NURS 200Feedback Log & Score Jared Griffin ./ Best feedback to score A
Document Content and Description Below
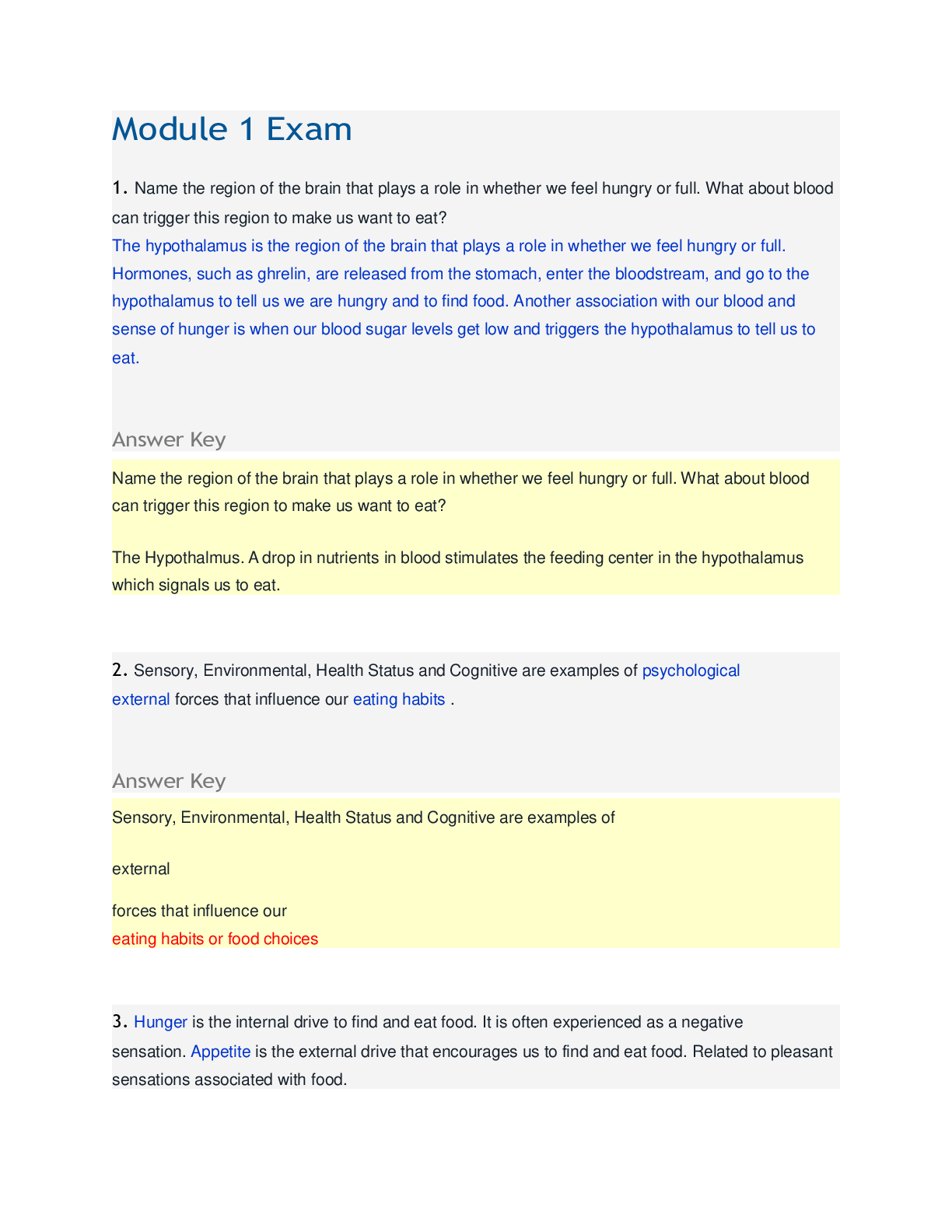
0:00 You reviewed the MAR. 0:00 You reviewed the orders. 0:00 You reviewed the intake and output. 0:10 Patient status - ECG: Sinus rhythm. Heart rate: 79. Pulse: Present. Blood pressure: 132/79 mm... Hg. Respiration: 16. Conscious state: Appropriate. SpO2: 97%. Temp: 99 F (37 C) 0:14 You introduced yourself. This was reasonable. 0:28 You identified the patient. To maintain patient safety, it is important that you quickly identify the patient. 0:37 You asked if the patient was <Allergy>allergic<> to anything. He replied: 'Yes, I am allergic to codeine.' 1:03 You educated the patient about activities, safety, and fall risk. 1:10 Patient status - ECG: Sinus rhythm. Heart rate: 79. Pulse: Present. Blood pressure: 131/79 mm Hg. Respiration: 15. Conscious state: Appropriate. SpO2: 97%. Temp: 98 F (36.9 C) 1:30 You educated the patient about personal protective equipment. 1:58 You educated the patient about use of incentive spirometer. This was indicated by order. 2:10 Patient status - ECG: Sinus rhythm. Heart rate: 79. Pulse: Present. Blood pressure: 133/80 mm Hg. Respiration: 15. Conscious state: Appropriate. SpO2: 97%. Temp: 98 F (36.9 C) 2:26 You educated the patient about wound care. This is an important part of infection control. 2:46 You asked the patient if he had any pain. He replied: 'Yes, I am feeling a little sore in my knee.' 2:51 You asked: How would you rate your pain? He replied: 'Not too bad; it's about a 2. ' 2:59 You asked the patient if he needed anything for the pain. He replied: 'No. I'm okay.' 3:10 Patient status - ECG: Sinus rhythm. Heart rate: 79. Pulse: Present. Blood pressure: 136/81 mm Hg. Respiration: 15. Conscious state: Appropriate. SpO2: 97%. Temp: 98 F (36.9 C) 3:30 You assessed the patient's dressing. This is a correct assessment in monitoring for infection. 3:46 You examined the patient's legs. The right knee can be bent about 75 degrees. There is a dressing covering the skin lesion on the lower leg. There is normal elasticity of the skin. His color is normal, and he is not sweating. 4:10 Patient status - ECG: Sinus rhythm. Heart rate: 79. Pulse: Present. Blood pressure: 132/79 mm Hg. Respiration: 15. Conscious state: Appropriate. SpO2: 97%. Temp: 98 F (36.9 C) 4:14 You checked the pedal pulse. The pulse is strong, 80 per minute, and regular. It is 4:41 You checked the capillary refill time. The capillary refill time was less than 2 seconds. 4:57 You assessed the patient's IV. The site had no redness, swelling, infiltration, bleeding, or drainage. The dressing was dry and intact. This is correct. Assessing any IVs the patient has is always important. 5:10 Patient status - ECG: Sinus rhythm. Heart rate: 79. Pulse: Present. Blood pressure: 133/80 mm Hg. Respiration: 15. Conscious state: Appropriate. SpO2: 97%. Temp: 98 F (36.9 C) 5:31 You listened to the lungs of the patient. The breath sounds are clear and equal bilaterally. 5:53 You listened to the heart of the patient. This is reasonable. There were regular heart sounds without murmurs. 6:10 Patient status - ECG: Sinus rhythm. Heart rate: 79. Pulse: Present. Blood pressure: 133/79 mm Hg. Respiration: 15. Conscious state: Appropriate. SpO2: 97%. Temp: 98 F (36.9 C) 6:20 You listened to the abdomen of the patient. Normal bowel sounds were heard. 6:33 You checked the <Temperature>temperature<> at the ear. The temperature was 98 F (36.9 C). This is a correct assessment in monitoring for possible infection. 7:10 Patient status - ECG: Sinus rhythm. Heart rate: 79. Pulse: Present. Blood pressure: 135/81 mm Hg. Respiration: 15. Conscious state: Appropriate. SpO2: 97%. Temp: 98 F (36.9 C) 7:11 You attached the <Pulseoximeter>pulse oximeter.<> Consider assessing the patient's pulse oximetry as part of the first assessments you do. 7:13 You looked for normal breathing. He is breathing at 15 breaths per minute. The chest is moving equally. Consider assessing the patient's breathing and respiratory rate as part of the first assessments you do. 7:36 You checked the radial pulse. The pulse is strong, 80 per minute, and regular. Consider assessing the patient's pulse as part of the first assessments you do. 8:02 You measured the <Bloodpressure>blood pressure<> at 134/80 mm Hg. Consider assessing the patient's blood pressure as part of the first assessments you do. 8:10 Patient status - ECG: Sinus rhythm. Heart rate: 79. Pulse: Present. Blood pressure: 132/80 mm Hg. Respiration: 15. Conscious state: Appropriate. SpO2: 97%. Temp: 98 F (36.9 C) 8:20 You disconnected the <Pulseoximeter>pulse oximeter.<> 8:46 You checked the eye movements. Extraocular movements within normal limits. 9:04 You checked the patient's pupils, and they were 5 mm and reactive. 9:10 Patient status - ECG: Sinus rhythm. Heart rate: 79. Pulse: Present. Blood pressure: 137/82 mm Hg. Respiration: 15. Conscious state: Appropriate. SpO2: 97%. Temp: 98 F (36.9 C) 9:27 You put an emesis basin at the bedside. This is reasonable. 9:38 You gave the patient a sip of water. 10:05 The patient used an incentive spirometer. This was indicated by order. 10:10 Patient status - ECG: Sinus rhythm. Heart rate: 79. Pulse: Present. Blood pressure: 135/80 mm Hg. Respiration: 15. Conscious state: Appropriate. SpO2: 97%. Temp: 98 F (36.9 C) 11:10 Patient status - ECG: Sinus rhythm. Heart rate: 80. Pulse: Present. Blood pressure: 134/80 mm Hg. Respiration: 15. Conscious state: Appropriate. SpO2: 97%. Temp: 98 F (36.9 C) 11:19 A patient handoff was performed. This patient underwent a right total knee arthroplasty (TKA) yesterday morning. He is a carrier of methicillin-resistant Staphylococcus aureus (MRSA) and has been placed in contact precautions. He has a history of osteoarthritis and mild hypertension. The scenario addresses aspects of infection control, and the students are expected to adhere to local protocols, including use of personal protective equipment, contact precautions, and hand hygiene. CDC recommends contact precautions when the facility (based on national or local regulations) deems MRSA to be of special clinical and epidemiologic significance. Moreover, ongoing postoperative assessments and interventions are implemented to decrease the risk for postoperative complications. If postoperative complications occur, the nurse provides physical assessments and care, provides emotional support to the patient and family, and carries out prescribed treatments. You got 100% [Show More]
Last updated: 1 year ago
Preview 1 out of 4 pages

Reviews( 0 )
Document information
Connected school, study & course
About the document
Uploaded On
Aug 02, 2021
Number of pages
4
Written in
Additional information
This document has been written for:
Uploaded
Aug 02, 2021
Downloads
0
Views
18












 (1).png)
 (1).png)
 (1).png)