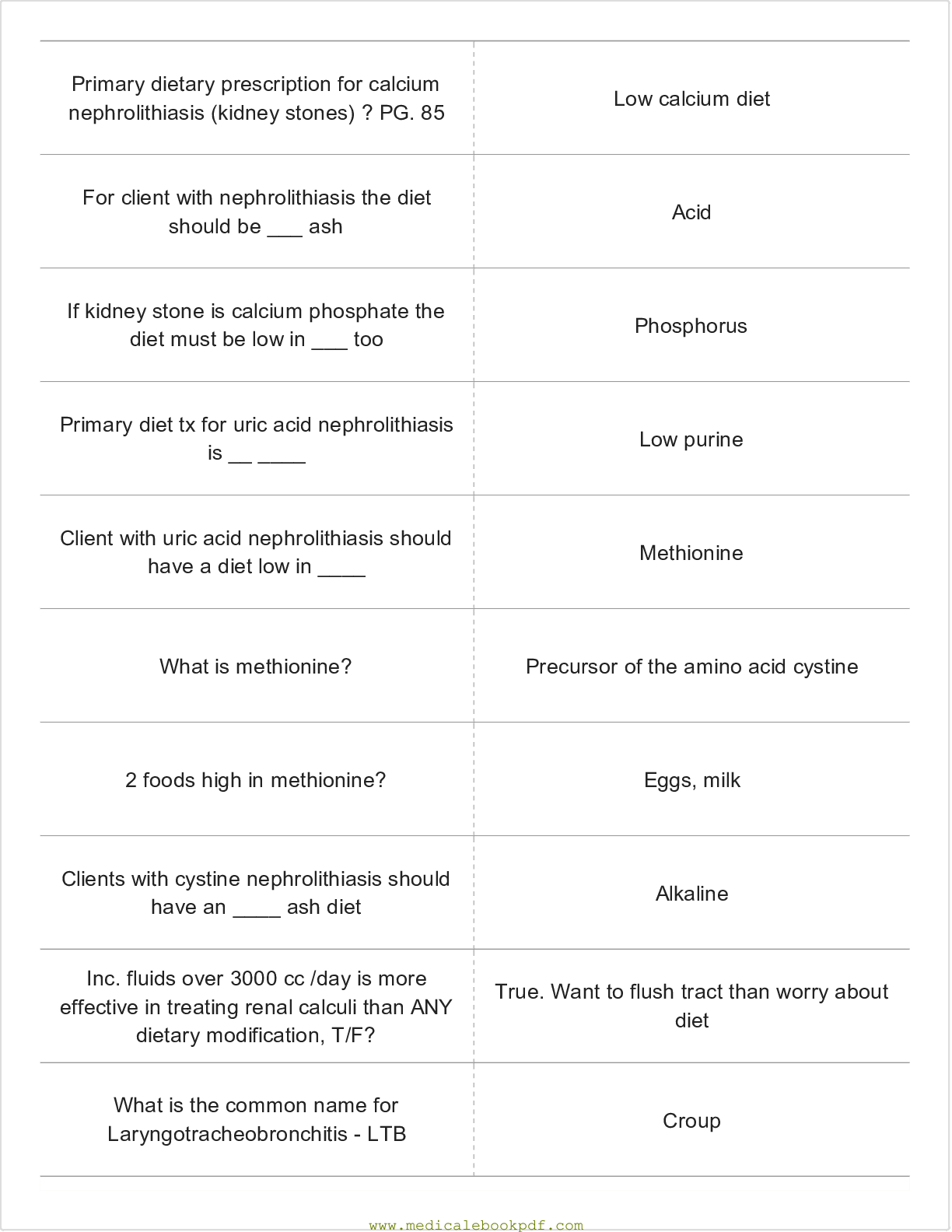
*NURSING > NCLEX > PASS NCLEX: Mark Klimek Blue book (ALL) NCLEX Study Guide 2000 Flashcards, Questions and Answers in (All)
PASS NCLEX: Mark Klimek Blue book (ALL) NCLEX Study Guide 2000 Flashcards, Questions and Answers in 123 pages. 100%.
Document Content and Description Below
Name the five/six essential nutrients The major source of energy for the body is carbs provide Kcalories per 1 gram Sucrose is a sugar found in What is glycogen? It is a ... stored formed of glucose/energy manufactured by the liver NO! It is a stored form of glucose MANUFACTURED by the liver. protein, fat burns The most concentrated source of energy for the . 9 Kcalories Fats carry vitamins A,D,E,K (Remember FADE K!) The nutrient needed most for growth and repair of tissues is . Proteins provide Kcalories protein (second best is Vit C) per 1 gram. Vitamins and minerals provide energy for the body. (T/F) False- they are necessary for a body's chemical reactions. True (even bone) 50 to 60% % of an adult's total weight? Name the four basic food groups Water acounts for to % of an infant's total weight? An individual is overweight if they are % above the ideal weight. Milk & Cheese, Meat & Legumes, Veggies & Fruits, Bread & Cereal 70 to 75% An individual is obese if 20 they weigh % above the ideal weight. What solution and material are used to cleanse the eyes of an infant? Can you use cotton swabs to clean the eyes, nares or ears of an infant? Can y With which body part do you begin when bathing an infant? When cleansing an infant's eye, cleanse from outer to inner canthus? Should you retract the foreskin of a 5 week old male, uncircumcised infant to cleanse the area? When sponge-bathing with tepid water the correct temp is Plain water, cotton balls, washcloths No, this is dangerous would cross contaminate 100 to 105 Lower body temperature during fever. Dropping water on inside surface of your forearm. Eyes always No, not until foreskin retracts naturally and without resistance- then it should be retracted, cleansed and replaced. . How long does it take for the umbilical stump to fall off? The primary reason why an infant is draped during the bath is to provide privacy. (T/F) You may use friction to remove vernix caseosa from an infant's skin. (T/F) 7 to 14 days False, the primary purpose of draping is to prevent chilling. False, it causes damage/bruising What solution is commonly used for care of umbilical cord? What cranial nerve is affected in Bell's Palsy? What is the #1 symptom of Bell's Palsy? Complete recovery from the paralysis of Bell's Palsy should occur in to 70acial paralysis 4 to 6 months. In addition to the facial paralysis, the sense of is also affected. Will the patient be able to close their eye on the affected side? Give three eye interventions for the client with Bell's Palsy. As the prostate enlarges it compresses the and causes urinary . At what age does BPH occur? What does BPH stand for? IN BPH the man has (increased/decreased) frequency of urination In BPH the force of the urinary stream is (increased/decreased). The man with BPH has taste no Dark glasses, artificial tears, cover eye at night Urethra, rentention men over 50 years of age Benign Prostatic Hypertrophy increased de forked with BPH has hesitancey. What does this mean? Will the man with BPH have enuresis, nocturia or hematuria? Difficulty starting to void Enuresis-No, Nocturia-Yes, and Hematuria-Maybe Enuresis inability to control the flow of urine and involuntary urination What is the best way to screen men for BPH? Should fluids be forced or restricted in BPH? Digital rectal exam forced What does TURP stand for? The most radical prostate surgery is the Transurethral resection of the prostate Perineal prostatectomy. What type of diet is used in BPH? Acid Ash Acid Ash diet Decrease pH (makes urine acid) Chz, eggs, Meat, fish, oysters, poultry, Bread, Cereal, Whole Grains, Pastries, Cranberries, Prunes, Plums, Tomatoes, Peas, Corn, Legumes. What is the primary purpose of a 3 way continuous bladder irrigation (CBI) after TURP? What solution is used for CBI? How fast do you run the CBI? What drug is use to treat bladder spasm? Should yodrain urine Normal saline (0.9 NaCl) At whatever rate it takes to keep the urine flowing and free of clots B&O suppositories (Belladonna & Opiates) No rectal temperatures, yes stool softeners Bright thick blood, persistent clots, persistent urine on dressing (don't call MD for transitory clots and urine on dressing.) urine drainage on the dressing. If you see an increase in blood content of urine coming out of the catheter, you would first . If you see clots in the tubing you would first . What exercises should the post prostectomy patient do upon discharge? Why? Will the post prostectomy patient be impotent? Pull carefully on the catheter to apply local pressure on the prostate with the Foley balloon. Increase the flow-rate. Perineal exercises, start and stop stream of urine, because dribbling is a common but temporary problem post op If TURP, no impotence, if perineal prostatectomy, yes impotence How often should the drainage bag be emptied? What is the most common problem due to catheterization? What is the most common organism to cause UTI with catheterization? What is the most common route for organisms to enter the blader when a catheterization is used? Name foods that make acid urine What is important about the level of the urinary drainage bag? How is the catheter taped in a male client? How is the catheter taped in a female client? What urinary pH prevents UTI? Should the Is urinary incontinence an indication for catheterization? Give three appropriate indications for bladder catheterization? What are the top 2 diagnoses for a client with a catheter? Which is #1? Up through the inside of the catheter in the days following catheterization Cranberry juice, apple juice (avoid citrus juices- they make alkaline urine) Never have the bag at a higher level than the bladder. To the lateral thigh or abdomen To the upper thigh Acidity, low pH No No Soap and water Keep the drainage system closed, do not disconnect junction of tubing Cloudy urine, foul smelling urine, hematuria No Urinary retention, to check for residual, to monitor hourly output #1- Potential for infection; Potential impairment of urethral tissue integrity What is systole? The MAXIMAL force of blood on artery walls What is diastole? The LOWEST force of blood on artery walls Accurate blood pressure is obtained by using a cuff that has width of of the arm. Which artery is most commonly used to measure blood pressure? Can the thigh EVER be used to obtain a blood pressure? When pressure is auscultated the first sound heard is the Yes, but this is rare. Systolic measurement. The change in the character of the sounds is known as the First diastolic sound The cessation of sounds is known as the Second diastolic sound When 2 values are given in a blood pressure the first is the nt. When 2 values are given in a blood pressue, the bottom number stands for the change in sounds or cessation of sounds? What is the normal adult blood pressure? Abnromally high blood pressure is called . What is the pulse pressure? The difference between the systolic and the diastolic blood pressure If you deflate a cuff TOO SLOWLY, the reading will be too high or low? Why? If you use too narrow of a cuff the reading will be too high or low? Vasoconstriction will blood High, venous congestion makes the arterial pressure higher (increases resistance) High pressure. Shock will blood pressure. Increased intracranial pressure will the pulse pressure. If my blood pressure is 190/110, what is my pulse pressure? What blood test must be done before a transfusion? What does a type and cross match indicate? What should the nurse measure before starting a transfusion? With what solution should blood be transfused? How many nurses are requried to check the blood? What happens when blood is administered with Dextrose IVs? If a transfusion reaction occurs what should the nurse do first? How long can a unit of blood be on the unit before it must be started? What should the nurse do with the IV line if transfusion reaction is suspected? If a transfusion reaction is suspected, what two samples are collected and sent to the lab? If a unit of blood is infused through a central line it must Decrease Increase or Widen 80 mmHg Type and cross match Whether the client's blood and donor blood are compatible. Vital signs 0.9 normal saline 2 nurses The cells clump together & don't flow well Stop the blood flow & start running the saline L Warmed be . Which of the following are signs of transfusion reaction? Bradycardia, Fever, Hives, Wheezing, Increased Blood Pressure, Low Back Pain What are three types of transfusion reactions Low back pain, wheezing, fever, hives H that can occur? What would you do first if you suspected transfusion reaction? What are the signs and symptoms of a hemolytic transfusion reaction? What are the signs and symptoms of a febrile transfusion reaction? What are the signs of symptoms of an allergic reaction to a transfusion? Give three reasons for a blood transfusion What does blood-typing mean? When does typing and cross matching need to be done? What does blood cross matching mean? When are hemolytic transfusion reactions likely to occur? When is a febrile reaction likely to occur? What test identifies Rh factor? What is the difference between whole blood and packed cells? What would you do if the client had an increasing temperature and was to get blood? How long should it take for one unit of blood to infuse? How long should you stay with the patient after beginning a transfusion? What blood type is the universal recipient? What blood type is the universal donor? Shivering, HA, low back pain, increased pulse & respirations, decreasing BP, oliguria, hematuria Low back pain, shaking HA, increasing temperature, confusion, hemoptysis Restore blood volume secondary to hemorrhage, maintain hemoglobin in anemia, replace specific blood components Check for surface antigen on the red blood cell Whenever a client is to get a blood product. It is only good for 24 hours. Mixing a little of the client's blood with the donor blood and looking for agglutination. In the first 10 to 15 minutes Within 30 minutes of beginning the transfusion Coombs test detects antibodies to Rh Packed cells don't have nearly as much plasma or volume as whole blood does Call the MD because blood is often held with an elevated temperature From one hour to three hours At least 15 to 30 minutes What is the routine for vital sign measurement with a transfusion? What IV solution is hung with a blood transfusion? What gauge needle is used with a blood transfusion? What other things are appropriate after a reaction? Can blood be given immediately after removal from refrigeration? With what solution & when should a breast feeding mother cleanse the areola? For a woman who doesn"t have retracted nipples, is towel drying or air drying better? The goal is for the infant to breast feed for minutes Once before administration Q15 x 2 after administration is begun Q1 x1 after transfusion has stopped 0.9 normal saline (No glucose) Large gauge, 18 gauge Call MD, get a blood sample, get urine sample, monitor vitals, send blood to lab No, it has to be warmed first for only about 20 to 30 minutes. Plain water, before & after each feeding Air drying of the nipples is best per side. How does the mother break the suction of the breast feeding infant? When should the breast feeding infant be burped? Assuming no mastitis, on which side should the breastfeeding begin? How long can breast milk be refrigerated? How long can breast milk be frozen? In what type of container should breast milk be stored? Can you microwave frozen breast milk in order to warm/thaw it? Which two nutrients is breast milk lower in? What should you tell a breast feeding mother about her milk supply when she goes home from the hospital? She inserts her little finger into the side of the infant's mouth After feeding from each breast Begin nursing on the side that the baby finished on the last feeding Sealed plastic bags Never Fluoride and iron Milk should come in postpartum day 3. Breastrfeed every 2-3 hours to establish good milk supply. Can a woman on oral contraceptives breastfed? What is another name for Buerger's disease? Which extremities are affected by it? Which sex does it affect the most often? The group with the highest incidence of Buerger's disease is . Upon walking the patient with Buerger's experiences . What is intermittent claudication? A first degree burn is pale or red? A first degree burn has vesicles (T/F)? A second-degree burn is pale or red? A second-degree burn is dull or shiny? A second-degree burn has vesicles? (T/F) A Second degree-burn is wet or dry? A third-degree burn is white or red? A third-degree burn is wet or dry? A third degre burn is hard or soft? Of first, second and third degree burns which has less pain? Why? For what purpose do you use the rule of nines? In the rule of nines, the head and neck receive : each arm Should not use OCP during the first 6 weeks after birth because the hormones may decrease milk supply. Estrogen is not recommended. Non-hormonal methods are recommended. Remember, breastfeeding is an unreliable contraceptive. Thromboangiitis obliterans Lower only Males Smokers Intermittent Claudication Pain in calf upon walking Red False Red Shiny True Wet White Dry Hard Third degree burns, nerve damage has occured To estimate the percentage of body surface burned; is NOT used for children. 9%, 9% receives . In the rule of nines, the 18%, 18%, 18%, 1% front trunk gets , the posterior trunk gets gets , each leg and the genitalia gets . What is the only IM given to a burn patient? In the emergent phase do you cover burns? (in the field) Should you remove adhered clothing? Name the 3 phases of burn Fluid moves from Tetanus toxoid- if they had a previous immunization; tetanus antitoxin- if they have never been immunized before (or immune globulin) Yes, with anything clean and dry. No Shock, diuretic, recovery Bloodstream, interstitial space the phase. to the in the SHOCK The shock phase lasts 24 to 48 hours for the first burn. to hours after a During shock phase of a burn is potassium increased or decreased? Why? What acid-base disorder is seen in the shock phase of a burn? What is the #1 therapy in the shock phase? What is the simple formula for calculating fluid replacement needs in the first 24 hours? If the MD orders 2,800 cc of fluid in the first 24 hours after a burn, one- of it must be infused in the first 8 hours. What blood value will dictate IV flow rate? How will you know the patient has entered the fluid mobilization or diuretic phase? How long does the fluid mobilization or diuretic phase of a burn last? In the diuretic phase, K+ levels fall or rise? If the nurse accidentally runs the IVs at the shock phase rate during the diuretic phase the patient will experience? Increased, because of all the cells damaged- the K+ is released from damaged cells. Metabolic Acidosis Fluid replacement/resuscitation 3cc X Kg X % burned per day Half (or 1,400 cc) The hematocrit The urine output will increase 2 to 5 days Fall- remember diuresis always causes hypokalemia Pulmonary edema The burn patient will be Hourly, weight on and daily Sulfamyon cream urine output . . Burns Silver nitrate cream . the Stains, skin Pain medications should be administered before care. When using silver nitrate, the dressings must be kept . What is Curlings ulcer? Why is it a problem in burn patients? What drug prevents it? In Abruptio Placenta, the placenta 30 minutes, wound care Wet It is a stress GI ulcer, you get these with any severe physical stress. Tagamet, Zantac, Pepcid (any H2 receptor antagonist), Protonix Prilosec Separates, prematurely the uterine wall . Abruptio Placenta usually occurs in from Multigravida, 35 (HTN, trauma, cocaine) (prima/multi) gravida over the age of . How is the bleeding of Abruptio Placenta different from that in placenta previa? If you are the nurse starting the IV on the client with Abruptia Placenta, what guage needle should you use? How often should you measure the vital signs, vaginal bleeding, fetal heart rate during Abruptio Placenta>? How is an infant delivered when Abruptio Placenta is present? Is there a higher or lower incidence of fetal death with Abruptio Placenta compared to Placenta Previa? In what trimester does Abruptio Placenta most commonly occur? usually pain; bleeding is more voluminous in previa 18 (in preparation to give blood if necessary) Q5-15 minutes for bleeding and maternal VS, continuous fetal monitoring, deliver at earliest sign of fetal distress Usually C-section Highter Third At what age are accidental poisonings most common? If a child swallows a potentially poisonous substance, what should be done first? Should vomiting be induced after ingestion of gasoline? When taking a child to the ER after accidental poisoning has occurred what must accompany the child to the ER? An elderly client is a (high/low) risk for accidental poisoning? What about a school age child? What types of chemicals cause burns to oral mucosa when ingested? Children at highest risk for seizure activity after ingestion are those who have swallowed 2 years old call medical help No- not for gas or any other petroleum products the suspected poison high - due to poor eyesight, high Lye, caustic cleaners drugs, insecticides and . Can impaired skin integrity ever be an appropriate nursing diagnosis when poisoning has occurred? What is the causative organism of acne? What structures are involved in acne vulgaris? Name 3 drugs given for acne? Dietary indiscretions and uncleanliness are causes of acne? What are the 3 causative factors in acne vulgaris? Uncleanliness is a cause of acne? What is the most common retinoid given to people with acne? Yes, when lye or caustic agents have been ingested P. acnes (propionibacterium acnes) The sebaceous glands Vitamin A, Antibiotics, Retinoids False Heredity, Bacterial, Hormonal False Accutane Accutane is an analog of which vitamin? What is the most common side effect of accutane? And what is most important in health teaching in adminstration? What is the antibiotic most commonly given to clients with acne? How long will it take for the person to see results when acne is being treated? Does stress make acne worse? How often should the client with acne wash his face each day? What instructions do you give to a client taking tetracycline? Vitamin A Inflammation of the lips; Causes birth defects Tetracycline 4 to 6 weeks yes twice a day Take it on an empty stomach and avoid the sunlight (photosensitivity) What are comedones? Blackheads and white heads What virus causes AIDS? The AIDS virus invades helper . AIDS is trasmissible through what four routs? HIV is present in all body fluids? Name the 5 risk groups for AIDS What is the first test for HIV antibodies? What test confirms the ELISA? Which test is the best indicator of the progress of HIV disease? A CD4 count of under is associated with the onset of AIDS-related symptoms. A CD4 count of under is associated with the onset of opportunistic infections. HIV - Human immunodeficiency virus T-lymphocytes (or CD4 cells) blood, sexual contact, breast feeding, across placenta in utero Yes, but not transmitted by all, only blood, semen and breast milk Homosexual/bisexual men, IV drug users, hemophiliacs, heterosexual partners of infected people, newborn children of infected women ELISA Western Blot CD4 count 500 200 Give 6 symptoms of HIV disease. Which 2 classes of drugs are given in combination for HIV sero-positivity? NRTI (nucleoside reverse transcriptease inhibitors) Anorexia, fatigue, weakness, night sweats, fever, diarrhea NRTI's (nucleoside reverse transcriptease inhibitors) and PI's (protease inhibitors) They prevent viral replication. an antiviral drug used against HIV (is incorporated into the DNA of the virus and stops the building process; results in incomplete DNA that cannot create a new virus; often used in combination with other drugs) PI's (Protease inhibitors) most potent of antiviral meds, inhibit cell protein synthesis that interferes with viral replication, does not cure but slows progression of AIDS and prolongs life, used prophylactically, used in AIDS to decrease viral load and opportunistic infections What do NRTI's and PI's do? What does the physician hope to achieve with NRTI's and PI's for HIV? What is the most common NRTI used? What is the most challenging aspect of combination of drug therapy for HIV disease? Clients with AIDS (gain/lose) weight? The typical pneumonia of AIDS is caused by They prevent viral replication A delayed onset of AIDS for as long as possible (usually can delay onset for 10- 15 years) AZT (zidovudine) The number of pills that must be taken in 24 hours can be overwhelming. The frequency also makes it hard to remember-an alarm wristwatch is used. lose Pneumocystic carinii . What type of oral/esophageal infections do AIDS patients get? What is the #1 cancer that AIDS patients get? Kaposi's sarcoma is a cancer of the Candida Kaposi's sarcoma skin . T/F: AIDS patients get lymphomas? What lab findings are present in AIDS? If the AIDS patient has leukopenia they will be on True Decreased RBC's, WBC's and platelets protective (reverse) isolation . Define Leukopenia decrease in wbc, indicated viral infection Without leukopenia the AIDS patient will be on Standard precautions or blood and body fluid precautions precautions. When the AIDS patient has a low platelet count, what is indicated? Does AIDS require a single room? When do you need a gown with AIDS? When do you need a mask with AIDS? When do you need goggles with AIDS? If an AIDS patient's blood contaminates a counter top, with what di you clean? Are all articles used by AIDS patients double- bagged? Can AIDS patients leave the floor? Is dietary protein limited in AGN? bleeding precautions; No IM's, no rectal temperatures, other bleeding precautions Yes - if WBC counts are low If you are going to get contaminated with secretions Not usually unless they have an infection caused by an airborne bug Suctioning, central line start, arterial procedures 1:10 solution of bleach and water no - only those contaminated with secretions Yes, unless WBC's are very low Not usually, however if there is severe azotemia then it may be restricted Define azotemia? nitrogenous wastes in the blood (increased creatinine, BUN) What is the best indicator of renal function? Do people recover from AGN? How can AGN be prevented? What is the most important intervention in treating AGN? What is the most common dietary restriction for AGN? What are the urinaysis findings on AGN? How long after strep infection does AGN develop? How do you assess fluid excess in the child with AGN? The serum creatinine Yes, the vast majority of all clients recover completely from it By having all sore throats cultured for strep and treating any strep infections Bedrest - they can walk if hematuria, edema and hypertension are gone. Moderate sodium restriction. Fluid restriction is #2 if edema is severe. Hematuria Proteinuria +3 to +4 Specific gravity Up 2 to 3 weeks after initial infection Daily weight What organism causes acute glomerular nephritis? What happens to the kidney in AGN? How often are vital sign measurements taken in AGN? Will the client have hypo or hyper tension with AGN? Why? What are the first signs of AGN? What are the three adult stages of development called What is the age range for early adulthood? What is the age range for middle adulthood? What is the age range for late adulthood? What is the developmental task for early adulthood? What is the developmental task for middle adulthood? Group A beta hemolytic strep It becomes clogged with antigen-antibody complexes which then cause inflammation and loss of function. Q4 hours with blood pressure Hypertension, because of fluid retention Puffiness of face, dark urine early adulthood, middle adulthood and later adulthood 19 to 35 years of age 35 to 64 years of age 64 years of age to death Intimacy vs. Isolation Generativity vs. stagnation. Intimacy vs. Isolation Erikson's stage in which individuals form deeply personal relationships, marry, begin families Generativity vs. Stagnation What is the developmental task for later adulthood? Erikson's stage of social development in which middle-aged people begin to devote themselves more to fulfilling one's potential and doing public service Ego Integrity vs. Despair Ego Integrity vs. Despair (Erikson) People in late adulthood either achieve a sense of integrity of the self by accepting the lives they have lived or yield to despair that their lives cannot be relived "Time is too short to start another life, though I wish I could," is an example of despair . "If I had to do it over again, I'd life my life just about the same," is an example of Ego Integrity What does AKA mean? Above the knee amputation What does BKA mean? Below the knee amputation If the patient had an AKA they should lie several prone (to prevent flexion contracture) times per day. The #1 contracture problem in AKA is of the flexion, hip What will prevent hip flexion contracture after AKA? What is the #1 contracture problem after BKA? How do you prevent flexion contracture of the knee after BKA? To prevent post-op swelling, the stump should be . How long should the stump be elevated to prevent post op swelling? How often should a stump be washed? When a stump is wrapped, the bandage should be tightest and loosest . If after a right BKA, the client c/o pain in his right tow, he is experiencing . When will phantom limb sensation subside? Name ways to toughen a stump so it will not breakdown due to the wear of the prosthetic leg? An aneurysim is an abnormal Lying prone several times a day Flexion of the knee Remide the patient to straighten their knee constantly while standing elevated 12-24 hours daily distally (far from the center), proximally (neareast to the point) phantom limb sensation (which is normal) in a few months push the stump against the wall, hitting it with a pillow widening (it is also weakening) of the wall of a(n) artery. What artery is widened in a thoracic aneurysm? the aorta An aneurysm can result from an and from infection, syphilis . The most common symptom of abdominal aneurysm is: Which aneurysm is most likely to have no symptoms? Which vital signs are most important to measure in clients with aneurysm? An aneurysm will most affect which of the following, the blood pressure or the pusle? What activity order is the client with an aneurysm supposed to have? If the client with aneurysm is physically unstable, should you encourage turning, coughing and deep breathing? What class of drugs is the client with an aneurysm most likely to be on? What is the BIG danger with aneurysms of any type? If an aneurysm is ruptured how would you know it? If an aneurysm ruptures what is the #1 priority? Is there anything that can be done for the client with a ruptured aneurysm before they get to the operating room? The post op thoracic aneurysm is most likely to have which type of tube? The post op abdominal aneurysm repair client is most likely to have which type of tube? a pulsating mass above the umbilicus the abdominal is most often "silent" The pulse and blood pressure the pulse (many times the aneurysm will rupture and much blood will be lost before the blood pressure starts to change. Bedrest. do not get these people up no, bedrest until the client is stable! Antihypertensives Rupture, leads to shock and death decreased LOC (restlessness), tachycardia, hypotension - all signs of shock Get them to the operating room ASAP Yes, if available you can get them into antishock trousers but not if this causes a delay in getting them to the operating room Chest tube, because the chest was opened NG tube for decompression of bowel If you care for a client who is post-op for a repair of a femoral popliteal resection what assessment must you make every hour for the first 24 hours? What causes angina pectoris? Describe the pain of angina pectoris What drug treates angina pectoris? How do you tell if a client has angina or an MI? How many nitro tabs can you take before you call the doctor? How many minutes should lapse between the nitro pills you take? By what route do you take nitro? What is the action of nitro? What are the top 2 side effects of nitro? What precaution must the nurse take when administering topical nitro paste? Everyone with angina needs bypass surgery? t/f Anorexics are usually under the check the distal extremity (far from center) for color, temperature, pain and PULSE, also MUST document Decreased blood supply to myocardium, resulting in ischemia and pain crushing substernal chest pain that may radiate Nitroglycerine the pain of the two is similar, the way to tell the difference is if nitro and rest relieve the pain. For angina, nitro and rest relieve the pain, for MI, nitro and rest do not relieve the pain 3 5 minutes - take one nitro tab every 5 minutes 3 times, if no relief, call MD sublingual dilates coronary arteries to increase blood supply (O2 supply) and reduces preload. headache and hypotension wear gloves, nurse may get a dose of the med False females, 25 age of . The diagnosis is made when there is a weight 15 (weigh < 85% of normal body weight), hospitalize if 30% weight loss loss of % or more of body weight. A major mental/emotional nursing diagnosis seen in anorexia nervosa is . The pulse rate of anorexics is tachycardic or bradycardic? Altered body image Bradycardic List the most common gynecologic symptom of anorexia nervosa? What is found over the body of the client with anorexia nervosa? What is the top priority in the care of the client with anorexia nervosa? The best goal to evaluate the progress of the client with anorexia nervosa? amenorrhea lanugo (soft downy hair) intake of enough food to keep them alive, have them gain weight an adequate weight gain What is the apgar scale? quick objective way to evaluate the vital functions of the newborn When is apgar scoring performed on infants? Name the 5 criteria that are recorded on an apgar scale The total apgar score can range from The maximum score and infant can receive on any one of the criteria is A 10 on the apgar means the baby is A 0 on the apgar means the baby On heart rate or cardiac status, a 2 means that the HR is above BPM. On the HR criteria an infant scores a "1" if their at one minute and again at 5 minutes after the birth Cardiac status, respiratory effort, muscle tone, neuromuscular irritability, and color 0 to 10 2 in terrific health is stillborn 100 greater, less than HR is and than 0 100 In order to score a 0 on HR the infant must have a rate of . A high score of 2 is given for respiratory effort if the newborn _. An infant is given a score of 1 if their respirations are or . An infant is given a Zero Cries vigorously Slow or irregular They do not breathe score of 0 for respiratory effort if . In order to get a score of 2 on muscle tone the infant must . To get a score of 1 on the APGAR for muscle tone the newborn must place their extremities in . A newborn receives a score of 0 on muscle tone when there is To score the maximum of 2 points on nueromuscular reflex irritability the infant must . If the neonate , they will Move spontaneously (actively) Flexion No movement (limp) Cry Grimaces score a 1 on neuromuscular irritability. To receive a 0 on reflex (neuromuscluar) irritability the neonate must exhibit To score a maximum score fo 2 on color the child must be No response Totally pink If the child's are . and the Extremities are blue (cyanotic), Pink trunk -face abdomen are , the child scores 1 on color To get a 0 on color the infant is Totally blue, pale Acrocyanosis Temporary cyanotic condition, usually in newborns resulting in a bluish color around the lips, hands and fingernails, feet and toenails. May last for a few hours and disappear with warming. Apendicitis is an of the appendix due to . Apendicitis occurs most in what age group? What is the most common complication of appendicitis? inflammation, obstruction 15 to 35 Peritonitis Peritonitis inflammation of the peritoneum What is the first sign of appendicitis? What follows the RUQ abd pain of appendicitis? Where does the pain of appendicitis finally end up? What is the name of the RLQ abd pain where appendicitis pain finally localizes? What is present when rebound tenderness is present? What is the hightes that the temp will be in appendicitis? What blood count is elevated in appendicitis? What is the name for an elevated WBC? What is the only treatment recommended for appendicitis? Before the client with suspected appendicitis sees the physician what should be avoided? To lessen pain place the client in position. Never apply to the area of the appendix. After appendectomy, document in the nurses notes the return of right upper quadrant pain N/V RLQ McBirney's point Peritoneal inflammation 102 F WBC Leukocytosis surgery - appendectomy pain meds, enemas, laxatives, food! NPO fowlers (a sitting position) (also use post op) heat (it causes rupture) bowel sounds (peristalsis) What is the primary dietary prescription for calcium nephrolithiasis? For the client with calcium nephrolithiasis the diet should be ash. If the kidney stone is calcium phosphate the diet must be low in too. The primary diet treatment for uric acid nephrolithiasis is Low calcium diet Acid Phosphorous Low pruine - . The client with uric acid nephrolithiasis should have a diet low in . Methionine What is methionine? The precursor of the amino acid cystine (precursor = material out of which something is made) Name two foods high in methionine. Clients with cystine nephrolithiasis should have a (n) ash diet. Increasing fluids to over 3000 cc per day is more effective in treating renal calculi ( kidney stones) than any dietary modification. (T/F) Neoplasm refers to benign and malignant tumors. (T/F) Which type of tumor is more malignant? Differentiated or undifferentiated? When cancer spreads to a distant site it is called? The cause of cancer is known. (T/F) A person should have a yearly work up exam for cancer detection over Milk, eggs Alkaline True. It's more important to flush the urinary tract than worry about what you're eating. True Undifferentiated is worse to have (highly differentiated is better to have) Metastasis False 40 the age of . In general, cancer drugs have side effects in which three body systems? What are the 3 most common chemotherapeutic GI side effects? Clients receiving chemotherapy must be NPO. (T/F) Is it permissible to give lidocaine viscous ac (before meals) if the patient has chemotherapeutic stomatosis? (T/F) With what solution should the client with chemotherapeutic stomatitis rinse pc (after meals)? GI Hematologic (blood) Integumentary N/V Diarrhea Stomatitis (oral sores) False True H2O2 - hydrogen peroxide What lubricant can safely be applied to the cracked lips of chemotherapy stomatitis? Name the 3 hematologic side effects of chemotherapy. Which cells are low in thrombocytopenia? What drug should NOT be given to the patient with chemotherapeutic thrombocytopenia? When should the nurse WITHHOLD IM injections in the client on chemotherapy? What are the 3 objective symptoms/signs of thrombocytopenia? Hint: P.E.E. K-Y Jelly Thrombocytopenia Leukopenia Anemia Platelets ASA (aspirin) Only when their PLATELET count is down. Petechiae Epistaxis Ecchymosis What is epitaxis? Nose bleeds What is ecchymosis? Bruising What is petechiae? Small dot like pinpoint hemorrhages on the skin. What blood cell is low in leukopenia? When the Absolute Neutrophil Count ANC is White blood cells 500 below person on the chemotherapy will be placed on reverse isolation. What is the #1 integumentary side effect of chemotherapy? Alopecia What is alopecia? Hair loss The hair loss due to chemotherapy is usually temporary? (T/F) Can scalp tourniquets prevent chemotherapy alopecia? Can ice packs to the scalp prevent chemotherapy alopecia? CD ranks among the leading cause of maternal death. True In some cases, yes In some cases, yes Fourth What is the #1 cause of CD of pregnancy? Pregnancy requires a increase in the cardiac output. What is the #1 cause of maternal death in CD of pregnancy? What is meant by decompensation? What will you see when you observe the neck of a client with CD of pregnancy? What will you hear when you auscultate the heart of the client with CD of pregnancy? What will you hear when you auscultate the lungs of the client with CD of pregnancy? If the client with CD of pregnancy experiences sudden heart failure what is the MOST common thing you will see? What is the #1 treatment of CD during pregnancy? What are the three most common drugs given to women with CD in pregnancy? Why are diuretics given to women with CD of pregnancy? Why are anticoagulants (heparin only) given to women with CD of pregnancy? Why is digitalis given to women with CD of pregnancy? Can a woman with CD of pregnancy be given analgesics during labor? Can morphine be given to a woman with CD during labor? Rheumatic heart disease 30-50% Decompensation Failure of the heart to maintain adequate circulation. Distended neck veins -JVD Murmurs Crackles-rales Sudden onset of SOB (dyspnea). Rest Diuretics Heparin Digitalis To promote diuresis which will: -lower circulating blood volume -decrease preload -decrease the amount of blood the heart pumps. To prevent thrombophlebitis due to venous congestion, usually in legs. To increase the strength of the heart and to decrease the rate, rest the heart while making it more efficient Yes, in fact they should be given analgesics, may get too anxious which is bad for the patient Yes, even though it negatively affects the fetus, remember morphine decreases preload and pain which rests the heart. What is the most common dietary modification for the woman with CD who shows signs of decompensation? Is a C-section mandatory for delivery of a woman with CD of pregnancy? Second to rest, what is very important treatment for CD of pregnancy? How long must the woman with CD of pregnancy be on bed rest after delivery? What nutrients should be supplied in the diet of the pregnant woman with CD? What are the two most common subjective complaints of the woman who is decompensating during labor? In addition to the things you assess for in every woman during labor, what additional assessment must you make for a woman with CD? How often must you assess the lung sounds during the first stage of labor? During active labor? During transition labor? In which position should a woman with CD in labor be? The nurse should limit the client's efforts to Decreased sodium, decreased water (restriction) No Weight control At least one week Iron Folic acid Prevent anemia (anemia always makes the heart work more) SOB Palpitations You must assess lungs sounds frequently Every 30 to 10 minutes Semi recumbent, HOB up Bear down during labor when CD is present. What is the big danger to staff when caring for a client with cesium implant? Radiation hazard What are the three principles to protect yourself from radiation hazard? Will the woman with a cesium implant have a foley? From where should the nurse provide care to the client with cesium implant? How can the woman with cesium implant move in bed? What four symptoms in a patient with a cesium implant should be reported to the physician? Should pregnant staff care for a client with a cesium implant? Can the woman with a cesium implant have the HOB elevated? From where should the nurse talk to the client? Is bed rest necessary when a woman has cesium implant in place? What type of diet is this woman with a cesium implant on? No nurse should attend the client with a cesium implant more than per day. What would you do if the cesium implant came out? Should the nurse provide perineal care for the client with a cesium implant? What part of your hand do you use to handle a wet cast? Upon what do you support a cast while it dries? Distance Shielding Time Yes The head of the bed Only from side to side Profuse vaginal discharge Elevated temp Nausea Vomiting (these indicate infection and perforation) No Yes, only 45 degrees maximum The entrance to the room Yes, absolute bed rest Low residue (decrease bowel motility ) 1/2 hour Pick it up with forceps only - never touch with hand even if you are wearing gloves. No, risk of radiation hazard The palm Pillows (no plastic covers) How long does it take a cast to dry? Should you cover a wet cast? Should you use a heat lamp or hair dryer or fan to help dry a cast? What signs or symptoms would you report if they were present after cast application? If there is inflammation under a cast, it will be evident in a spot. To prevent irritation of the skin near the edges of a cast the edges should be 24 hours No No heat lamp and hair dryer Yes fan Numbness Tingling Burning Pallor Unequal or absent pulses Unequal coolness Hot Petaled . What type of cast causes cast syndrome? What causes cast syndrome? What is the #1 symptom of cast syndrome? What is the #1 treatment of cast syndrome? A dry cast is gray or white? A dry cast is dull or shiny? A dry cast is dull or resonant to percussion? Traction is used to A body cast Anxiety and stress leading to sympathoadrenal shut-down of the bowel Nausea and vomiting due to bowel obstruction NPO and NG tube for decompression White Shiny Resonant Reduce and immobilize, muscle spasm; and fracture, relieve prevent a and . deformities Can skin traction be removed for skin care? Can the client be removed from skeletal traction? Name 3 types of skin traction Name 3 types of skeletal traction Yes No Bucks Bryants Pelvic Cranial tongs Thomas splints with Peason attachments 90 degrees to 90 degrees What type of traction is most commonly used for hip fracture in adults? What type of traction is most commonly used for hip fractures in children? In what position should the bed be if the patient is in pelvic traction? To insure that Bryant's traction is working the child's hip/sacrum should be What is the advantage of balanced counteraction? Patients in Russell's traction are particularly prone to . When a patient is in a Bucks Bryants Semi-fowlers with knee gatched Off the bed enough to slip a hand between the sacrum and the bed. You can easily move the patient around in bed Thrombophlebitis Unaffected Buck's traction they may turn to the side. Define cataract Opacity of the crystalline lens Is surgery done immediately upon diagnosis of cataract? What three most common visual defects occur with cataract? What are the two common treatments of cataract? What does the eye look like when a client has cataracts? What will the client be wearing after cataract surgery? When the client asks about the use of glassess or contacts after cataract surgery what would you say? What will be a high priority nursing diagnosis for a client post cataract surgery? Should the client ambulate independently after cataract surgery? No, they usually wait until it interferes with ADLs . Cloudiness Diplopia (double vision) Photophobia (sensitivity to light) Laser, surgical removal. Surgery called intraocular or extraocular lens extraction Cloudy, milky-white pupil A protective patch/shield on the operative eye for 24 hours, then a metal shield (AT NIGHT only) for 3 weeks If an introcular lens is implanted they will NOT need glasses. If no lens is implanted, then contacts will be fitted for 3 months post-op, temporary thick glasses given immediately but will get a different prescription in 2 to 3 months Safety No the patient should not ambulate independently, depth perception is altered. What positions are to be avoided after cataract surgery? What are the post- operative signs of hemorrhage into the eye? What movements are to be avoided after cataract surgery? What positions are okay after cataract surgery? Should you use talcum powder with a post- operative cataract client? What are the three signs of increased intraocular pressure? What is the major objective in caring for a client after surgical cataract removal? When the lens is to be extracted for cataracts, what drugs are given preoperatively? What three drugs are given post-operatively for surgical cataract removal? Give five causes of catarcts? Celiac's disease is a disease The client with celiacs cannot Lying face down. Also, do not lie on operative side for a month. Severe pain Restlessness Coughing Sneezing Bending at the waist Straining at stool Rubbing or touching eyes Rapid head movements Do not lie on operative side; do not lie on back No, it may cause sneezing; also should avoid pepper. Pain (moderate to severe) Restlessness Increased pulse rate To prevent pressure in or on the eyes Mydriatics Dilators Antibiotic drugs (gtts) Stool softeners Antiemetics Analgesics (mild to moderate) Injury Congenital Exposure to heat Heredity Age Malabsorption Gluten tolerate Gluten is a . . Protein What does gluten do to the intestines of the client with celiac's disease? The stools of a client with celiac's disease are , and - . It destroys the lining of the intestine. Large Greasy Foul-smelling Clients with celiac's disease do not absorb what mineral? Clients with celiac's disease don't absorb fats; therefore they don't absorb Iron Fat soluble vitamins . What are the four fat- soluble vitamins? Malabsorption of which vitamin leads to bleeding disorder? What will the abdomen of clients with celiac's disease look like? What is the #1 treatment of celiac's disease? Veggies are allowed or not allowed in diet of client with Celiac's disease? Fruits are allowed or not allowed? Grains of all kinds are prohibited. (T/F) What grains are allowed in a gluten-free diet? What grains are not allowed in a gluten-free diet? Are foods made with wheat, oat, or rye flour allowed? Is milk allowed on a gluten-free diet? Are meats allowed on a gluten-free diet? Are eggs allowed on a gluten-free diet? Is commercial ice cream allowed on a gluten-free diet? Are puddings allowed on a gluten-free diet? Which soups are not allowed on a gluten free diet? A,D,E,K Vitamin K, remember do not mix up potassium with Vitamin K Distended with flatus Gluten-free diet Allowed Allowed False Rice and corn Wheat Oats Rye Alfalfa Barley No Yes Yes, but watch for breaded meats and hot dogs/lunch meats- may have grain in them and are not allowed Yes No, even though it is a milk product, commercial ice cream has GRAIN in it. No, for the same reason ice cream isn't. Creamed soups- these often have flour The #1 problem with central lines Infection How often should central line dressings be changed? What type of dressing is applied to a central line insertion site? Can drugs be piggybacked into central --TPN? When changing central line tubing the patient should be told QOD- every other day Sterile occlusive No, use another lumen. Turn his head away from the site, hold breath, and perform the Valsalva maneuver to ? If a central line is found accidentally open the patient should be positioned on his . A CVA is a of the brain cells due to decreased Left side Destruction; blood flow and oxygen and . Women have a (higher/lower) incidence of stroke than men? Name the three types of CVA Use of oral contraceptives increases the risk of CVA (T/F). Chronic abuse of alcohol increases risk of CVA. (T/F) Obesity increases risk of CVA (T/F) Smoking increases the risk of CVA. (T/F) Atrial fibrillation increases the risk of CVA (T/F) Lower Embolus Thrombus Hemorrhage True False True True True, emboli particularly What is a TIA? Transient Ischemic Attack Warning sign of impending CVA (transient neurologic deficits of any kind can last 30 seconds to 24 hours) Do patients experiencing a CVA have a headache? Yes The first sign of CVA is usually a . The activity order in early management of Change in LOC Absolute Bed Rest CVA is . The patient with a recent CVA is most likely to have fluids restricted or forced? How far should the HOB be up after CVA? Can the stroke victim be turned side-to-side? How often should the CVA patient be turned or repositioned? The CVA patient should be turned onto his paralyzed side no longer than 2 hours. (T/F) ROM exercises should occur every 2 hours in CVA patients. (T/F) To prevent urinary incontinence; the CVA patient should be catheterized. (T/F) Which type of paralysis is typical of CVA- paraplegia, hemiplegia or quadriplegia? What anatomical fact accounts for the left side of the body being controlled by the right brain? If the patient has right hemiplegia, he cannot Restricted 30 degrees Yes Every 2 hours False, the patient should not be on their paralyzed side for more than 20 minutes. False-- every 4 hours or 3 times a day is enough False- remember incontinence will never be allowed as a reason for catheterization Hemiplegia The motor-pyramidal-tracts cross over to the other side (decussate in the medulla) Right arm and right leg, left move his and the and stroke was on the side of the brain. What is hemianopsia? Not being able to see one half of the field of vision. The client with hemianopsia should be taught to Scan . What is scanning? Moving the head from side to side to see the whole field of vision. If the client has right homonymous hemaniopsia, the food Right on the side of the tray may be ignored. After meals, the nurse must always check of the CVA Mouth (cheek), food client for . Should a CVA patient have all four side rails up at all times? Should they be restrained? When a patient does not understand INCOMING language he is said to Side rails yes. Restraints- no, unless they are a danger to themselves or others Receptive have aphasia. When the CVA client understands your question but can't respond verbally correctly, he is said to have aphasia. Expressive What is global aphasia? Both receptive and expressive Aphasia is most common if the stroke occurred in the (dominant/non- dominant) hemisphere of the brain. How do you tell which side of the person's brain is dominant? For which type of aphasia are slow, short, simple directions most useful? For which type aphasia is careful listening and needs anticipation most useful? The loss of the ability to perform purposeful, skilled acts, ie brushing teeth, is called . Cytoxan cyclophosphamide Dominant It is the side that controls their dominant hand, ie, a left handed person has a dominant right hemisphere and conversely a right hand person has a dominant left hemisphere Receptive Expressive Apraxia Hemorrhagic cystitis Cisplatin Peripheral neuropathy, constipation, ototoxicity Bleomycin Pulmonary fibrosis Adriamycin Cardiotoxicity Vincristine Peripheral neuropathy (foot drop, numbness and tingling, hoarseness, jaw pain) constipation (adynamic ileus due to neurotoxicity) DTIC- dome Flu-like symptoms Chemo-therapeutic Agent Toxicities Methotrexate Toxic to just about every organ except to heart, toxicity made worse with aspirin The infant fears most when hospitalized. The toddler fears most when hospitalized. The preschooler fears separation as well as when hospitalized. The toddler and preschooler will think that illness is caused by . The school-aged hospitalized child is afraid of separation from . The school-aged child perceives the cause of illness to to be external or internal? The adolescent who is hospitalized fears separation from and loss of . Preschoolers may require physical restraint during painful procedures. (T/F) Which age group engages in stalling tactics before painful procedures most? Which age groups are most likely to physically resist the nurse during procedures? Separation from love object Separation from family Mutilation- remember preschoolers have vivid imaginations...fantasy Something they did wrong. Age group External, she knows that illness is not a result of bad behavior. Peers, independence True School-Age School-age, adolescents Toddlers may require physical restraint for painful procedures. (T/F) The meats that are highest in cholesterol True Organ meats liver, heart, brains, kidneys are meats. The meats that are second highest in cholesterol are the Shell seafood- shrimp, crab, lobster Egg white is (high/low) in cholesterol? Egg yolk is (high/low) in cholesterol? The three meats lowest in cholesterol are , Low High Chicken, pork, mutton and . Milk is (high/low) in cholesterol. Is cheese high in cholesterol? Which oils are high in cholesterol? Is cholesterol a triglyceride? Do plant foods contain any cholesterol? Low Only moderate, not really that high Animal oils No No, not many What is otitis media? Chronic infectious/inflammatory disease of the middle ear Is otitis a disease of the adult or child? What part of the ear is involved in otitis media? What are the 2 common subjective signs of otitis media? What are the 2 common objective signs of otitis media? What commonly happens secondary to otitis media? Do all the children with otitis media need tubes in their ears? What are the two most common medical treatments for otitis media? What is the most severe complication of otitis media? Usually the child Middle ear Hearing loss Feeling of fullness in the ear Hyperpyrexia (fever) Drainage from ear Perforation of the ear drum No Systemic antibiotics Antibiotic ear drops Meningitis or mastoiditis What is cholesteatoma? An epidemial cyst in the ear highly associated with otitis media. What are the restrictions to be followed when tubes are in a child's ear? No swimming, no showering, no diving What is cleft lip? The lip is open to the nares What is cleft palate? The roof of the mouth is open to the nasopharynx. Is it possible to have only one: cleft lip or cleft palate? When will the cleft lip be repaired? When is cleft palate repaired? Why is cleft lip repaired early? Describe the nipples on bottles used to feed babies with cleft lip? The infant with cleft lip/palate needs more frequent . Children with cleft lip/palate should be fed in what position? What is the #1 complication of cleft lip/palate? Children with cleft lip and cleft palate have long-term problems Yes, you can have one or or the other or both Between 10 weeks and 6 months Between 1 and 5 years of age Feeding is easier after repair and appearance after repair is more acceptable to parents. Large-holed, soft nipples Bubbling, burping An almost upright position Aspiration hearing speech teeth , and . In how many surgeries is cleft palate repaired? Why is final repair of the palate delayed until 4 to 5 years? How are cleft lip and cleft palate primarily treated? Is the infant restrained BEFORE repair? Should children with cleft palate BEFORE surgery be allowed to cry? To breast-feed? AFTER repair of cleft lip is infant allowed to cry? To breast feed? Two surgeries one at 12 to 18 months the last at 4 to 5 years Earlier surgery would interfere with tooth development. Surgical repair No, just AFTER repair Yes, they can cry; may breast feed with simple cleft lip however palate interferes with feeding No, the infant should be held to PREVENT CRYING; the infant is not allowed to breast-feed because sucking is not good after lip repair. After clep lip repair, what device will the baby wear? What is the purpose of a Logan Bow? With what device will the infant be restrained? How do you care for an infant with a Logan Bow? Can cleft lip /palate babies sleep on their backs? What position is contraindicated after cleft lip repair? What will be used to feed the infant after cleft lip repair? What must the mother do after feeding the baby who has had cleft lip/palate repair? A Logan bow To prevent stress on the suture line Elbow restraints Remove the gauze before feeding and cleanse after feeding with peroxide and saline. Yes NEVER lie on their abdomen A dropper/syringe with rubber tip to discourage sucking Rinse the infant's/child's mouth with water What is a colostomy? A surgically created opening of the colon out onto the abdomen wall. Name the 3 most common reasons for a colostomy. What is meant by the term "temporary colostomy"? What is meant by the term "double barrel" colostomy? Colostomies performed for cancer tend to be (temporary/permanent). Colostomies performed for a gunshot are usually (temporary/permanent) In a double-barrel colostomy, from which stoma (barrel) will the stool come out? A fresh new stoma is , Cancer Diverticulitis Ulcerative Colitis A colostomy that is not intended to be permanent-- the bowel will be reconnected at a later date and the client will defecate normally A procedure where the colon is cut and both ends are brought out onto the abdomen. Permanent Temporary Proximal Red, large, noisy and . When a client voices embarrassment over the noises that their colostomy makes on the first post-op day, what would you say? The noise will go away in a few days to a week. What behavior on the part of the client is the BEST indicator that they have accepted their stoma? By what day post-op should the client begin to take care of their own stoma? The MORE colon is removed the more the stool. What technique is used to remove feces and flatus from the bowel through a colostomy? How many times per day will the client irrigate his colostomy? Which solution is used to irrigate a colostomy? How warm should the irrigation solution be? In what position should the client be when they irrigate their colostomy? When they do their own stoma care By the 3rd to 4th day, they should be looking at it and asking questions by day 2. Liquid Colostomy irrigation Once Tap water Warmer than body temperature, ie, 99- 100F Sitting Illeostomy liquid stool odor mild stool very damaging to the skin continuous drainage high risk for fluid/electrolyte imbalances incontinent never irrigate Transverse Colostomy soft stool typical stool odor stool damages the skin empties several times per day may or may not be at risk for fluid/electrolytes imbalances may irrigate Descending Colostomy formed stool typical stool odor stool doesn't irrigate unless diarrhea predictable 2 to 3 times per day emptying lowest risk for fluid/electrolyte imbalances continent do irrigate CHF can be right-sided, left sided or both-sided. (T/F) True- left sided usually comes FIRST What does right sided CHF mean? What does left sided CHF mean? CHF can result from MI. (T/F) When cardiac output fails, name three ways the heart will try to compensate. What is meant by "cardiac decompensation"? Name the three groups of drugs used to treat CHF? What is the activity order for clients with CHF? What special item do clients with CHF have to wear to decrease venous stasis in the legs? How often should anti- embolism hose (TED) be removed? When during the day should TED hose be applied? Is it okay to use powder with TED hose? Should you massage the calves of the client with CHF? Before you give digitalis, what action must you take? If the adult client's apical pulse is below 60, what should you do? Right ventricle has decompensated Dependent Edema (legs and sacrum) Jugular venous distention Abdominal distention Hepatomegaly Splenomegaly Anorexia and nausea Weight gain Nocturnal diuresis Swelling of the fingers and hands Increased BP Left ventricle has decompensated True Ventricle hypertrophy Dilate and heart rate will increase It means that the compensatory mechanisms - hypertrophy, dilation, tachycardia are not working and the heart has failed. Diuretics Vasodilators Digitalis Bed Rest TED hose Daily Before the client gets out of bed Yes Never Measure the apical pulse Do not give digitalis For a child don't give for a pulse under 70 For an infant don't give for a pulse under 90 What daily measurement best indicates the amount of fluid the client is retaining? Should clients with CHF have a Foley catheter? What complication is common in CHF? When the client is taking diuretics, what mineral is the CHF client most likely to lose? You should tell the client with CHF to immediately report to his/her doctor if he/she gains pounds in one Daily weight Yes, on diuretics and fluid balance is important Pulmonary edema Potassium--K+ Three week. Name the four most common toxic effects of digitalis. Should hearing aids be removed before going for surgery? Hearing aids are more useful in sensory or conductive hearing loss? Some women experience discomfort when wearing contact lenses during pregnancy or menstrual periods. (T/F) Should a client sleep with the hearing aide in place? What the two most common causes of whistling and squealing of a hearing aid? What solution should be used to clean a hearing aid? What solution is best to use if you intend to remove a client's contact lenses? Hearing aids make sounds more distinct and clear. (T/F) Anorexia N&V-- very common Yellow vision Arrythmia Yes, but just before surgery Conductive True No, a client should not sleep with a hearing aide in place. Loose earmold Low battery Soap and water Sterile saline False, they only amplify--make it louder, they do not clarify Can you use alcohol on the earmold of a hearing aid? The connecting tube of a hearing aid can be cleansed No, it dries and cracks it A pipe cleaner with . What is the most common complication of malpositioned lenses in the comatose or confused patient? Corneal ulceration 1 kg 1000 cc 1 inch 2.5 cm 1 ml 1 cc 1 tsp 4 to 5 cc 1 g 1000 mg 1 L 1000 cc 1 oz 30 cc 1 kg 2.2 lbs 1 tbs 15 cc 1 tbs 3 tsp 1 gm 15 gr 1 gr 60 mg Cushings syndrome is secretion of Oversecretion; glucocorticoids, mineralocorticoids, androgenic hormones; , the and by . adrenal gland In Cushings the blood sugar is (increased/decreased). In Cushings the sodium level is (increased/decreased) In Cushings syndrome, the client develops face. In Cushings syndrome, the trunk is and the extremities are . What is seen on the abdomen of the patient with Cushings? Men with Cushings develop _. Increased Increased Moon Obese, thin Striae--purple horizontal lines Gynecomastia What is gynecomastia? Female-type breasts Women with Cushings develop? Hirsutism Amenorrhea What is hirsuitism? Hair where you don't want it The Cushings syndrome patient will have a on their Buffalo hump upper back. The patient with Cushings Syndrome will have (increased/decreased) blood pressure. The Cushings syndrome patient will have natremia, kalemia and glycemia. Cushings clients will have (increased/decreased) resistance to infection. Chronic therapy imitates Cushings. Cushings Man aka Cush Man Increased, remember retaining water and sodium Hyper; hypo; hyper Decreased Steroid moon face with infection buffalo hump on back big trunk thin extremities loses potassium keeps glucose and salt has striations on abdomen and breasts Is CF hereditary? Yes What glands are affected in CF? What is the appearance of the stool in a client with CF? remember the 4 Fs What are the top 2 nursing diagnoses for a client with CF? What is the classic test for CF? In which two systems/organs are the most problems in CF? How does the client evaluate the activity of their pancreas? Exocrine glands Fat Frothy Foul-smelling Floating Steatorrhea Decreased airway clearance Alteration in nutrition or absorption Iontophoresis - sweat test Lungs Pancreas Observe stools for steatorrhea What is the typical diet for CF client? The major problem in CF is . The most common intervention for the CF client with a diagnosis of decreased airway clearance is High calorie High protein Modified fat Increased viscosity of the secretions of exocrine glands lead to obstruction. Postural drainage . What vitamins need to be replaced in CF? What do CF clients need to do (ingest) in hot weather? The child with the diagnosis of CF probably had a history of at Fat soluble in water soluble form -- A,D,E,K Take NaCl tablets Meconium ileus-- bowel obstruction due to the thickness of the stool. birth. Why is the child with CF receiving pancreas/viokase/pancr eatin? When should the child with CF take his pancreatin/viokase/panc reas? They are enzymes which aid absorption of nutrients. With meals, so it is in the gut while the food is present, the whole purpose is to increase absorption of ingested food. Define Cystoscopy? Direct visualization of the urethra and bladder through a cystoscope. What would you do if the client had any one of the following after cystoscopy: bladder spasm, burning, frequency? What would you do if the client's urine was pink- tinged after cystoscopy? Is the client NPO before cystoscopy? Are enemas required before cystoscopy? Should you encourage fluids after cystoscopy? Is a signed informed consent required for cystoscopy? Record it but no need to call the MD Record it in the notes, no need to call the MD. No, not unless a child with a general anesthetic-- in fact with adults you should encourage fluids. No, but may be ordered. yes Yes What vital sign changes are most ominous after cystoscopy? Is the client sedated for a cystoscopy? What drugs are most commonly given before cystoscopy? Increasing dietary fiber lowers the risk of of the A fall in the blood pressure and increase in the pulse-- increasing hemorrhage It is done under LOCAL anesthesia. General anesthesia may be used for a child. Valium or demerol Cancer, colon . Foods lose some or all of their fiber when they Processed, cooked, peeled, refined are . , or . Whole grains and grain products are (high/low) in fiber. Fruits are (high/low) in fiber. Veggies are (high/low) in fiber. Milk and milk products are (high/low) in fiber. Meats are (high/low) in fiber. Nuts, seeds, and legumes are (high/low) in fiber. Which has highest fiber? Grains, fruits, veggies, nuts. When a person increases fiber in the diet they should do High High High Low Low Low Grains, especially bran Slowly so . Side effects of a high fiber diet Gas (flatus), minerals include malabsorption of . Of milled bread, and Whole grain enriched bread, fortified bread and whole grain bread; which is highest in fiber? What structures in the brain are most affected in Parkinson's? Basal ganglia The neurotransmitter imbalance that causes Parkinson's is a Decrease, dopamine activity in . What drugs can cause a Parkinson-like syndrome? What is the classic motor manifestation of Parkinson's? What type of rigidity is typical of Parkinson's? Parkinson's patients move fast or slow? What type of gait is seen in Parkinson's? Patient's with Parkinson's have speech. Patients with Parkinson's tend to have constipation or diarrhea? Name four drugs used to treat Parkinson's. In what type of chair should Parkinson's patients sit? What time of day can be particularly dangerous for the Parkinson's patient? When a patient is taking Levodopa he should have assistance getting out of bed because... What vitamin should patients on Levodopa avoid? Levodopa should be given with or without food? What might Levodopa do to patients urine? The tremors of Parkinson's will get better or worse when they purposefully move or perform a task? The client on a PCA pump is less likely to have post-operative complications than the client without a PCA pump. (T/F) Haldol, major tranquilizers -- drugs that end in -azine Pill-rolling and tremors Cogwheel Slow Shuffling slow gait Monotone Constipation Levodopa, Sinement, Symmetrol, Cogentin, Artane, Parlodel Firm, hard-backed Mealtime, due to choking Of orthostatic hypotension B6 pyridoxine With Make it very dark Better, they tremor more when not performing an action True, because the comfortable patient moves around more and is less likely to get thrombophlebitis, pulmonary embolus, fatigue, ileus and pneumonia Clients with COPD are not good candidates for PCA pumps. (T/F) Name the three most common uses of PCA techniques. PCA pumps allow a more constant level of serum drug than conventional analgesia. (T/F) A major disadvantage of PCA pump is that the client can take too much medication. (T/F) Clients on PCA pumps use more medication than those receiving IM injections. (T/F) A disadvantage of PCA pumps is that the client does not ambulate as early due to the machine. (T/F) When discontinuing a PCA infusion it is acceptable to discard the drug cartridge. (T/F) Comfort range or relative humidity is... Which patients should be forbidden to smoke? Smoke alone? When applying restraints remember to... List ways to ensure privacy... Plastic pillow cases are . (disadvantages) When using restraints with clients who object, don't forget about True, due to the effects of narcotics on central respiratory control Post-operative pain, cancer pain, sickle- cell crisis pain True False, it is not possible for the client to overdose due to the lock-out feature False, they use less False, PCA clients ambulate earlier and they pull their machine with them. False, the whole cartridge system must be returned to the pharmacy due to federal narcotic control laws. 30-60% Those with oxygen in the room, confused, sleepy, drugged clients Avoid bruising skin, cutting off circulation, accidental entangling Use drapes and screens during care in semi-private rooms Hot and slippery False imprisonment - . Individuals who are ill more are sensitive to noise than individuals who are well. When you are not at the bedside the bed should always be... Can nurses be held liable for an accident resulting from a client not being told how to use the call light? In the lowest position yes Dangers associated with drafts are... The first thing a nurse should do when a client objects to side rails is... The comfort range of temperature is... Is having the client verbally identify himself considered adequate safety? Bed side rails should be up for the following individuals... The symptoms of sensory overload and sensory deprivation are... If a family member asks to have the side rails down while they are in the room you should... Pillows are sterilized between uses. (T/F) What is the common name for pediculosis? What is the common finding with pediculosis pubis? What common household solution is used to remove nits? What shampoo is used for lice? Where are head lice most commonly found? Circulation of micro-organisms on air currents Explain why they are being used. 68 to 74 degrees No, only identification bands are acceptable. Elderly clients, unconscious, babies, young children, restless, confused Fear, panic, depression, inability to concentrate, restlessness, agitation Remember that you are responsible for the client's safety-- not his family, it might be unwise to permit this False Lice Reddish-brown dust in the underwear Vinegar. Nits are the eggs of lice that adhere to the hair shaft Kwell At the back of the head and behind the ears On what do lice feed? Blood After treatment how long do you have to inspect for lice? What is the most common symptom of lice? What is the most dangerous toxicity of Kwell? What is the typical of the lesions of pemphigus? What is the characteristic lesion of pemphigus? Inspect for 2 weeks to be sure that they are all gone Itching CNS toxicity Foul-smelling, blisters break easily, seen in the elderly, cause unknown Large vesicular bullae What are bullae? Large blisters What chemical is added to the bath water of a client with pemphigus? What precaution must be taken with potassium permanganate? What is the typical skin care of pemphigus? What unusual nursing diagnosis is high priority in pemphigus? What are the top three nursing interventions in pemphigus? What kinds of fluids will clients with pemphigus drink best? What drugs are most commonly used? Should steroids be given with meals? What is the #1 cause of death in pemphigus? Potassium permanganate Be careful that no undissolved crystals touch the client; it will burn the skin Cool wet dressing Alteration in fluid and electrolyte balance Oral care, protection from infection, encouraging high fluid intake Cold fluids Steroids Always Overwhelming infection Pemphigus An acute or chronic disease of adults, characterized by occurence of successive crops of bullae that appear suddenly or apparently normal skin and disappear, leaving pigmented spots. It may be attended by itching and burning and constitutional disturbance. The disease if untreated is usually fatal. A characteristic finding is a positive Nikolsky sign: When pressure is applied tangential to the surface of affected skin, the outer layer of epidermis will detach from the lower layer. (Probably autoimmune) Peritoneal Dialysis (PD) The removal of wastes, electrolytes and fluids from the body using peritoneum as dialysis membrane When PD is being used the client must be on heparin. (T/F) How long does one episode/course of PD last? With PD there is a high/low risk of peritonitis? When fluid accumulates in the abdomen during PD what problem does the client experience first? False, you do not need to be heparinized for peritoneal, but you do need to be heparinized for hemodialysis Could be 10 hours High Dyspnea - SOB or difficulty breathing, due to the inability of the diaphragm to descend What nutrient is lost in highest amounts during PD? Can a client who had recent bowel surgery get PD? Should a client who is having breathing problems receive PD? What body surface must be punctured to administer PD? The solution introduced into the peritoneum during PD is called... Before allowing the dialysate to flow into the peritoneal cavity it must Protein No No The abdomen Dialysate Warmed, body be to temperature. Before PD it is important the client be... What force is used to introduce the dialysate into the peritoneum? How fast does the dialysate usually flow into the peritoneum? How long is the dialysate allowed to remain in the peritoneum before it is drained out? How long does it usually take for the dialysate to drain out of the peritoneum? If the dialysate does not drain out well, you would first... What color is the dialysate when it comes out? Should you raise the HOB to increase drainage of the dialysate? How often do you measure vital signs during PD? Can a client on PD: Sit in a chair? Eat? Urinate? Defacate? Weighed, to assess water loss or gain Gravity only, no pumps In 10 minutes 15-30 minutes 10 minutes: (10 minutes flow in, 30 minutes in abdominal cavity, 10 minutes flow out = total of 50 minutes) Have them turn side to side Straw-colored - clear Yes Every 15 minutes during the first cycle and every hour thereafter Yes to all If too much fluid is removed during PD, the client will experience... If the client absorbs too much of the dialysate the client will experience... If the client complains of dyspnea during PD you Decreased blood pressure (hypotension) Increased blood pressure (circulatory overload) Slow the flow, elevate HOB would first , then . If the client complains of abdominal pain during PD you would first... Cloudy drainage in the dialysate commonly means... What would you do if you noticed a small amount of blood come out in the first few bottles that were infused? What precautions are important in the care of the client receiving PD? Is I&O important to record during PD? How high should the dialysate bag be when its infused? What factor do clients with pernicious anemia lack? What vitamin is not absorbed in a patient with pernicious anemia? What is another name for Vitamin B-12? Why isn't Vitamin B-12 absorbed in pernicious anemia? What happens when patients with pernicious anemia don't absorb Vitamin B-12? What other disease can be confused with pernicious anemia? What are some classic and unique signs of pernicious anemia? Encourage them to move about Peritonitis (Not good, call MD) Nothing, this is normal: the blood is due to the initial puncture of the abdomen Safety, because they get dizzy. Yes Shoulder height Intrinsic factor. It has no other name. Vitamin B-12 Extrinsic factor Because these patients lack intrinsic factor Their RBC's do not mature and they become seriously anemic. Angina pectoris Beefy red tongue Numbness and tingling of the hands Sores in the mouth Chest pain What is the medical treatment for pernicious anemia? How long must the client receive this medical treatment? Can we cure pernicious anemia? What unique urine test is done to diagnose pernicious anemia? Is it okay to give B12 orally to a client with pernicious anemia? What neurologic test do they do for this anemia? What is conservation? In what stage does it develop? What is the age range of formal operation thinking? What is the sensori- motor stage of intellectual development? What is the age range of concrete operational thinking? What is the age range of pre-operational thinking? Hint: Think of PRE- schoolers. What is the classic pattern in formal operational thinking? What is egocentricity? In what stage is it found? In Placenta Previa the placenta is implanted than it should be and lays over the IM injections of Vitamin B-12 For the rest of life No, just treat the symptoms. The Schilling test No, it will never be absorbed due to a lack of intrinsic factor The Romberg test (a test for balance), in normal people this test is negative, in the client with pernicious anemia this test becomes positive When the child realized that number, weight, volume remain the same even when outward appearances change; Concrete Operational 12-15 It is the intellectual stage of children from birth to 2 years 7-11 3-6 Abstract reasoning The child views everything from his frame of reference, common in pre-operational thinking Lower, cervical os . What is the classic symptom of Placenta Previa? In whom is Placenta Previa most likely to occur? Primigravida's or multigravida's? Painless 3rd trimester bleeding (hint: Painless Placenta Previa) Multigravidas What is meant when the physician/nurse use the terms total (complete) or partial (incomplete) in reference to placenta previa? What are the 3 complications of placenta previa? What is the best and safest way to confirm placenta previa? Should a woman with placenta previa be hospitalized? If a surgeon delays doing a C-section for Placenta Previa it is due to: (reason for delay). As soon as Placenta Previa is diagnosed, most pregnancies will be terminated via C-section if the fetus is mature. (T/F) If a woman is admitted with active bleeding with Placenta Previa you should monitor fetal heart tones . It is not necessary to use electronic fetal monitoring when there is active bleeding in Placenta Previa. (T/F) Will a woman with active bleeding in Placenta Previa be given any systemic pain relief during labor? If you were told to start the IV on the woman admitted for Placenta Previa, what gauge needle would you use? Pneumonia is an Total or complete: placenta covers whole cervical opening Partial or incomplete: placenta covers only part of the cervical opening Shock Maternal death Fetal death Ultrasound Yes, always if bleeding Immaturity of the fetus (they will want the child to mature) True Continuously via fetal monitor False, infant must always be monitored No, they don't want to depress the fetus 18 gauge, or any other large enough to administer blood Infection, alveoli, lungs the in the of . Pneumonia is only caused by bacteria. (T/F) False, it can be caused by viruses and aspiration. Which blood gas disorder is most common in pneumonia? What is polycythemia vera? What is the typical complexion of a client with polycythemia vera? What procedure is done to relieve symptoms in polycythemia vera? Respiratory alkalosis, because the hyperventilation blows off more CO2, than the consolidation traps in the blood A blood disease in which there is an increase in erythrocytes, leukocytes and platelets Ruddy red, almost purple Phlebotomy What is phlebotomy? Drain off 200-500 cc of blood from body (opposite of transfusion). What type of diet will people with polycythemia vera be on? What are three signs of polycythemia vera? Is hemoglobin increased or decreased in this disease? What oral problem will people with polycythemia vera have? What organ will be enlarged in polycythemia vera? Due to increased destruction of RBC's seen in polycythemia vera what blood level will be increased? What drug is most commonly used in polycythemia vera? How often should the client cough and deep breath post-operatively? How often should the post-operative patient turn? How often should the patient use the incentive spirometer? How often should the nurse auscultate the lung sounds post- operatively? Low iron Headache Weakness Itching Increased Bleeding mucous membranes The spleen, because it is destroying the excessive RBC's. Uric acid levels will be high (remember - uric acid levels are always high when cells are being destroyed as in hemolysis, chemotherapy or radiation therapy) Myleran -- (this is usually used for bone marrow cancer) Every 2 hours Every 2 hours Every 1-2 hours Every 4 hours How often should the bedridden post- operative patient do leg exercises? The post-operative patient should void by hours post- operatively or you must call the MD. Will the typical post- operative client have lung sounds? Bowel sounds? Increased temperature? Unless contraindicated the patient should be out of bed no later than hours post- operatively. Deep vein thrombosis is most common in what type of surgery? The most common complication of deep vein thrombosis Every 2 hours 6 to 8 Lung - yes; bowel sounds - no; Low grade temperature - yes 24 Low abdominal or pelvic Pulmonary embolism . The best way to prevent thrombophlebitis is TED hose. (T/F) False, ambulation/exercise are the best ways. What is paralytic ileus? Paralysis of the bowel due to surgery (common --especially in abdominal surgery) If a post-operative patient complains of gas and cramping you should first Assess then ambulate then . The typical post- operative inflammatory temperature elevation is in the range of . The onset of post operative infection is on the or 99.8 to 101 degrees 2nd or 3rd, never before that (remember elevated temperatures earlier than the 2nd post-operative day is NOT infection) day post-operative day. Define dehiscense Separation of the incisional edges Define evisceration Protrusion of abdominal contents through a dehiscence. What do you do for dehiscence? Decrease HOB (but not flat); cover with sterile gauze moistened with sterile saline, call MD What do you do, in order, for evisceration? Decrease HOB (but not flat); cover with sterile gauze moistened with sterile saline, call MD ante- Before in time or place (ie. "antepartal - before giving birth) Im-; in- "Not" or "into" intra- Occurring within inter- Between per- Throughout, completely, a large amount ec- Out of e-; ex- Out from, away from, outside iso- A combining form meaning 'equal' para- Similar, beside Pregnancy (decreases/increases) the body's insulin requirements. Can pregnancy convert a non-diabetic woman into a diabetic? What name is is given to diabetes that is brought on by pregnancy? Diabetes with pregnancy is (more/less) common as the woman ages. What is the #1 cause of infant illness when the mother has diabetes? When is infant hypoglycemia most likely to occur during labor and delivery? Hormones of pregnancy work against insulin. (T/F) A sign of gestational diabetes is excessive (weight gain/weight loss) (Obese/very thin) women are most likely to become diabetic during pregnancy. In gestational diabetes the client experiences a (decrease/increase) in thirst In gestational diabetes the client experiences a (decrease/increase) in urine output. Increases Yes Gestational diabetes More Hypoglycemia In the hours immediately following delivery True Weight gain Obese Increase (polydipsia) Increase (polyuria) Gestational diabetes is associated with what OB history? Women who have gestational diabetes tend to deliver infants who are (small/large). Gestational diabetics tend to get infections. What test confirms the diagnoses of gestational diabetes? What are the two main treatment methods in gestational diabetes? How often should a woman visit the doctor prenatally if diabetes is present? How many pounds per week is the diabetic allowed to gain the 2nd and 3rd trimesters? Is severe carbohydrate restriction required in gestational diabetics? Of protein, fat, and carbohydrates, which ones (percent-wise) increase in the diet of gestational diabetics? When is insulin used in the treatment of gestatinal diabetes? If insulin is used, the dose is the same in all 3 trimesters. (T/F) Oral hypoglycemics should never be used during pregnancy. (T/F) When should a diabetic be delivered? What IV solution is used during labor for the diabetic? The mother's insulin requirements will (fall/rise) markedly after delivery. During pregnancy what complications is most dangerous for the fetus of a diabetic? Previous large baby (over 9 lbs), unexplained stillbirth, miscarriage, congenital anomalies Large for gestational age Monilial (yeast) 3 hour glucose tolerance test Diet, insulin Twice a month, then once per week in the 3rd trimester 1 pound a week No, it could lead to ketosis Protein, fat When dietary control does not keep the blood sugar within normal limits False, it varies True, they cause birth defects (teratogenic) Between 37 and 39 weeks D5W Fall ketosis If ketosis is a big problem for the baby during pregnancy what the big problem after delivery? Why is hypoglycemia such a dangerous problem? (Multi/prima) gravida clients are most likely to get PIH. Which age group(s) are most likely to experience PIH? When does pre- eclampsia usually begin in pregnancy (week)? Name the three symptoms of PIH. If pre-eclampsia is mild will the woman be hospitalized? What type of diet is indicated for a woman with pre-eclampsia? What measurement must the woman with pre-eclampsia make every day? What is the activity order for a woman with severe pre-eclampsia? What is the dietary order for the woman with severe pre-eclampsia? Are diuretics used for women with pre- eclampsia? When a woman is hospitalized for severe pre-eclampsia the nurse should test... When pre-eclampsia gets worse the deep tendon reflexes will be (hyper/hypo) reflexia. Pre-eclampsia makes the neuromuscular system more or less irritable? What vision problem do women with pre- eclampsia have? Hypoglycemia Brain cells die without glucose, brain damage Primagravida Patients under 18 and over 35 After 20 weeks Hypertension, weight gain (edema), proteinuria No, just rest at home Increased protein/normal salt intake (no restriction typically) She must weigh herself Left side lying Low salt, high protein Yes #1 reflexes, the urine for protein Hyper-reflexia More Blurred vision What types of precautions will be in effect for a woman with severe pre-eclampsia? Name 5 things included in seizure precations. When is pre-eclampsia called eclampsia? In eclamptic client what ominous sign almost always precedes a seizure? What are the three major treatment objectives in eclampsia? The urine output of the eclamptic client will (decrease/increase). How would you palpate the uterus to see if the eclamptic woman was having contractions? Premature rupture of membranes (PROM) is Seizure precautions Suction machine in room O2 in room Padded rails up X 4 Must stay on unit Ambulation with supervision only No More than 1 pillow Once convulsions have occured Severe epigastric pain Decrease blood pressure Control convulsions Diuresis Decrease Place the hand flat on the abdomen over the fundus with fingers apart and press lightly Spontaneous, before, onset a amniotic sac break in the the of contractions. Usually labor starts 24 within hours of rupture membranes. What is the danger with PROM? How would you tell if the woman with PROM had an infection? To test amniotic fluid the nurse should check the of the fluid. Amniotic fluid is (acidic/alkaline) Being alkaline means have a (high/low) pH Amniotic fluid turns nitrazine paper deep (color). When PROM occurs, the age of the fetus must be determined. The best way to assess lung maturity is to check the ratio. Infection Maternal fever Fetal tachycardia Foul smelling vaginal discharge pH Alkaline High Blue L/S (lecithin/sphingomyelin) An L/S ratio greater than indicates lung 2.0 maturity. If labor does not begin 24 within hours after PROM, labor will likely be induced. If PROM occurs before viability, what is the typical management? If PROM occurs after viability but before 36 weeks, what is the typical management? If there are any signs of infection after PROM, what must occur immediately? PROM always occurs in a gush of fluid. (T/F) The woman must avoid sexual intercourse if PROM has occurred. (T/F) What does self- disclosure mean? Is it always bad for the nurse to self-disclose? If the nurse uses self- disclosure it should be and the conversation should be... Insight means the ability of the patient to his problem. During what phase should the nurse examine his/her own feelings? Flight of ideas is when the patient changes topics of conversation . The basis for a Termination of pregnancy Hospitalize, watch for infection, try to gain time for the infant to mature Delivery of fetus False True When the nurse tells the patient personal information about self. No, you can self-disclose as long as you do it cautiously and you are 100% sure it is therapeutic. Short, quickly refocused back on the patient Understand Pre-interaction phase Rapidly Nurse's, awareness, self understanding therapeutic nurse/patient relationship begins with the and , self . What are the steps of the nurse/patient therapeutic relationship? Pre-interaction phase Orientation phase Working phase Termination phase Should the nurse self- disclose if the patient asks the nurse to? The nurse should introduce information about the end of the nurse/patient relationship during the phase. Termination phase begins in the phase. Pulmonary edema is accumulation of in the lung. Pulmonary edema is a common complication of disorders. Pulmonary edema usually results from failure. What force causes the pulmonary edema in left ventricular failure? Can letting IVs run too fast cause pulmonary edema? What are the four classic signs of pulmonary edema? What is meant by dyspnea on exertion? What is meant by paroxysmal nocturnal dyspnea? What is meant by orthopnea? Is heart rate fast or slow in pulmonary edema? What will the nurse auscultate over the lungs when pulmonary edema occurs? When pulmonary edema is severe what does the sputum look like? What drug is used in pulmonary edema to reduce fluid in the lungs? What drug is used to increase ventilation in clients with pulmonary edema? No, not unless it is specifically therapeutic. Orientation Orientation Fluid Cardiovascular Left ventricular Increased hydrostatic pressure in the pulmonary capillaries Yes in the client with poor cardiovascular function Dyspnea on exertion, paroxysmal nocturnal dyspnea, orthopnea, coughing Shortness of breath when active. Sudden episodes of difficulty breathing Shortness of breath when lying flat Fast, tachycardia Crackles (rales) Bloody and frothy A diuretic (Lasix) Aminophylline (bronchodilator) Is O2 given in pulmonary edema? Since pulmonary edema is caused by left ventricular failure what drug is given? Why is morphine given to clients with pulmonary edema? If your client suddenly goes into pulmonary edema what would you do first? Pulmonary embolus is an obstruction of the Yes Digitalis To decrease apprehension and decrease preload, this rests the heart Elevate the HOB, then increase O2, then call the MD Capillary, thrombus pulmonary by a dislodged bed or foreign substance. Where do the emboli that cause pulmonary embolus usually come from? Besides a thrombus what else can cause an embolus in the lung? What treatment modality can lead to pulmonary embolus? What class of drugs can lead to pulmonary embolus? What heart problem can lead to pulmonary embolus? What genetic disorder can lead to pulmonary embolus? What is the first sign of pulmonary embolus? The dyspnea of pulmonary embolus is accompanied by . Does the heart rate increase or decrease in pulmonary embolus? With severe pulmonary embolus the client will look as though they are . What are the two major treatments of pulmonary embolus? The legs Air, fat, tumor cells Bed rest Oral contraceptives Atrial fibrillation (RIGHT atrial fibrillation casues pulmonary embolus; LEFT atrial fibrillation causes cerebral embolus) Sickle cell anemia Dyspnea Pleuritic pain Increase In Shock O2, anticoagulants Name the anitcoagulant given for immediate anticoagulation by IV or SQ route. A drug for long term anticoagulation in any disorder would be? What two lab tests monitor coumadin therapy? When coumadin is therapeutic, the INR should be between Heparin Coumadin Prothrombin time (PT) and the INR 2.0 and 3.0 and . What is lovenox? It is a low-dose Heparin used for anticoagulation in POST-OP THROMBOPHLEBITIS PREVENTION NOT USED FOR PULMONARY EMBOLUS Heparin therapy is monitored by daily measurement of the . Effective heparin therapy rises the PTT to approximately times normal. Clients on heparin should use an electric razor or safety razor? What is the best way to prevent pulmonary embolus in post- operative patients? Is it appropriate to massage the legs of the client to preven pulmonary embolus? Heparin is used in the acute phase of pulmonary embolus. What drug is used for 6 months after pulmonary embolus? Coumadin therapy is monitored by what daily test? PTT (partial thromboplastin time) 2.5 Electric razor Early ambulation No, never Coumadin PT (prothrombin time) What is pyelonephritis? A bacterial infection of the kidneys Which organism causes pyelonephritis? E. Coli Name the symptoms that pyelonephritis and cystitis have in common? What medical intervention is necessary in pyelonephritis? How does pyelonephritis differ from cystitis in meaning? What causes or precedes pyelonephritis? Will the client with pyelonephritis have daily weights? Name the five signs/symptoms that pyelonephritis has that cystitis does not have? What is the BIG danger with pyelonephritis? How is pyelonephritis prevented? Will the client with pyelonephritis have hematuria? The patient with pyelonephritis will have (hypertension/hypotentio n)? Where is the pyloric sphincter? What does stenosis mean? What is done to correct pyloric stenosis? In what position should the child with Pyloric Stenosis be during feeding? The feedings for an infant with pyloric stenosis should be thick or thin? What test is done to confirm a diagnosis of pyloric stenosis? These infants are prone Frequency, urgency, burning, cloudy, foul smelling urine IV antibiotics for one to two weeks, must get urine culture 2 weeks after antibiotic therapy is over Cystitis means bladder infection; pyelonephritis means an infection of kidney pelvis Cystitis always does Yes, as would any client with kidney problem Fever, flank pain, chills, increased WBC, malaise Permanent scarring and kidney damage By preventing or treating all cystitis (UTI's) It is common but not always present Hypertension At the distal (duodenal) end of the stomach Narrowed Surgery (pyloromyotomy) High fowlers Thickened Upper GI series (barium swallow) Dehydration, thrive to develop failure to and . Why does the pyloric valve become stenosed in pyloric stenosis? In what position should a child with pyloric stenosis be after a feeding? The infant with pyloric stenosis appears even after vomiting. What do you see during and after feeding? Is vomiting projectile or non-projectile in patients with pyloric stenosis? Is the vomiting bile-stained or not bile-stained? What assessment finding is found under the right rib cage? The symptoms of pyloric stenosis mostly commonly appear at age It hypertrophies Right side with HOB up Hungry Peristaltic waves from left to right Projectile, not bile-stained An olive sized bulge (the hypertrophied pylorus) 4 to 6 weeks to . Describe the typical child with pyloric stenosis. For what reason are Montgomery straps used? Sutures in general are Firstborn, full term, white, boys Permit you to remove & replace dressings without using tape (protects the skin) 7th removed by the day. Leaving a would open to air decease infection by eliminating what 3 environmental conditions? To remove tape always pull (toward/away) from the wound. Dark, warm, moist Toward (this way you don't put pressure/pull on the suture line.) Define contusion. Bruise (internal) Define debridement. Removal of necrotic tissue from a wound. What is the purpose of a wound drain? To prevent germs from getting into or out of a wound you should use what type of dressing? What solution is put onto the skin to protect it from the irritating effects of the tape? Remove secretions from the area so healing occurs. An occlusive dressing Tincture of benzoin With what is a round closed in first intention? What is another name of second intention? When swabbing an incision you would start at the incision or 1 Inch away from the incision? After you remove soiled dressings and before you put on the sterile dressing you must.... What is meant be the phrase "advance the drain 1 inch"? After advancing a Penrose drain you (should/should not) cut off the excess drain? When a dressing saturated, germs can enter the wound from the outside. (T/F) When is a bad time to change dressings? Sutures or steri-strips, staples Granulation Start at the incision and move outward. Wash your hands and put on sterile gloves You pull the drain out 1 inch. Should True, by a process called capillary action Mealtime Define laceration. Cut Scoliosis is a curvature of the . Scoliosis is MOST common in the and Lateral, spine Thoracic and lumbar sections of the spinal column. Scoliosis in the thoracic spine is usually convex to the (left/right). Scoliosis in the lumbar spine is usually convex to the (left/right). With which other two spine deformities is scoliosis associated? Right Left (*Hint: curve Left in Lumbar) Kyphosis (humpback), Lordosis (swayback) What is Kyphosis? Humpback in the thoracic area What is Lordosis? Swayback in the lumbar region (Lumbar, Lordosis) What is the difference between structural and functional scoliosis? What age group should be routinely screened for scoliosis? Structural-you are born with; Functional- you get from bad posture Young teens What are the 3 subjective complaints of clients with scoliosis? What test/exam CONFIRMS the diagnosis of scoliosis? What type of brace is most commonly used for scoliosis? Name 4 exercises used to treat mild scoliosis. What kind of treatment is done for severe scoliosis? What type of cast is used post-operatively? What kind of rod is used to "fix" curvature? Scoliosis MOST commonly affects Back pain, dyspnea, fatigue X-rays of the spine Milwaukee Heel lifts; sit-ups; hyperextension of the spine; breathing exercises Surgical fusion with rod insertion Risser cast Harrington Rod Teenage females (type of clients). How many hours a day should the client wear a Milkwaukee brace? What solution should be used on the skin where the brace rubs? Clients with a Milwaukee brace should avoid vigorous exercise. (T/F) After corrective SURGERY how is the client turned? How often should the neurovascular status of the extremities of a client in a Risser cast be measured? Fresh post- operatively? What is a common complication of a client in a body cast (like a Risser cast)? 23 Tincture of benzoin or alcohol,no lotions of ointments-you want to toughen the skin not soften it True Log rolled (in a body cast) Every 2 hours Cast syndrome What is cast syndrome? Nausea, vomiting and abdominal distention that can result in intestinal obstruction What group of people get cast syndrome? What is the treatment of for cast syndrome? How would you, the nurse, assess for developing cast syndrome? What causes cast syndrome, specifically in a Risser cast? The inheritance pattern of sickle-cell anemia is ANYONE in a body cast Removal of the cast, NG tube to decompress, NPO Ask the client if they are experiencing any abdominal symptoms-keep track of bowel movements & passing flatus (if not having BMs or passing flatus, cast syndrome is suspected) Hyperextension of the spine by a body cast: the hyperextension interrupts the nerve & blood supply to the gut Autosomal recessive . What does heterozygous mean? People who are (hetero/homo) have sickle cell trait. What does homozygous mean? People who are (hetero/homo)zygous have sickle cell disease. People with sickle cell TRAIT only carry the disease, they DO NOT have symptoms. (T/F) What are the #1 and #2 causes of sickle cell crisis? The most common type of crisis that occurs is a It means you only have 1 defective gene from 1 parent. Heterozygous It means you have the defective gene from both parents. Homozygous True-usually it has occurred that in times of SEVERE stress, the TRAIT does cause some symptoms but not usually. Hypoxia, dehydration Vaso-occlusive - crisis. In vaso-occlusive crisis the vessels become occluded with . The abnormal hemoglobin produced by people with sickle cell anemia is Abnormal RBC's Hgb S-it "sickles" called Hgb . What shape does Hgb S make the RBC's? Crescent-shaped Why do the crescent- shaped RBCs cause occlusion of the vessels? What are the top 3 priorities in care of the client with sickle-cell crisis? What activity order will the client with sickle cell CRISIS have? Or Tylenol, Morphine, Demoral, Aspirin which is NEVER given to a sickle-cell patient? At what age is death most likely in sickle cell anemia? Sickle-cell anemia symptoms do not appear before They clump together and create a sludge. Oxygenation, hydration, and PAIN control Bed rest Aspirin-it can cause acidosis which makes the crisis and sickling worse Young adulthood 6; fetal hemoglobin the age of months due to the presence of . Sickle cell anemia is most commonly seen in (blacks/whites). Should a child in sickle- cell crisis wear tight clothes? Spinal cord injuries are more common in males. (T/F) In what age range is spinal cord injury most common? The #1 goal in emergency treatment of spinal cord injury is... When halo traction is being used to immobilize the spinal cord the client is Blacks No, it can occlude vessels even more. True 15 to 25 Immobilization of the spine Ambulate allowed to . When the patient with spinal cord injury is in tongs or on a stryker frame or on a circoelectric bed they are on...... The 2 most common surgeries used to treat spinal Absolute bed rest Laminectomy and spinal fusion cord injury are . and What is spinal shock? It is a common occurrence in spinal cord injury in which the spinal cord swells above and below the level in injury When does spinal shock occur? How long does spinal shock last? When the spinal cord injury is at level of to Immediately or within 2 hours of injury 5 days to 3 months C1 to C8 the patient will be a quadriplegic. When the spinal cord injury is between and C1 and C4 , there is permanent respiratory paralysis. Can the patient with spinal cord injury at C7 level have respiratory arrest? Spinal cord injury in the thoracic/lumbar regions result Yes, because even thought his injury was below C4, spinal shock can lead to loss function above the level, however the will not be permanently ventilator dependent- he will breath on when once spinal shock goes away. Paraplegia in plegia. If airway obstruction occurs at the accident site and you suspect spinal cord injury, what maneuver is used to open the airway? In spinal cord injury Modified jaw thrust Move, hyperextend never the neck. How should you change the position of the spinal cord injury patient after he has an order to be up? Why? For the patient with neurogenic bladder you should straight catheterize Slowly, because of severe orthostatic hypotension (they use a tilt table) Every 6 hours every hours. The patient with spinal cord injury will have (flaccid/spastic) muscles. Spastic Name 3 drugs used to treat spasms. What is automatic dysflexia or hyperreflexia? What are the vital sign changes seen in autonomic dysreflexia? What do you do first for the client experiencing autonomic dysreflexia? What do you do secondfor the client experiencing autonomic dysreflexia? Do you need to call the doctor for autonomic dysreflexia? What is the #1 treatment for autonomic dysreflexia? What is the purpose of restricting activity after spinal tap? Should the client drink after a spinal tap? Do you need an informed consent for a spinal tap? Should CSF contain blood? Does the client have to be NPO before a spinal tap? What is the normal color of cerebrospinal fluid? Into what space is the needle inserted during a spinal tap? Can the client turn side- to-side after a spinal tap? In what position should the client be during a spinal tap? Identify the activity restriction necessary after lumbar puncture? Valium, Baclofen, Dantrium A common complication of quadriplegics in response to a fulle bladder or bowel. Sweating, headache, nausea & vomiting, gooseflesh, and severe HYPERtension Raise HOB Check the bladder, check the bowel No, only call the doctor if draining the bladder & removing impaction does not work Drain the bladder, empty the bowel To prevent headache due to CSF loss Yes, encourage fluids to replace CSF Yes No No Clear, colorless Subarachnoid space Yes Lateral decubitus (on their side) position and knees to chest Lie flat for 6 to 12 hours What are the 2 purposes of a spinal tap? Does the client have to be sedated before a spinal tap? To measure or relieve pressure and obtain a CSF sample No Antibiotic (Define) A drug that destroys or inhibits growth of micro-organisms Asepsis (Define) Absence of organisms causing disease Antiseptic (Define) A substance used to destroy or inhibit the growth of pathogens but not necessarily their spores (in general safe to use on persons) Disinfectant (Define) A substance used to destroy pathogens but not necessarily their spores (in general not intended for use on persons) Bactericide (Define) Substance capable of destroying micro- organisms but not necessarily their spores Bacteriostatic (Define) Substance that prevents or inhibits the growth of micro-organisms Anaerobe (Define) Micro-organisms that do not require free oxygen to live Aerobe (Define) Micro-organisms requiring free oxygen to live Pathogen (Define) Micro-organism that causes disease Clean technique (Define) Practices that help reduce the number & spread of micro-organisms (synonym for medical asepsis) Sterile (Define) An item on which all micro-organism have been destroyed Coagulate (Define) Process that thickens or congeals a substance Host (Define) An animal or a person upon which or in which micro-organisms live Portal of entry (Define) Part of the body where organisms enter Contaminate (Define) To make something unclean or unsterile Surgical asepsis (Define) Practices that render & keep objects & areas free from all micro-organisms (synonym for sterile techniques) Medical asepsis (Define) Practices that help reduce the number & spread of micro-organisms (synonym for clean techniques) Spore (Define) A cell produced by a micro-organism which develops into active micro- organisms under proper conditions. Which hand should hold the suction catheter? Which should hold the connecting tube? The nurse should use (medical/surgical) asepsis during airway suction? The dominant, the non-dominant Surgical asepsis (sterile technique) What kind of lubricant should be used on the suction catheter? Should the suction be continuous or intermittent? For how long should suction be applied during any one entry of the catheter? How often should the nurse clear the tubing during suctioning? Which way would you turn the client hear to suction the right mainstem bronchus? The left mainstem bronchus? The best client position during airway suctioning Sterile water-soluble Intermittent to prevent mucosal damage 10 seconds After each pass/entry/removal To the left, to the right Semi-fowlers is . The suction should be delivered while (inserting/removing) the catheter. What outcomes would indicate that suctioning was effective? How often should the client's airway be suctioned? The unconscious client should assume what position during suctioning? If not contraindicated, what action by the nursing before suctioning would most likely reduce hypoxia during suctioning? What solution should be used to clear the tubing during suctioning? With what size catheter should an adult's airway be suctioned? While removing the catheter Clear even lung sounds, normal vital signs When it needs to be, for example moist lung sounds, tachycardia, restlessness (hypoxia), ineffective cough Side-lying, facing nurse Administer a few breaths at 100% oxygen before beginning Sterile saline 12 to 16 French How much suction should be used for an infant? How much suction should be used for a child? How much suction should be used for an adult? Do you assess for suicide potential whenever a patient makes any statement about wanting to die or kill self? Children are at risk for suicide. Adolescents are (low/high) risk for suicide. Young adults are (low/high) risk for suicide. People between 25 and 50 years are (low/moderate /high) risk for suicide. People over 50 year are (low/high) risk for suicide. The patient who has a definite plan is (low/high) risk for suicide. The use of pills makes the patient (low/moderate/high) risk for suicide. The patient who has NO definite plan is (low/high) risk for suicide. Less than 80 mm Hg 80 to 100 mm Hg 120 to 150 mm Hg Yes, in fact whenever a patient makes a statement about wishing or wanting to die or kill self you must ALWAYS AND FIRST assess for suicide potential*-stop everything and assess for suicide patient (except CPR, or course) Low High High to moderate Low to moderate High Moderate to high, depends upon feasibility and ease of plan Moderate Low The use of , , and to Guns, ropes, knives kill self, make high risk suicide. Who is at higher risk for suicide, a man or a woman? Of: married, divorced, and separated, which marital status is highest risk for suicide? Lowest risk of suicide? Man Highest-separated then divorced Lowest-married The goal of action while the suicidal patient is still of the phone is to get person Another person on the scene (then immediately decreases risk) Remember: people who are alone are always high risk the . What are the four classic suicide precautions? Once the patient is admitted for attempted suicide should you ever discuss the attempt with them? Search personal belongings for drugs & alcohol, remove any sharp objects, remove any device for hanging or strangling; must be on constant one-to- one observation (NEVER out of sight) No, you should not focus on the attempt, focus on the present and future. -pathy Disease, suffering -penia Lack, deficiency of -sect To cut -plast Plastic surgery on a specified part -sclerosis Hardening of a tissue by: inflammation, deposition of mineral salt; an infiltration of connective tissue fibers -centesis A perforation or puncture -genic Produce, originate, become -emia Blood -otomy Butting -pexy Fixation of something -atresia Condition of occlusion -desis Binding, fusing -cele Combining form meaning a tumor or swelling or a cavity -cis Cut, kill -rhapy; -rrhapy Joining in a seam, suturation -scope; -scopy Instrument for observation -osis Indicates condition, process -oma Tumor -ostomy Surgical opening -stasis Stoppage -itis Inflammation -ology Study of; knowledge, science -lysis Breaking down -ectomy Surgical removal of -tripsy Crushing of something by a surgical instrument -ase Used in naming enzymes -gram; -graphy Write; record Syphilis is sexually transmiteed. (T/F) Syphilis first infects the . What are the stages of syphilis? Syphilis is a fatal disease if untreated. (T/F) What organism causes syphilis? What is the lesion like in primary syphilis? The chancres of syphilis are (painful/painless). Chancres disappear without treatment. (T/F) Late syphilis attacks which 3 body organs? What test CONFIRMS the presence of syphilis? What is the treatment of choice for syphilis? Why is penicillin administered with Procaine? With Probenecid? What is the most common sign of neurosyphillis? Mastitis and breast engorgement are more likely to occur in (primipara/multipara). Where does the organism that causes mastitis come from? Which organism most commonly causes mastitis? Prolonged intervals between breast-feeding (decrease/increase) the incidence of mastitis. Can too tight bras lead to mastitis? True Mucous membranes Primary, secondary, latent, late True Treponema palladium The chancre (pronounced shanker) Painless True Liver, heart, brain Dark-field illumination of the treponema palladium Penicillin Procaine makes the shot less painful; Probenecid blocks the excretion of penicillin Ataxia (gait problems) Primipara The infant's nose or mouth Staph Increase Yes, preventing emptying of ducts Mastitis usually occurs 10 at least after delivery. days When mastitis is present the breasts are Hard, swollen, warm , , and . Mastitis is accompanied by a fever over . If mastitis is caused by an organism, what causes breast engorgement? If mastitis occurs 1+ weeks after delivery, when does breast engorgement occur? Does breast engorgement interfere with nursing? What class of drugs is used to treat mastitis? Antibiotics are used to treat breast engorgment? (T/F) Application of (warm H2O compress/ice packs) is the preferred treatment for breast engorgement. The mother with mastitis should stop breast feeding. (T/F) If the mother has an open abscess on her breast, must not breast- feed. (T/F) For breast engorgement, the non-breastfeeding mother should be told to express breast milk. (T/F) What is the best treatment for breast engorgement? 102 degrees Temporary increase in vascular and lymph supply to the breast in preparation for milk production 2 to 5 days after delivery Yes, the infant has a difficult time latching on (getting nipple in its mouth) Antibiotics False Ice packs to decrease swelling False, the mother must keep breast feeding. (Offer unaffected breast first) True No, that would increase milk production and would make the problem worse (warm compresses or warm shower to let milk "leak" is okay- Ice is best) Breast-feeding - it will balance supply and demand What is mastoiditis? Inflammation/infection of the mastoid process What is the most common cause of mastoiditis? Chronic otitis media What are 4 signs and symptoms of mastoiditis? What unusual post- operative complication can result from mastoidectomy? What should you do to assess for facial nerve paralysis post- mastoidectomy? What is the medical treatment for mastoiditis? What is the surgery for mastoiditis called? Will a simple mastoidectomy worsen hearing? Should the nurse change the post- mastoidectomy dressing? What is a common side effect of mastoidectomy? What is a major nursing diagnosis post- mastoidectomy? In the chain of infection, hand washing breaks the mode of Drainage from ear, high fever, headache and ear pain, tenderness over mastoid process Facial nerve paralysis due to accidental damage during surgery (law suit time!) Have the patient smile and wrinkle forehead. Systemic antibitoics Simple or radical mastoidectomy No, a radical mastoidectomy may No, reinforce it. Physician changes first post op dressing Dizziness (vertigo) Safety Transmission . The best way to decrease nosocomial infection is sterile technique. (T/F) Sterile gloved hands must always be kept above the waist. (T/F) When putting on the second of a set of sterile gloves, you should grasp the cuff. (T/F) When putting on the first glove of a set of sterile gloves, you should grasp the cuff. (T/F) When putting on the second glove of a set of sterile gloves, you must not use the thumb of the first hand. (T/F) False, hand washing is the best way. True False, reach under the cuff with the tip of the gloved fingers. True True Airborne microorganisms travel Dust or water on or particles. Another name for medical asepsis is... Sensitivity (susceptibility) means... When unwrapping a sterile pack how should you unfold the top point? Clean technique The susceptibility of an organism to the bacterial action of a particular agent Away from you Virulence means.... Ability of an organism to produce disease Another name for surgical asepsis is... What is the best location in a client's room to set up a sterile field? Medical aseptic technique are aimed at reducing the number of organisms (T/F) What does bacteriostatic mean? What does bacteriocidal mean? What does nosocomial infection mean? When pouring liquid onto a sterile field you should pour from a Sterile technique On the over-bed table True, doesn't eliminate all of it just decreases the number Having the capability to stop growth of the bacteria Having the capability to kill bacteria. Infection acquired through contact with contamination in the hospital 6 to 8 height of to inches above sterile field. When you plan to use gloves for a procedure you do not need to wash hands before it. (T/F) False, always wash even if you plan to use gloves Culture means.... Growing colony of organisms, usually for the purpose of identifying them Surgical aseptic techniques render and keep articles free from all organisms. (T/F) You must never turn your back to a sterile field. (T/F) What must you do if you reach across a sterile field? Micro-organisms grow True True Consider the area contaminated and not use the articles in the area Warm, dark, moist best in a , , place. It is common practice to regard the edges of any sterile field as contaminated. (T/F) Immediately after opening a bottle of sterile water, can you pour it directly into a sterile basin? Which is the best method for identifying clients accurately? An emulsion is a mixture of and . Syrups and elixirs are of particular concern to diabetic clients because.... Oral medications have a (faster/slower) onset of action that IM drugs. Oral medications have a (shorter/longer) duration of action than IM medications. How should drugs that stain teeth be administered? A drug given by a parenteral route acts outside the GI tract. (T/F) Name the four most common parenteral routes of administrations. When blood is administered by IV, the needle/catheter should be gauge. You can administer up to cc of a drug per site by IM injection in adults. Children should receive no more than cc per site by IM injection. The preferred IM injection site for children under 3 is the True, the outer 1 inch is considered contaminated. You must not touch it with your sterile gloves. No, you must pour a few cc's out of the bottle into a waste container before you pour into the sterile basin. (This is called "lipping" the bottle) By ID name-band Oil and H2O they contain sugars Slower Longer By a straw True SQ, IM, IV, ID (intradermal) 18 gauge 3 cc 2 cc Vastus lateralis . Why is the dorsogluteal site not recommended for IM injection the children less than 3 years of age? Can 3 cc of fluid be administered per IM into the deltoid of an adult? The #1 danger when using the dorsogluteal site for IM injection is . The preferred angle of injection to to be used for IM administration is . The preferred length of needle to administer an IM injection is... The preferred gauge of needle for IM injection is... Which type of medications are given by Z-track injection? How long is the needle kept inserted during Z- track injection? What must be done to the equipment before injecting by Z-track method? When giving a Z-track injection, the overlying skin is pulled (up/down/medially/latera lly). Subcutaneous injection must be given at 45 degrees. (T/F) The preferred gauge of needle for injection for SQ injection . The preferred length of needle for SQ injection is . The intradermal route is primarily used for . Name the two sites used for intradermal injection. Because the muscle is not well developed yet. No, maximum of 1 cc Damage to the sciatic nerve 90 degrees 1 to 2 inch 21 to 22 gauge Irritating, staining 10 seconds Change the needle Laterally True (for boards), false- whatever angle gets it SQ without going IM 25 gauge 5/8 inch Skin testing Inner forearm Upper back In general, the nurse should wear gloves when applying skin preparations such as lotions. (T/F) After using nose drops, the client should remain for minutes. Strict aseptic techniques is required when administering a vaginal medication. (T/F) Before administering vaginal medications the client is more comfortable if you ask them to . After administration of a vaginal durg the client should remain for minutes. Rectal suppositories with an oil base should be kept refrigerated. (T/F) Strict sterile technique is required when administering a drug per rectum. (T/F) The best way to ensure effectiveness of a rectal suppository is to... A rectal suppository is inserted inches in an adult and inches in a child. The client should remain supine for 5 minutes after having received a rectal suppository. (T/F) A suppository given rectally must be lubricated with a water soluble lubricant. (T/F) Eye medications can be given directly over the cornea. (T/F) Eye drops should be placed directly into the . True Supine, 5 False-- only "clean" technique or medical asepsis is necessary Void Supine, 10 True False, clean or medical asepsis Push the suppository against the wall of the rectum 4,2 False-- they should be lying on their side for 5 minutes, not supine True, lubricant fingers also False, into the conjunctival sac, never the cornea; hold the dropper 1/2 inch above the sac Conjunctival sac To prevent eye medications from getting into the systemic circulation you apply pressure to the for seconds. The eye should be irrigated so that the solution flows from outer to inner canthus. (T/F) If ear medications are not given at room temperature the client may experience... To straighten the ear canal in the ADULT, the nurse should pull the pinna and . To straighten the ear canal in the young CHILD under 3 the pinna should be pulled and . After receiving ear drops the client should remain in position for minutes. How far above the ear canal should you hold the dropper while administering ear drops? Liquid doses of medications should be prepared at level. Liquid drugs should be poured out of the side (opposite of/the same as) the label. It is safe practice to administer drugs prepared by another nurse. (T/F) In order to leave drugs at the bedside you must have a physician's order. (T/F) Young infants accept medication best when given with a . Nasolacrimal sac, 10 (press between the inner canthus and the bridge of the nose) False, it must flow from inner canthus to outer (alphabetical: I to O) Dizziness, nausea Up and back Down and back Side lying, 5 1/2 inch Eye Opposite False True Dropper It is safe practice to recap needles after injection. (T/F) What do you do if you get blood in the syringe upon aspiration? False, Never re-cap Remove the syringe immediately and apply pressure; you must discard the syringe and redraw medication in a new syringe Tagamet Give with meals, remember Zantac does not have to be given with meals Capoten Give on empty stomach, one hour before meals (antihypertensive) Apresoline Given with meals (antihypertensive) Iron with nausea Give with meals Sulfonamides Take with LOTS OF WATER regardless of whether you give it at mealtime or not -- Bactrim, Septra, Gantricin, ie, used to treat UTI Codeine Take with lots of water rergardless of meals -- to prevent constipation Antacids Give on empty stomach I hour ac and hs Ipecac Give with 200-300 cc water-- not related to mealtime -- this is an emetic (to make you vomit after ingestion of poisons -- don't give if the poisons were caustic, or petroleum based) Rifampin Give on empty stomach (anti- tuberculosis) remember Rifampin causes red urine Non-steroidal anti- inflammatory drugs Give with food (for arthrosis) Aldactone Give with meals (K--sparing diuretic) Iron (without nausea) Give on empty stomach with orange juice to increase absorption Penicillin Give on empty stomach Erythromycin Give on empty stomach (antibiotics) Stool Softeners Take with lots of water regardless of mealtim Griseofulvin Give with meals-- especially high fat meals (anti-fungal) Tetracycline Do not give with milk products, do not give to pregnant women or children before age 8 or damage to tooth enamel occurs Theophylline derivative Give with meals, ie, Aminophylline, Theodur (anti-asthmatic bronchodilator) Steroids Give with meals-- remember taper the patient off these drugs slowly Pancreas pancreatin isozyme Para-amino salicylate sodium (PAS) Give with meals-these are oral enzymes used with children with cystic fibrosis to increase the absorption of the food they eat Give with meals/food-- anti tuberculosis Colchicine Give with meals -- anti gout, remember if diarrhea develops, stop the drug Thorazine Take with LOTS OF WATER regardless of meals to prevent constipation. All drugs that end in "-zine" are major tranquilizers that also cause Psuedo Parkinson's or extra-pyramidal effects. Carafate and sulcrafate Give on empty stomach 1 hour before meals and at bedtime -- remember these coat the GI tract and interfere with the absorption of other medications (give them by themselves) Allopurinol Give with meals and give with lots of water--anti uric acid--- used to treat gout and the purine build up seen in chemotherapy for cancer Define Meniere's Disease What is the famous triad of symptoms in Meniere's? Does Meniere's occur more in men or women? What should the client do if they get an attack? What safety measures should be followed with Meniere's? What age group in Meniere's highest in? What can PREVENT the attacks of Meniere's? What electrolyte is given to people with Meniere's? What is the surgery done for Meniere's? What disease often follows labyrinthectomy? What is the activity order after labyrinthectomy? When surgery is performed for Meniere's, what are the consequences? What should the client avoid after labyrinectomy? What type of diet is the client with Meniere's on? An increase in endolymph in the inner ear, causing severe vertigo. Paroxysmal whirling vertigo -- sensorineural hearing loss--tinnitus (ringing in the ears) Women Bed Rest Side rails up x 4, ambulate only with assistance 40 to 60 Avoid sudden movements Ammonium chloride Labyrinthectomy Bell's palsy-- facial paralysis, will go away in a few months Bed rest Hearing is totally lost in the surgical ear Sudden movements and increased Na food Low salt What two classes of drugs are given in Meniere's? Meningitis is an inflammation of the of the and spinal . Meningitis can be caused by , , and . The four most common organisms that cause meningitis are... The child with meningitis is most likely to be (lethargic/irritable) at first. What visual symptom will the patient with meningitis have? What is the most common musculo- skeletal symptom of meningitis? Will the patient with meningitis have a headache? Kernig's sign is positive when there is pain in the when attempting to straighten the leg with flexed. What type of vomiting is present in meningitis? What is the definitive diagnostic test for meningitis? If the patient has meningitis, the CSF shows pressure, WBC, protein, glucose. On what type of isolation will the patient with meningitis be? How long will the patient with meningitis be on these precautions? Antihistamines and diuretics (Diamox) Linings, brain , cord Viruses, bacteria, chemicals Pneumococcus Meningococcus Streptococcus H. influenza Irritable Photophobia (over-sensitivity to light) Stiff neck- nuchal rigidity Yes Knee; hip Projectile Lumbar puncture with culture of CSF (cerebro-spinal fluid) Increased, increased, increased, decreased Contact and respiratory precautions Until they have been on an antibiotic for 48 hours The room of a patient with meningitis should be and . The client with meningitis can Dark and quiet Seizures develop . What is opisthotonos? Arching of back (entire body) from hyperextension of the neck and ankles, due to severe meningeal irritation. If a patient has opisthotonos, in what position would you place them? Average duration of menstrual flow is . The normal range is to days. Average blood loss during menstruation is cc. Name the two phases of ovarian cycle. In the menstrual cycle, day 1 is the day on which... How long does an ovarian cycle last? How many days after ovulation does menstruation begin? What hormones are active during follicular phase? During the luteal phase of the ovarian cycle, which of the following hormones increase: estrogen, progesterone or LH? What is the major function of the luteal phase of the ovarian cycle? If an ovum is fertilized during the luteal phase what hormone will be secreted? During menstruation, the average daily loss of Side-lying 5 days, 3 to 6 50 to 60 cc Follicular phase (first 14 days) Luteal phase (second 14 days) Menstrual discharge begins Average of 28 days 14 days FSH and Estrogen Progesterone and LH To develop and maintain the corpus luteum which produces progesterone to maintain pregnancy until placenta is established. HCG (human chorionic gonadotropin) 0.5 to 1.0 mg iron is mg. What occurs during the follicular phase of the ovarian cycle? What type of environmental modification is best for a migraine? The long term treatment of migraine focuses upon... What type of pain is typical of migraines? Are migraines more or less common in men? Besides pain, people with migraines complain of what other symptoms? What are the processes occurring in migraines? Where is the pain of migraine most likely located? Name a drug given to treat migraine? Are migraine headaches usually unilateral or bilateral? When Inderal is given in migraine headache, it is used to prevent or treat an attack? MS is a progressive disease of the CNS. Myelin promotes , of nerve impulses. MS affects men more than women. (T/F) What age group usually gets MS? MS usually occurs in (hot/cool) climates . What is the first sign of MS? MS can lead to urinary incontinence. (T/F) MS can lead to impotence in males. (T/F) It accomplishes maturation of the graafian follicle which results in ovulation Dark and quiet environment Assessing things that bring on stress and then planning to avoid them. Throbbing Less Nausea, vomiting and visual disturbances Reflex constriction then dilation of cerebral arteries. Temporal, supraorbital Sansert (methsergide), Cafergot (Prophylaxis: Imipramine) Unilateral To prevent. It DOES NOT treat. Demyelinating Fast, smooth conduction False 20 to 40 Cool Blurred or double vision True True Patients with MS should be taught to walk with a - gait. Why are Adrenocorticotropic Hormone (ACTH) and prednisone given during acute MS? For acute exacerbations of MS per IV is often used. What drug can be given to treat urinary retention in MS? Will the muscles of MS clients be spastic or flaccid? What three drugs can be given for muscle spasms? Baclofen causes (constipation/diarrhea) Dantrium causes (constipation/diarrhea) Patient's with MS should have (increased/restricted) fluids. The diet of a patient with MS should be -- ash. What major sense is affected most in MS (besides vision)? Which will bring on a MS exacerbation: over- heating or chilling? In Myasthenia Gravis (MG) there is a disturbance in transmission of impulses at the . The #1 sign of MG is . What is the unique adjective given to describe the early signs of MG? MG affects men more than women. (T/F) Wide based To decrease edema in the demyelination process ACTH (Corticotropin) Urecholine, Bethanocol Spastic Valium, Baclofen (Lioresal), Dantrium Constipation Diarrhea (hint: D's go together, Dantrium and Diarrhea) Increased to dilute urine and reduce incidence of UTI. Acid Tactile (touch)-- they burn themselves easily Both will; but they tend to do better in cool weather (summer will always be a bad time for MS patients) Neuromuscular junction Severe muscle weakness The early signs (difficulty swallowing, visual problems) are referred to a BULBAR signs. False, affects women more than men When women get MG they are usually old or young? When men get MG they are usually old or young? What neurotransmitter is problematic in MG? What class of drugs is used to treat MG? What ending do anticholinesterases have? Are anticholinesterases sympathetic or parasympathetic? Anticholestinesterases will have (sympathetic/cholinergic ) side effects. What surgery CAN be done for MG? The severe muscle weakness of MG gets better with exercise. (T/F) What will the facial appearance of a patient with MG look like? If a patient has MG, what will be the results of the Tensilon Test? Besides the Tensilon Test, what other diagnostic tests confirm a diagnosis of MG? What is the most important thing to remember about giving Mestinon and other anticholestinerases? Do you give anticholestinerases with or without food? What type of diet should the patient with MG be on? What equipment should be at the bedside of an MG patient? Name the two types of crises that a MG patient can have. Young Old Acetylcholine Anticholinesterases -stigmine Parasympathetic Cholinergic (they will mimic the parasympathetic nervous system) Thymectomy (removal of thymus) False, it is worse with activity Mast-like with a snarling smile (called a myasthenic smile) The patient will show a dramatic sudden increase in muscle strength Electromylogram (EMG) They must be given EXACTLY ON TIME; at home, they might need to set their alarm With food, about 1/2 hour ac; giving ac helps strengthen muscles of swallowing Soft Suction apparatus (for meals), tracheostomy/endotube (for ventilation) Cholinergic (too much Mestinon) Myasthenic (not enough Mestinon) The #1 danger in both Myasthenic and Cholinergic crisis is . What words will the client use to describe the pain of an MI? Respiratory arrest Crushing, heavy, squeezing, radiating to left arm, neck , jaw, shoulder What is an MI? Either a clot, spasm or plaque that blocks the coronary arteries causing loss of blood supply to the heart and myocardial cell death What is the #1 symptom of an MI? Males are more likely to get an MI than females. (T/F) Due to MI occurs within of symptom onset in 50% of all patients. What pain medication is given for the pain of a MI (Give three). What is the reason for giving post MI patients ASA? Name a new drug with anti-platelet activity. The three most common complications after MI are , , and . Give another name for an MI. What will the activity order be for the post-MI client? What is the most common arrhythmia after a MI? What cardiac enzymes indicate an MI? What serum protein rises soonest after myocardial cell injury? Do people without cell damage have troponin in their blood? How soon after cell damage does troponin increase? When will the client with an MI be allowed to engage in sexual intercourse after an MI? Severe chest pain unrelieved by rest and nitroglycerine True One hour Morphine, Demerol, Nitroglycerine To prevent platelets from forming clots in the coronary arteries Plavix Cardiogenic shock, arrhythmia, CHF Heart attack Bed rest with bedside commode Premature ventricular contractions (PVCs) Elevated CPK, LDH, SGOT Troponin No it is only present when myocardial cells are damaged. As soon as 3 hours (can remain elevated for 7 days) 6 weeks after discharge Will fluid resuscitation (administering large amounts of IV fluid) treat cardiogenic shock? Will the client with a MI be nauseated?...diaphoretic ? What will the extremities of the client with a MI feel like? What is the permanent EKG change seen post MI? Of CPK and LDH which rises earliest? What drug will be used to treat PVCs of MI? Will the client with a MI need 100% O2 for their entire stay in the hospital? What information does the measurement of skin fold thickness yield? In general, males have a higher risk of heart disease than females. (T/F) Post-menopausal females have a lower risk of heart disease than males aged 25-40. (T/F) Family history of diabetes increases the risk fo heart disease. (T/F) Family history of liver disease increases the risk of heart disease. (T/F) Cigarette smoking increases the risk of heart disease. (T/F) Oral contraceptives decrease the risk of heart disease. (T/F) Routine exercise decreases the risk of heart disease. (T/F) No, you must use cardiac drugs (giving IVs and blood will not help this kind of shock) yes, yes Cold, clammy ST wave changes CPK Lidocaine No, just moderate flow (42% or 3 to 6 liters for first 48 hours) The amount of body fat True False. They have a higher risk. True False True False, use increases the risk True What is done in a graft for hemodialysis? What is done in an AV fistual? Does anything exit the skin in an AV fistula? How long can an AV fistula be used? Who is the most likely to receive a graft for dialysis? How often do clients with renal failure undergo dialysis? Is hemodialysis short term or long term? How long does the average dialysis last? What are 3 ways to gain access to the circulation in hemodialysis? What is the most common site for an AV shunt? What should be avoided in the arm of the client with an AV shunt? What syndrome results when too much fluid is exchanged during hemodialysis too quickly? What are the symptoms of disequilibrium syndrome? Does anything exit the skin in an AV shunt? How long can AV shunt be used? Hemophilia is a disorder. Hemophilia A is a deficiency of Factor # . During an acute bleeding episode, you should apply for 15 minutes and apply . The inheritance patterns for hemophilia is: A blood vessel is sutured between an artery and a vein. A surgical anastomosis is made between the artery and a vein. No Indefinitely People with diabetes mellitus. 3 times per week Both- but most short term dialysis is achieved by hemodialysis 4 to 6 hours AV shunt AV fistula AV graft Radial artery to radial vein No venipuncture or blood pressure allowed in the arm with a shunt, graft or fistula. Disequilibrium syndrome Change in LOC N/V Headache Twitching Yes, the plastic tube that connects the artery and vein outside the arm Just for a few weeks Bleeding VIII Pressure, ice Sex linked recessive In hemophilia, the PTT is (up/down), the coagulation or clotting time is (up/down) and the platelet count is (up/down). What does hemarthrosis mean? During bleeding into the joints you should (mobilize/immobilize) the extremity. To treat hemarthrosis you should the extremity above the . What is the name of frozen factor VIII given to hemophiliacs? Once you have stopped the bleeding into the joint, how long should the hemarthrosis patient wait before bearing weight or doing range of motion? What drug can you apply topically to stop bleeding? Which of these symptoms are NOT seen in hemophilia? Prolonged bleeding, petechiae, ecchymosis or hematoma? Hepatitis is an , disease of the . Hepatitis A,B,C and D are all (bacterial/viral) diseases. An early sign of hepatitis A is . Early stage hepatitis often looks like the . In later stages of hepatitis, the turns dark. What does pre-icteric mean? Up (increased or longer) Up (increased or longer) Neither (hemophilia does not affect platelets) Bleeding into the joints Immobilize to prevent dislodging the clots that do form. Elevate, heart Cryoprecipitate 48 hours Epinephrine, or topical fibrin foam Petechiae Acute, inflammatory, liver Viral Anorexia or fatigue Flu Urine The stage BEFORE the patient exhibits jaundice. What is the icteric stage? What skin symptoms do you see in hepatitis? (Give 2) Which disease has more severe symptoms-- Hepatitis A or B? Patients with hepatitis have an aversion to . In hepatitis the are light colored. What is the common name for Herpes Zoster? What type of rash occurs with shingles? How long does it take for shingles to heal? Who is the most common subjective symptoms of shingles? What three drugs are given for shingles? What other disease is related to shingles? What organism causes shingles? What is the #1 nursing diagnosis with shingles? When the patient exhibits jaundice. Pruritis (itching) Jaundice (Both are due to bilirubin accumulation) Hepatitis B Cigarettes Stools: remember the urine is dark and stools are light. (Bilirubin ends up in the skin and urine instead of the stool where it should have gone.) Shingles A vesicular rash over the pathway of a sensory nerve 30 days Pain, pain, Pain Acyclovir (anti-infective) Tegretol (anticonvulsant--given to stabilize nerve cell membranes) Steroids (anti-inflammatory) chickenpox Varicella--herpes zoster Alteration in comfort: pain, #2 Impaired skin integrity Hepatitis A Enteric precautions Fecal/oral route of transmission Incubates 3 to 5 weeks Vaccine available (Can give immune globulin after exposure) HAsAg (this is what the blood test show) Hepatitis A surface Antigen Hepatitis B Watch those needles HBsAg (this is what blood tests show) Hepatitis B surface antigen HBIG - vaccine Vaccination available, can give immune globulin after exposure Transmitted by blood and body fluids Incubates 5 to 35 weks Hepatitis C Watch those needles Incubates 2 to 23 weeks Transmitted by blood only No vaccine, immune globulin doesn't work Which types of client should have their toenails trimmed only by an MD? Two purposes of bed bath are... The typical hospital client (should/should not) wear their dentures. What type of movement should be used for cleansing eyes? Before applying elastic hose the nurse should... Clients on what class of drugs should use an elastic razor? When a client is unable to hold his dentures firmly in his mouth, the nurse should... How often should mouth care be performed for those clients on oxygen? Should lemon and glycerine swabs be used to cleanse the mouth? How should a client's toenails be trimmed? Are nurses permitted to give perineal care to clients of the opposite sex? Clients on what type of therapy must use a safety blade razor (non electric)? How should a nurse carry soiled linen? When giving a bed bath, on which body party should the nurse begin to work? Give three reasons for giving a back rub. The greatest danger in placing water in the mouth of the unconscious patient during oral hygiene is... When shaving a client, water used should be more (hot/cold) than bath water? Diabetics, peripheral vascular disease, very thick nails Cleanses the skin Provides comfort Should Inner to outer canthus Elevate the clients legs for 3 to 5 minutes to decrease venous stasis Anticoagulants (heparin/coumadin/lovenox) Leave them out Every 2 hours No, they are not cleansing agents. They are used AFTER cleansing as a moistening agent Straight across Yes, nurses are permitted to give perineal care to clients of the opposite sex. Oxygen therapy, since an electric razor could cause sparks In a neat bundle held away from the body. The eyes Comfort Stimulate circulation and muscles Relaxation Aspiration Hot What does evening or hour of sleep (HS) care consist of? Oral hygiene Washing face/hands Back rub Tightening linens What is dentifrice? Agents which promote adherence of dentures to gums, ie, Polygrip What is sordes? Crusts on the tongue and gums due to improper oral hygiene What action will facilitate the trimming of brittle toenails? Should the client roll the elastic stocking down to wash legs? Why or why not? Elastic stockings should be removed for the bath. (T/F) When should a patient put on TED hose? Hyperemesis Gravidarum is and vomiting that persists into the trimester. Give three possible causes of hyperemesis gravidarum. Has hyperemesis gravidarum ever been associated with mixed feelings about pregnancy? What are the two most common complications of hyperemesis gravidarum? What is the initial diet order for clients with hyperemesis gravidarum? Why are doctors cautious in using antiemetics to treat hyperemesis gravidarum? What are the instructions given to clients recovering from hyperemesis gravidarum in relation to mealtime? What is the biggest challenge in nursing care of the client with hyperemesis Soaking in warm water No, it can cause a constricting band around the ankle/foot. True Before getting out of bed (before the swelling occurs). Severe and prolonged; 2nd trimester (normal vomiting should be gone before 2nd trimester) Pancreatitis Multiple pregnancies Hydatidiform mole Yes, increased incidence of it in women who are ambivalent about pregnancy Electrolyte imbalance (dehydration) Starvation NPO They don't want to harm the fetus Remain seated upright for 45 minutes after each meal Getting them to eat Hypertension is an or sustained elevation in the (systolic/diastolic) . Hypertension is often fatal if untreated. (T/F) Hypertension is more common in blacks or whites? Aging decreases the risk of hypertension. (T/F) Obesity increases the risk of hypertension. (T/F) Oral contraceptives (increase/decrease/do not effect) the blood pressure. What four organs does hypertension affect the most? How many measurements must be made before you can say a person has hypertension? What blood pressure is considered to be hypertension? Which pressure is most damaging, an increased (systolic/diastolic)? When a doctor takes three different blood pressure readings at different times, how far apart must the measurements be made? Can hypertension be cured? What class of drugs is used to first treat hypertension? Name the two most common dietary prescriptions used to treat hypertension? What two non-dietary lifestyle changes are used commonly to treat hypertension? Intermittent, diastolic blood pressure True Blacks False, it increases the risk True Increase Brain (stroke) Eyes (blindness) Heart (MI) Kidney (renal failure) At least three Anything greater than 140/90 mm Hg An increased diastolic At least one week No, just treated Diuretics Calorie reduction for weight loss Sodium restriction Decreases stress Increase activity When you take the blood pressure of the client with hypertension you would measure - , with the client , and . What do caffeine and smoking do to blood pressure? What is the #1 side effect of antihypertensives? Would vasodilators or vasoconstrictors treat hypertension? Would sympathetic stimulators or sympathetic blockers treat hypertension? In hypovolemic shock there is a in the circulating volume -- this tissue perfusion with . What gauge catheter would you use to start an IV in hypovolemic shock? What is the #1 cause of hypovolemic shock? What happens to the blood pressure in hypovolemic shock? What happens to the pulse pressure in hypovolemic shock? How do you calculate the pulse pressure? If J. Doe's blood pressure is 100/60, what is his pulse pressure? What is the normal pulse pressure? In hypovolemic shock the level of consciousness (LOC) is (increased/decreased). Which heart rate is associated with hypovolemic shock, bradycardia or tachycardia? Both arms; lying, sitting and standing Increase it Orthostatic hypotension (means you feel weak when you rise to a standing position because your blood pressure falls) Vasodilators (decreases resistance) Sympathetic blockers (decrease cardiac output and decrease resistance) Decrease; blood; decreases; oxygen 16 or larger Acute blood loss It decreases It narrows (becomes a smaller number) You subtract the diastolic from systolic 40 (100-minus 60 equals 40) 40 (+ or -10) Decreased Tachycardia In hypovolemic shock the output of urine will be less than cc per hour. The client's skin will be , , and . Which acid-base disorder is MOST commonly associated with hypovolemic shock? Of all the following, which one(s) increase in hypovolemic shock? Blood pressure, output, heart rate, pH, LOC, pulse pressure, respiratory rate What are the first two sings of hypovolemic shock? What is the #1 medical treatment of hypovolemic shock 25 to 30 cc Cool, pale, clammy (due to arterial constriction to shunt blood from skin to vital organs) Metabolic acidosis (due to lactic acid accumulation- no oxygen = anaerobic metabolism) Only the heart rate and respiratory rate Change in LOC and tachycardia Replace blood and fluids What are mast trousers? Pneumatic device placed around the legs and lower body that is inflated to force blood centrally Do clients in hypovolemic shock have to have a Foley inserted? In what position would you place a client in suspected hypovolemic shock? How often are vital signs measured in hypovolemic shock? If the blood pressure (systolic) falls below 80 mmHg, what would you do first in hypovolemic shock? Yes, to measure urine output (when output is >30 cc per hour the shock has resolved) On back with arms and legs elevated Every 15 minutes Increase the oxygen flow rate What is a hysterectomy? It is surgical removal of the uterus How long must a woman wait before having intercourse after hysterectomy? Is the woman likely to have a foley catheter in after a hysterectomy? 4 to 6 weeks Yes Are enemas common before a hysterectomy? What would you do if the client complains of flank pain (back pain) after hysterectomy? What are 2 common psychological reactions to hysterectomy? What causes thrombophlebitis after hysterectomy? What sign would indicate the presence of thrombophlebitis? Should you assess for Homan's sign? How long does the woman have to be off oral contraceptives before hysterectomy? How long should a woman wait before lifting heavy objects after a hysterectomy? How long does a lady have to wait before driving after a hysterectomy? If the client complains of abdominal gas after a hysterectomy, the best intervention is..... What are two major complications of a hysterectomy besides hemorrhage? What body position should be avoided after hysterectomy? Why? When will bowel sounds return after a hysterectomy? Ectopic pregnancy is implantation of a fertilized ovum the . The most common site for ectopic pregnancy is in the . Yes Call the MD, probably had a ureter tied off accidentally in surgery Grief, depression Venous stasis in the abdomen (the woman was in the vaginal lithotomy position for hours) A hard, red swelling in the posterior calf No. Homan's sign is no longer recommended as a test for thrombophlebitis because it can cause a clot to embolize Oral contraceptives should be discontinued 3 to 4 weeks preoperatively. 2 months 3 to 4 weeks Ambulation Thrombus and pulmonary embolus Urinary retention Knee flexion (because it increases the chance of thrombophlebitis) After 24 hours but before 72 hours Outside, uterus Fallopian tube - 90% Have intrauterine devices to prevent pregnancy ever been linked to ectopic pregnancy? What is the most common sign of fallopian tube ectopic pregnancy? What is the most dangerous side effect/complication of fallopian ectopic pregnancy? If the fallopian tube ruptures due to ectopic pregnancy, nursing care is the same as that for . The uterus feels after rupture of a fallopian ectopic pregnancy? The first sign that a fallopian ectopic pregnancy had ruptured is... Ectopic pregnancy is (usually/almost never) carried to term. The most common medical-surgical treatment for ectopic pregnancy is . Name the surgery performed for an ectopic pregnancy. Yes and so have pelvic infections. Unilateral pelvic pain Rupture of the fallopian tube Shock and peritonitis Boggy- tender, also Sharp abdominal pain Almost never Surgical removal of fetus and some surrounding tissue Exploratory laparotomy What is ECT? The use of electrical shock current delivered to the brain to induce a seizure that treats depression. The client is (awake/under local anesthesia/under general anesthesia) during ECT? What conditions does ECT treat? Is an informed consent necessary for ECT? Under general anesthesia -- must be artificially ventilated Depression primarily Yes Name the three most common complications of ECT? What class of drugs is given with ECT? What intellectual ability is impaired after ECT? How long will a client's memory be impaired after ECT? Immediately after ECT, how will the client normally act? In what position should the client be immediately after ECT? What typical pre- operative type of orders will be ordered before ECT? The convulsion (seizure) that the electrical current produced is violent. (T/F) What does an EEG measure? When are there activity restrictions after an EEG? Should the client wash his hair before an EEG? What would you tell a client who says what if I get shocked during my EEG? Does a client have to be NPO before an EEG? What instructions are MOST important to give a client during an EEG? What should the client do after an EEG? Should sedatives be given before an EEG? How much sleep should the client get the night before an EEG? Do you need a signed informed consent for an EEG? Aspiration of emesis (most common) into the lung Dislocations of joints Fractures due to convulsion-- rare today Muscle relaxant -- succinylcholine Memory 2 to 3 weeks Drowsy Dull Apathetic On their side-- to prevent aspiration NPO after midnight Remove dentures Client to void before surgery Side rails up False, it used to be, but it isn't any more with the use of muscle relaxants Measures electrical activity generated by the brain ONLY when sedatives are used, and then it's only necessary to keep side rails up. Yes That is impossible since the test measures electrical activity coming FROM him, never to him. No, they should never be NPO, it could cause hypoglycemia and alter the EEG results. Try not to move Wash their hair Only if ordered as a pre-test medication. At least 4 to 5 hours--unless it is a sleep deprivation EEG No Should caffeine be limited before an EEG? What will excessively fatty stool be like? What are the large, pale, foul smelling, greasy stools called? Name the three types of parasites abnormally found in stool. What does occult blood in the feces mean? Are fats a normal constituent of feces? A decrease in urobilin in stool results in stool that is . Name two things for which stool specimens are tested. Is blood a normal constituent of feces? Yes. It should be eliminated for 24 hours before the test. Large, pale, foul smelling, greasy Steatorrhea Roundworm Tapeworm Pinworm Bleeding somewhere in the GI tract Yes but it should be WNL Clay-colored Occult blood, fat, ova and parasites No What is melena? A black, tarry stool indicating a GI bleed What position is best for clients with emphysema under normal circumstances? What flow rates of O2 are appropriate for the client with emphysema? If a client with emphysema has a severe dyspneic episode what position is best? What will you observe on the hands of the client with emphysema? In emphysema, the alveoli are over- and under- . The development of emphysema is most associated with a history of . In emphysema, the appetite the weight and the anterior-post diameter of the chest . What is the increase in anterior-posterior diameter of emphysema called? Semi-fowlers or higher Low flow -- <2.5 L/min; never exceed 2.5L in COPD Sitting upright with arms folded on the overbed table Clubbing of the fingernail beds Over-enlarged, under-ventilated so that air is trapped in alveoli Smoking Decreases, decreases, increases Barrel chest The person with emphysema have , lips and (slow/rapid) breathing. What dietary prescription is most appropriate for the client with emphysema? What fluid order should the emphysema client have? The client with emphysema is (ruddy/pale/cyanotic). Hyperthyroid (High metabolism) High growth hormone in a child (give another name) Over secretion of mineralcorticoids only (give another name) Low growth hormone (give another name) High growth hormone in an adult. Under-secretion of adrenal cortex Hypothyroidism in an adult. Over secretion of adrenal cortex Over secretion of adrenal medulla Grunting, pursed, rapid Frequent small meals to prevent tiring 3 liters of fluid per day (this is an increase) Cyanotic Graves Disease Gigantism Conn's disease Pituitary dwarfism Acromegaly Addison's disease Myxedema Cushing's syndrome Pheochromocytoma Hypothyroid in a child Cretinism Oversecretion of ACTH Cushing's disease What is endometriosis? Growth of endometrial tissue outside of uterus Endometriosis most commonly occurs in women between ages of and . After menopause, endometriosis (decreases/increases). What is the MOST common side effect of endometriosis? What is the major complication of endometriosis? 25 to 40 Decreases Dysmenorrhea (painful menstruation) Infertility What diagnostic procedure confirms the diagnosis of endometriosis? What class of drugs is used to conservatively treat endometriosis? Which androgen drug is most commonly used to treat endometriosis? Women with endometriosis should be counseled to use (tampons/pads) during menstruation? Will client die of endometriosis? What would you say? What advice is best for women with endometriosis who want to have children? What is the #1 danger of epiglottitis? Epiglottitis most commonly occurs in children from age to . What organism causes epiglottitis? What level of fever is present in epiglottitis? What symptoms are classic epiglottitis? Will a child with epiglottitis cough? How will the child with epiglottitis breathe? If a child is suspected of having epiglottitis, should you put a tongue depressor in their mouth to look? Would you do a throat culture for a child with epiglottitis? If epiglottitis is suspected, what should the parents be told? What drug is used to fight epiglottitis? Laparoscopy Androgens Danazol Pads only Not life-threatening Do not postpone pregnancy, may not be able to have children Airway obstruction 1 to 8 years Hemophilus influenza B Over 102 degrees Muffled voice Drooling Stridor No, there will be a lack of spontaneous cough. Leaned forward with flaring nostrils No, never put any instrument in the child's mouth unless you are prepared to do an immediate intubation. No, never put anything in their mouth. To take the child to the ER as soon as possible. Penicillin, ampicillin Children with epiglottitis often need a tracheotomy. What behavior would indicate the need for a tracheotomy? What is recommended for the prevention of epiglottitis? Autonomy vs Shame and Doubt Restlessness Increased HR Retractions All children two months and over should receive an H. influenza B vaccine. Toddler Industry vs Inferiority School Age 18 to 25 years Young Adult Says "no" Toddler Encourage creativity and collecting things School Age Give choices Toddler Centers on having basic needs met Infancy 18 months to 3 years Toddler 3 to 6 years Pre-schooler 12 to 20 years Adolescent Initiative vs Guilt Pre-schooler 6 to 12 years School age Trust vs Mistrust Infancy Peer group important Adolescent Encourage fantasy Pre-schooler Identity vs Role confrontation Adolescent Intimacy vs Isolation Young adult Birth to 18 months Infancy Define EGD Insertion of a fiber optic scope to visualize the esophagus, stomach and duodenum What can be done during an EGD besides visualization? Can EGD be done on an uncooperative client? Does client need to have side rails up after EGD? Can an EGD be done on clients with GI bleeding? Is the client sedated before EGD? What pre-test activities must be performed before the EGD? When can an EGD client begin to eat after the test? Remove polyps Take specimens Coagulate bleeding vessels No Yes, until sedative effects of valium have worn off Yes Yes, with valium (diazepam) or another sedative Remove dentures and eyeglasses Sign consent NPO after midnight When gagg reflex returns (knocked out with xylocaine) Is an EGD a fasting procedure? What drug is given to anesthetize the pharynx? What are the complications of EGD? What two discomforts are common during an EGD? What is the most dangerous complication of EGD? What is the most common complaint after an EGD? Carbonic Anhydrase Inhibitors Yes, after midnight Xylocaine (a local anesthetic) Perforation of gut Aspiration secondary to emesis Respiratory arrest (due to valium) Vomiting Gagging Secondary respiratory arrest (valium) Sore throat Treat glaucoma Decreases aqueous humor production Diuresis Diamox is an example Anticholinergic Dilates pupils Causes photophobia Used preoperatively for cataract removal Don't use in glaucoma Atropine is an example Miotic Constricts pupil; Timoptic Pilocarpine are examples Mydriatic Tachycardia Photophobia Dilates pupil Do not use in glaucoma What do carbonic anhydrase inhibitors do to the eye? Name the most common side effect of carbonic anhydrase inhibitors? Which two groups of these drugs cause photophobia? Which of these classes of drugs causes contact dermatitis? What do mydriatics do for the eye? Neo-synephrine is an example Decrease production of aqueous humor and thus decrease intraocular pressure. Diuresis Mydriatics Anticholinergics Miotics Dilate the pupil (My "D"riatic "D" for dilate) What do miotics do for the eye? Constrict the pupil Name one mydriatic Neo synephrine or Atropine What do anticholinergics do for the eye? Dilate the pupil Cycloplegia Paralyzes accommodation What is cycloplegia? Paralysis of the iris/pupil Which two of these classes of drugs cause tachycardia? What is the most common use for anticholinergics in the eye? How should eye ointments be given? Name two anticholinergics used in the eye. Name one carbonic anhydrase inhibitor How should the eye drops be given? How is the flow of eye irrigational fluid directed? Mydriatics Anticholinergics (sympathetic effects) To cause cycloplegia Dilation Allowing eye exam Placed on the lower inner eye lid, then have client close eyes Cyclogel, atropine Diamox Place drops into the lower conjunctival sac From inner canthus to outer canthus Name two miotics Pilocarpine, Timpotic (or any drug ending in -lol) Define nuclear family A family of parents and their offspring When does a nuclear family become an extended family? In America, the family is the basic unit of society. (T/F) Give the 2 major roles of the family in society What percentage of North American families are single-parent? 90% of single-parent families are headed by a . In what step of the nursing process does the nurse ask the family about their beliefs on illness? What is the first thing a nurse must do to help families in crisis? When aunts or uncles or grandparents live with the family True To protect and socialize 50% Female Assessment phase Nurse must first examine her own values Anxiety-producing thoughts are called . Repetitive actions designed to reduce anxiety are called . Which defense mechanism is most closely associated with obsessive-compulsive disorder? Should you allow an obsessive-compulsive person perform their compulsive behavior? Should you ever make an obsessive- compulsive person stop their compulsive behavior? Is the patient with obsessive-compulsive disorder neurotic or psychotic? Should you confront the obsessive-compulsive patient with the absurdity of their behavior? What should you do if an obsessive-compulsive patient is always late due to their rituals? What are the two types of oral contraceptives? How many days of the menstrual cycle do you take the progestin only pill? How many days of the menstrual cycle do you take the combination pill? How long before surgery must you discontinue oral contraceptives? If a women forgets to take pill one day, what should she do? Obsessions Compulsions -- such as washing hands over and over, dusting furniture 3 hours per day, refusing to turn your back to anyone Displacement Yes, give them time to do their ritual and try to set limit and redirect No, they will become very anxious Neurotic-- they know reality No, just say things like :You washed your hands for so long you must have been very anxious." Get them started earlier-- for example if they wash their hands for 1/2 hours before meals and are always late for breakfast, just get them started 1/2 hour earlier. Progestin only and combination progesterone and estrogen All 28 days You take it on days 5-24, but not on days 24-28 and 1-4 (8 days off) One week before surgery Take it as soon as she remembers it, and take next pill at regular time. What if a woman forgets to take the pill for two days in a row? What should she do? What should a woman do if she forgets to take her pill for 3 days or more? If a woman doesn't stop oral contraceptives one week before surgery she is at risk for developing . People who smoke more than cigarettes per day should not be on oral contraceptives. If a women on oral contraceptives misses a period, should she still take pills? Will breakthrough bleeding, nausea and vomiting and breast tenderness go away when a woman is on oral contraceptives? Osteoarthritis is a disease of the . Osteoarthritis is most commonly caused by the wear and tear of life. (T/F) The most common symptom of osteoarthritis is . What two joints are most commonly affected in osteoarthritis? To control the pain of osteoarthritis one should use heat or cold? What three medications are used in osteoarthritis? What do you observe on the fingers of the client osteoarthritis? Are Heberden's nodes painful? Take 2 pills a day for two days in a row and then resume normal schedule. Throw away pack and start new pack same day. use back-up contraceptive method for 7 days Thrombophlebitis 15, because if you smoke you have constriction of vessels and this potentates the chances that a woman on oral contraceptives will get thrombophlebitis Yes, however, if 2 missed periods occur,stop and have a pregnancy test. Yes, after about 3-6 months of treatment. Degenerative, joint True Joint pain knee and hip Heat Aspirin, non-steroidal inflammatory (NSAIDs) Indocen, Ibuprofen, steroids Heberden's nodes Not in the beginning, can be later as swelling occurs Are rest periods and range of motion exercises appropriate in the care of osteoarthritis? The pain of osteoarthritis is usually better or worse with rest? With activity? What age group gets osteoarthritis? Osteoarthritis is more common in females. (T/F) For cervical osteoarthritis the client should wear... Yes, rest is probably the most effective thing they can do. Better with rest, worse with activity 60-80 years old False, it occurs with equal frequency A cervical collar What is arthroplasty Joint replacement What is arthodesis? Joint fusion What is otosclerosis? Overgrowth of spongy bone in the middle ear that doesn't allow the bones of the middle ear to vibrate What will the client with otosclerosis complain of besides hearing loss? Do people have a loss of hearing with otosclerosis? What is corrective surgery for otosclerosis called? Should side rails be up after stapedectomy ? What should the client avoid post- stapedectomy? What warning should you give the client about getting up after stapedectomy? What should the client expect regarding hearing post- stapedectomy? What should the post- stapedectomy client do if he must sneeze? What type of hearing loss is associated with otosclerosis? Buzzing or ringing, in the ears (tinnitus) Yes Stapedectomy Yes, client may feel dizzy coughing sneezing blowing nose swimming showers flying Get up slowly An initial decrease with the benefits of surgery noticeable in 6 weeks Open his mouth, this de-pressurizes the middle ear. Conductive Which sex has a higher incidence of otosclerosis? Do hearing aids help in otosclerosis? What will be the results of the Rinne test in otosclerosis? Is stapedectomy done under general or local anesthesia? If the client complains of decreased hearing after stapedectomy what would you say? Which side will the client be allowed to lie upon post-stapedectomy? What two drugs are commonly give post- stapedectomy? Cysts on the ovaries are usually malignant. (T/F) What is the #1 reason why MD's remove ovrian cysts? Do small ovarian cysts cause symptoms? Common signs of large ovarian cysts are... What does torsion of an ovarian cyst mean? What is the big danger from torsion? What other disorders resemble rupture of ovarian cysts? What affect do oral contraceptives have on ovarian cysts? What are the three most common signs of ovarian cyst rupture? Compare signs of non- ruptured ovarian cysts with the sings of a ruptured ovarian cyst. (Give 3 for each) After surgery to remove an ovarian cyst the woman can return to normal activities between to weeks, Women Yes Bone conduction will be better than air conduction Local It is normal due to edema. The hearing will start to improve within six weeks. Depends on M: operative side promotes drainage, un-operative side prevents graft dislodgement. Don't make a big deal of position post-op Codeine/Demerol for pain, Dramamine for dizziness False, usually benign Remove before they transform into malignancy. No, only large ones Low back pain Pelvic pain Abnormal bleeding Twisting of cyst with interruption of its blood supply Necrosis and rupture of ovary Appendicitis, rupture of a fallopian tube pregnancy They cause it to stop growing and decrease in size. Pain, abdominal distention, abdominal rigidity Non-ruptured: low back pain, dull pelvic pain, abnormal uterine bleeding especially with menstruation Ruptured: acute pain, abdominal distention, and abdominal rigidity 4-6 weeks How soon after removal of an ovarian cyst can a woman resume sexual intercourse? Should a woman douche after surgery to remove an ovarian cyst? What does lightening mean? When does lightening occur in pregnancy? What is the most common positive effect of lightening? Name the two earliest signs that a woman is likely in labor. What is the most RELIABLE or VALID indication that a woman is in labor? What is the meaning of cervical effacement? Into how many stages is labor and delivery divided? What is accomplished during the first stage of labor and delivery? How long is the first stage of labor and delivery for a primagravida? For a multigravida? THe cervix is fully dilated when it is cm. The 2nd stage of labor and delivery accomplishes.... The 2nd stage of labor and delivery begins with and ends with of the . The 2nd stage of labor and delivery lasts hours for a primagravida and hours for a multigravida. The 3rd stage of labor and delivery accomplishes... 4-6 weeks No, it is not good to douche on a regular basis, it destroys natural protective vaginal flora When the fetal head descends into the pelvis 2-3 weeks before birth for primipara After it occurs the woman can breathe much easier Low back pain and show (blood-tinge mucous plug is passed) The onset of regular contractions that result in progressive dilation/effacement of the cervix The cervix thins 4 Full effacement and dilation 12 hours, 6 hours 10 Delivery of the infant Full dilation, delivery, infant 1 1/2 hours, 1/2 hour Expulsion of the placenta The 3rd stage of labor and delivery lasts... What occurs during the 4th stage of labor and delivery? When does the 4th stage of labor and delivery end? What is the average blood loss during labor? When the terminology "the three phases of labor" is used, what does it mean? Normal length of pregnancy is to days. Pregnancy is divided into trimesters. During the first trimester the woman experiences decreased or increased vaginal secretions? When are urine pregnancy tests positive? Pregnancy tests test for the presence of what hormone? Urine and blood pregnancy tests are enough evidence to be certain of pregnancy. (T/F) Less than one hour Recovery 2 hours after expulsion of the placenta 500 cc If the statement refers to phases of labor, it means the 3-step process of latency, followed by an active and transitional 240 to 300 3 Increased At the time of the first missed period HCG (human chorionic gonadotropin hormone) False, these tests only suggest pregnancy What is Hegar's sign? Uterine softening What is Chadwick's sign? The first trimester goes from week to week . The second trimester goes from week to week . Which week can mother first feel the fetus move? What is the word used to identify the feeling that the mother experiences when the fetus moves? The 3rd trimester goes from week to week . Blue-tint to the cervix 1, 13 14, 27 16th to 20th week (the end of the 4th month into the 5th month) Quickening 28, 40 In which trimester does the woman most feel backache? Which trimester is the fetus most susceptible to effects of outside agents? What is the name of the process in which outside agents cause birth defects in the fetus? Which trimester is nausea and vomiting most common? Which trimester do Braxton-Hicks contractions begin? In addition to the nares, where else should the nurse assess for skin irritation when nasal cannulae are in use? What are the two early signs of hypoxia? What is the highest flow rate appropriate for nasal cannulae? How often should the nares of a client with O2 by nasal cannulae be assessed for skin breakdown? What is the maximal O2 flow rate for the client with COPD? What are the signs of O2 toxicity? What can happen if the client with COPD is given a high flow rate of O2? What is the problem with giving high flow rates of O2 by nasal cannulae? Can a client smoke in the room when the O2 is turned off? When O2 is administered, it must be... Masks deliver higher or lower concentrations of O2 than nasal cannulae? Third First Teratogenesis First Third Behind and on top of the ears Restlessness, tachycardia 6 L/min Every 6-8 hours 2 L/min Confusion, headache They may stop breathing Dries the mucous membranes. No, the O2 delivery device must be removed from the wall or the tank out of the room before a client can smoke Humidified Higher How often should the nurse check the flow rate of the O2? At least once per shift O2 is an explosive (T/F) False, it does not explode-- it supports combustion What is the #1 difference between sealed & unsealed radiation? What are the 3 principles the nurse uses to protect self when caring for a client with a sealed radioactive implant? What is another name for external radiation therapy? What is the difference between external radiation treatment and internal radiation treatment? Of sealed internal, unsealed internal, and external radiation treatment, which is MOST dangerous for the nurse? Should pregnant nurses care for patient receiving sealed internal radiotherapy? Should pregnant nurses care for a patient receiving unsealed internal radiotherapy? What skin products should the patient receiving external radiotherapy AVOID? Describe the hygiene measures the you teach the patient receiving external radiotherapy? What are the major side effects of radiotherapy? Both are internal forms of radiotherapy however, in sealed, a solid object is placed in a body cavity; in unsealed a radioactive substance is injected in liquid form into a vein Time, distance, shielding Beam or X-rays In external the tumor is bombarded with x-rays & nothing is placed in the body; in internal there is some radioactive substance introduced into the body Sealed internal then unsealed internal, external radiation treatment is of no danger to the nurse unless the nurse is in the radiation treatment room during the treatment Never. (Lawsuit time!) Maybe, as long as they don't contact body secretions. No ointments with metals like zinc oxide, no talcum powder Use plain water only, no soaps, pat dry, can use cornstarch for itch Pruritis, erythema, burning, sloughing of skin, anorexia, nausea & vomiting, diarrhea, bone marrow depression When the patient is receiving radioactive iodine what precautions is/are most important? Rape is a crime of passion. (T/F) Most rapes occur involving two people of different races. (T/F) When must psychological care of the rape victim begin? Name the two phases of Rape Trauma Syndrome. Immediately after rape, a woman who is calm & composed is adjusting well. (T/F) Name the 3 physical symptoms of Rape Trauma Syndrome. Victims of rape often blame . In the long term reorganization phase the woman is likely to change . In the long term reorganization phase the woman is likely to experience during sleep. In the long term reorganization phase the woman has 4 common fears. Name them.... Before evident from the woman's body can be gathered for rape, must be completed. Should a female staff member be present when the rape victim is being examined? The rape victim requires only a pelvic exam & a head to toe exam is not done, so the client is not stressed. (T/F) Wear gloves while in possible contact with urine, special precautions taken to dispose of the urine. False, it is a violent act False, usually the same race In the emergency room Disorganization phase, re-organziation phase False, calmness & a composed attitude are SIGNS of Rape Trauma syndrome, (calm person is just as disorganized as the crying and upset lady) GI irritability, itching or burning on urination, skeletal muscle tension* don't forget PAIN Themselves Residence or/an telephone number Nightmares 1. Indoors or outdoors (depending on where the rape occured) 2. Being alone or in crowds 3. People being behind them 4. Sexual fears Consent forms Always False, the exam is a very long, invasive head-to-toe exam During exam the vaginal speculum is lubricated before it is placed in the vagina? (T/F) What drug is often used to prevent pregnancy after rape? When working with a rape victim they should be treated with and . After rape, a woman needs follow-up exam/test for False, lubrication could alter the evidence Kits approved by FDA: Preven (levornorgestrel & ethinly estradiol) or Plan B: Levonorgestrel (less N&V) Dignity & respect Sexually transmitted disease (STD's), i.e: AIDS, gonorrhea, syphilis... . After discharge contact with the rape victim is maintained via the . Raynaud's is an arterial or venous disease? What part of the body is most affected by Raynaud's? Raynaud's affects males or females mostly? What 3 things precipitate a Raynaud's attack? The digits in Raynaud's are hot or cold? What will the fingers look like? What will you find when you assess the legs of these patients? What 3 sensations will the client experience? What should the client with Raynaud's avoid? In the recovery room (PACU) the patient should be positioned.... What reflex is commonly routinely tested in the recovery room? When will the artificial airway be removed in the recovery room? Telephone Arterial disease characterized by spasms The fingers Women (young) Exposure to cold, emotional stress, tobacco use Cold Pale, sometimes blue Weak/absent pulses, cool, pale, loss of hair, shiny thin skin Pain, numbness, tingling Cold weather. (They should wear gloves & stop smoking) On either side Gag reflex When the gag reflex returns Vital signs are measured in the recovery room. In the recovery room the head should be .... In the recovery room the neck should be ... Can post-operative pain medications be given in the recovery room? Give 3 stages of acute renal failure. Every 15 minutes To the side with the cheek & neck extended slightly down Slightly extended Yes Oliguric, diuretic, recovery Define renal failure. Inability of the kidney to excrete wastes & maintain fluid & electrolyte balance What is the BIG danger in renal failure? Hyperkalemia and it's effect on the heart What is anuria? Less than 50 cc of urine in 24 hours What is oliguria? Less than 500 cc of urine in 24 hours What are the dietary modifications for the recovery phase of acute renal failure? What are the dietary modifications for the diuretic phase of acute renal failure? What are the dietary modifications for the oliguric phase of acute renal failure? What causes the itching seen in renal failure? What is the first phase in acute renal failure? In the oliguric phase, blood volume is , sodium is , and potassium is . How long does the oliguric phase last? In the diuretic phase, blood volume is , sodium is , and potassium is . How long does the diuretic phase last? Increased carbohydrates, increased protein. Increased carbohydrates, increased protein. Moderate potassium & sodium. (May need to increase fluids in diuresis results in dehydration.) Increased carbohydrates, decreased protein, decreased sodium, decreased potassium, decreased water. Accumulation of wasted in the blood and the associated signs. This occurs in the end stage renal failure. The oliguric phase High, high, high 7-10 days Low, low, low 3-4 days, maximum time 2-3 weels In the diuretic phase: urine output can= to liters/24 hours. Which is more dangerous, oliguria or anuria? Why? Respiratory Distress Syndrome occurs in full- term infants. (T/F) Respiratory Distress Syndrome hardly ever occurs after week of gestation. Respiratory Distress Syndrome is also know as .... The cause of RDS is a lack of . Surfactant surface tension inside . Surfactant prevents the of the alveoli. Lack of surfactant causes the neonate to lose lung capacity with each . Death from Respiratory Distress Syndrome most commonly occurs within hours of birth. Within in minutes of birth, what 3 respiratory difficulties occur? What medication is given? By what route? What acid/base disorder is seen in Respiratory Distress Syndrome? What will you auscultate over the lungs of the neonate with Respiratory Distress Syndrome? What lab test assesses the risk of Respiratory Distress Syndrome? 4-5 liters per 24 hours Oliguria, because since you are losing more fluids you are actually hemo- concentrating the hyperkalemia more False, it occurs in premature infants 37 Hyaline Membrane Disease (HMD) Surfactant Decreases, alveoli Collapse Breath 96 Retractions, nasal flaring, and grunting Survanta (Surfactant) via ET tube. Repeat doses are often required. Respiratory acidosis (CO2 is retained) Decreased lung sounds with crackles L/S ratio (Lecithin/Sphingomyelin ratio) What L/S ratio indicated fetal lung maturity? What other test is used to confirm fetal lung maturity? Severe cases of Respiratory Distress Syndrome requires ventilation with . What may be added to the IV to correct the acidosis? High flow rates of O2 delivered in Respiratory Distress Syndrome can cause 2/1 Amniotic fluid is analyzed for presence of PG PEEP (Positive end expiratory pressure) & CPAP. (Continuous positive airway pressure), to keep alveoli open while on the ventilator. High frequency jet ventilation is sometimes used. Bicarbonate Retrolental fibroplasia (an eye problem) . Retrolental fibroplasia can result in . High ventilatory pressures result in what chronic lung problem? At what time of year does rheumatoid arthritis flare up? As with any inflammatory disease clients with rheumatoid arthritis have a low- . What factor is present in the blood when the client has rheumatoid arthritis? Blindness from retinal damage Bronch-pulmonary dyplasia Spring grade fever The rheumatoid factor [Show More]
Last updated: 1 year ago
Preview 1 out of pages
Reviews( 0 )
Document information
Connected school, study & course
About the document
Uploaded On
Oct 19, 2020
Number of pages
Written in
Additional information
This document has been written for:
Uploaded
Oct 19, 2020
Downloads
0
Views
4
















 NCLEX Study Guide.png)
 NCLEX Study Guide Flashcards _ Quizlet-compressed.png)
 NCLEX Study Guide (2000 Q&A-100% CORRECT) A+ UPDATED 2022.png)