*NURSING > SHADOW HEALTH > Shadow Health: Ppatient Tina Jones: Transcript Subjective Data Collection Objective Data Collection (All)
Shadow Health: Ppatient Tina Jones: Transcript Subjective Data Collection Objective Data Collection Education & Empathy Documentation Information Processing Health History Tips and Tricks Self-Reflection
Document Content and Description Below
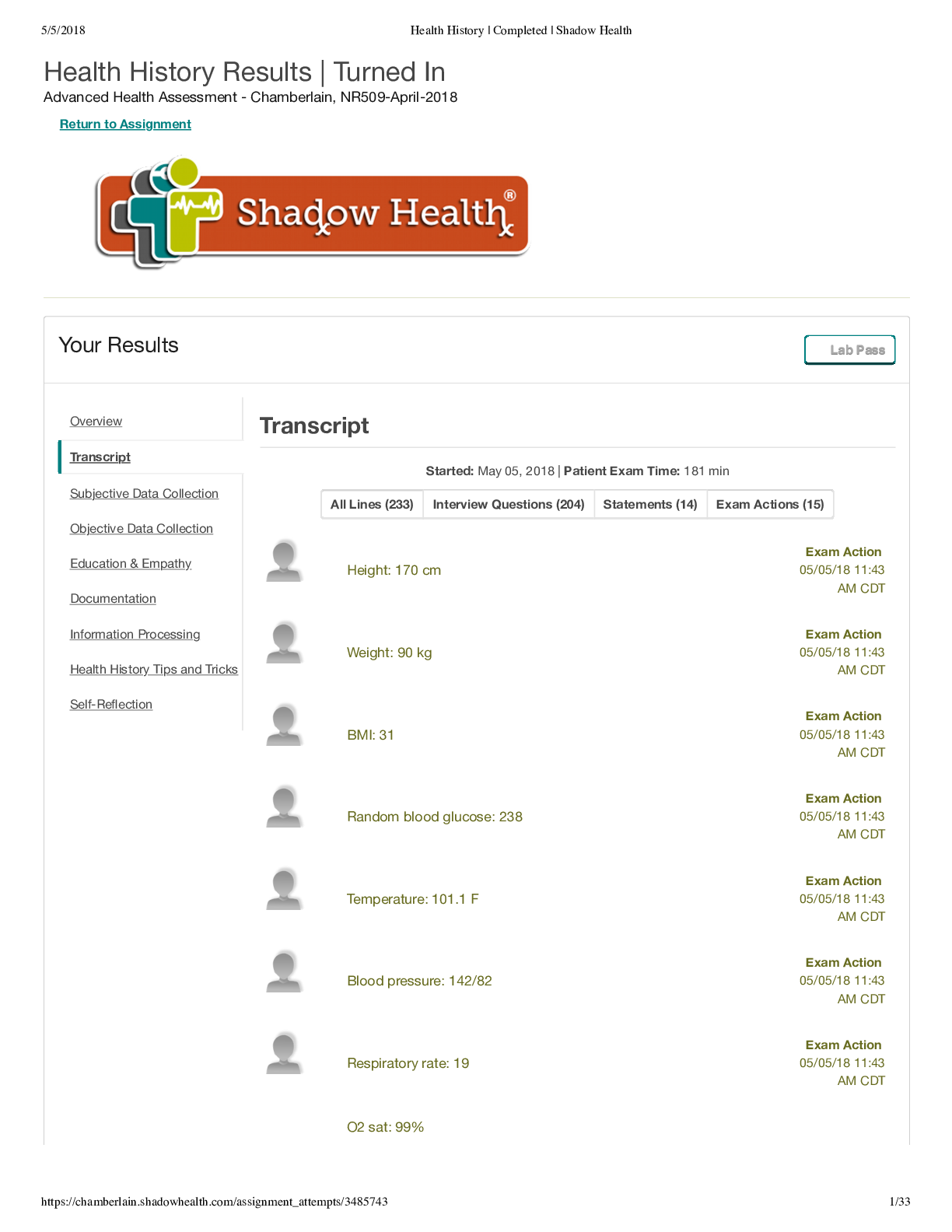
… Student: Hello! Diana Shadow: Hi. I’m Preceptor Diana. I will explain the details of this assignment and your objectives, just as a preceptor would in real life. Pay close attention to this in f... ormation as it will help guide your exam. At the end of this prebrief, you will answer a short question about the upcoming assignment. During the simulation, you may return to these instructions at any time by scrolling to the top of your transcript. Student: What is the situation? Diana Shadow: Your patient is Tina Jones:, a 28-year-old African American woman who has just been admitted to Shadow General Hospital for a painful foot wound. Your role in this simulation is that of a healthcare provider who will take Ms. Jones’ health history, a key component of her admission process. Student: What are my objectives in this assessment? Diana Shadow: A health history requires you to ask questions related to Ms. Jones’ past and present health, from her current foot wound to her pre-existing conditions. You will also want to review Ms. Jones’ systems, psychosocial history, and family medical history. These assessments together will give you a comprehensive picture of Ms. Jones’ overall health. If you discover any disease states, ask about symptoms and the patient’s experiences of them. Your questioning should cover a broad array of the symptoms’ characteristics. Throughout the conversation, you should educate and empathize with Ms. Jones when appropriate to increase her health literacy and sense of well-being. Regardless of whether you have assessed Ms. Jones previously, ask all questions that are necessary for obtaining a complete health history. While you should communicate with patients using accessible, everyday language, it is standard practice to use professional medical terminology everywhere else, such as in documenting physical findings and nursing notes. You may complete the exam activities in any order and move between them as needed. After obtaining Ms. Jones’ health history, you will complete an information processing activity. You will identify and prioritize diagnoses, then create a plan to address the identified diagnoses. Student: What else will this exam involve? Diana Shadow: You will complete nursing tasks to protect the patients safety, privacy, and health. You can document your findings, including vital signs, in the Electronic Health Record. This record provides necessary information for healthcare professionals who will continue patient care. Besides Subjective Data Collection, and Education and Empathy, there are activities within the simulation that provide valuable practice for their real-world counterparts, but they are not automatically graded by the simulation. Student: How will I be evaluated? Diana Shadow: In this assignment, you will be evaluated on your Subjective Data Collection, as well as your Education and Empathy. Your success in Education and Empathy is based on whether you promptly respond after identifying a moment worthy of therapeutic communication. The evaluation of your interview is dependent on how you word your questions therapeutically and precisely and explore all relevant topics with comprehensive breadth and depth. You will also be evaluated on your ability to collect data and form nursing diagnoses in the information processing activity. This assignment takes on average between 90 and 110 minutes. This exam may take longer than in real life, because in this safe simulation, students of all experience levels can take time to hone and review their skills. You can pause and resume the assignment at any time; your work is always saved automatically. Student: How does this assignment prepare me for the real world? Diana Shadow: In this assessment, you will become familiarized with the structure and content of a health history exam so that with real-life patients, you can: º ask effective and comprehensive questions º obtain a thorough health history º evaluate the patient’s risk of disease, infection, injury, and complications º educate and empathize º reflect on your experience and identify areas to improve º identify and prioritize nursing diagnoses º and develop a plan to address nursing diagnoses. Diana Shadow: In 1 or 2 sentences, answer this question to help prepare for the upcoming exam: Why is it important to obtain a patient’s complete health history? Student: So that you understand if there are any problems related to their chief complaint. Also, to help treat their current condition. Diana Shadow: Time to begin. … Patient Exam – Vital Signs: Height: 170 cm, Weight: 90 kg, BMI: 31, Random blood glucose: 238, Temperature: 102.4° F, Blood pressure: 138/90 mmHg, Heart rate: 90, Respiratory rate: 18, O2 sat: 98% Patient Exam – Interview: … Student: Hello, my name is Catlain, I am your nurse today. Tina Jones: Hey.Student: Can you confirm your name? Tina Jones: Tina Jones:. Student: Why did you come in today? Tina Jones: I got this scrape on my foot a while ago, and it got really infected. It’s killing me. Student: What additional symptoms have you experienced? Tina Jones: I mean, it’s all red and swollen, and there’s pus, it feels hot, it hurts like hell… It’s got all that going on. Show Less [Show More]
Last updated: 1 year ago
Preview 1 out of 60 pages
Instant download

Buy this document to get the full access instantly
Instant Download Access after purchase
Add to cartInstant download
Reviews( 0 )
Document information
Connected school, study & course
About the document
Uploaded On
Aug 12, 2021
Number of pages
60
Written in
Additional information
This document has been written for:
Uploaded
Aug 12, 2021
Downloads
0
Views
100