations did you make during the physical assessment? Assessment: What were your dif... ferential diagnoses? Provide a minimum of three possible diagnoses. List them from highest priority to lowest priority. What was your primary diagnosis and why? Plan: What was your plan for diagnostics and primary diagnosis? What was your plan for treatment and management, including alternative therapies? Include pharmacologic and nonpharmacologic treatments, alternative therapies, and follow-up parameters, as well as a rationale for this treatment and management plan. Reflection notes: What would you do differently in a similar patient evaluation? HPI: A.M, a 20-year-old Caucasian female came to the clinic with C/O bumps at her private part which she noticed 5 days ago while taking a shower. She denies any fever chills or any pain, itching or discharge at site. She has not tried any treatment other than applying warm compress at site with no effect. She reports severity as mild but is extremely anxious as she is in sexual relationship with a new partner for a month. Medications: Depaprovera shot Allergies: NKDA. No known food allergies Past Medical History (PMH [Show More]
Last updated: 1 year ago
Preview 1 out of 5 pages

Buy this document to get the full access instantly
Instant Download Access after purchase
Add to cartInstant download
We Accept:

Reviews( 0 )
$16.50
Document information
Connected school, study & course
About the document
Uploaded On
Sep 14, 2022
Number of pages
5
Written in
Additional information
This document has been written for:
Uploaded
Sep 14, 2022
Downloads
0
Views
55


.png)
.png)
.png)
.png)
.png)


.png)
.png)