Health Care > SOAP NOTE > NURS 621 SOAP note Subjective Objective Assessment , Plan (Burning with urination as well as increas (All)
NURS 621 SOAP note Subjective Objective Assessment , Plan (Burning with urination as well as increased urinary frequency for 24 hours)
Document Content and Description Below
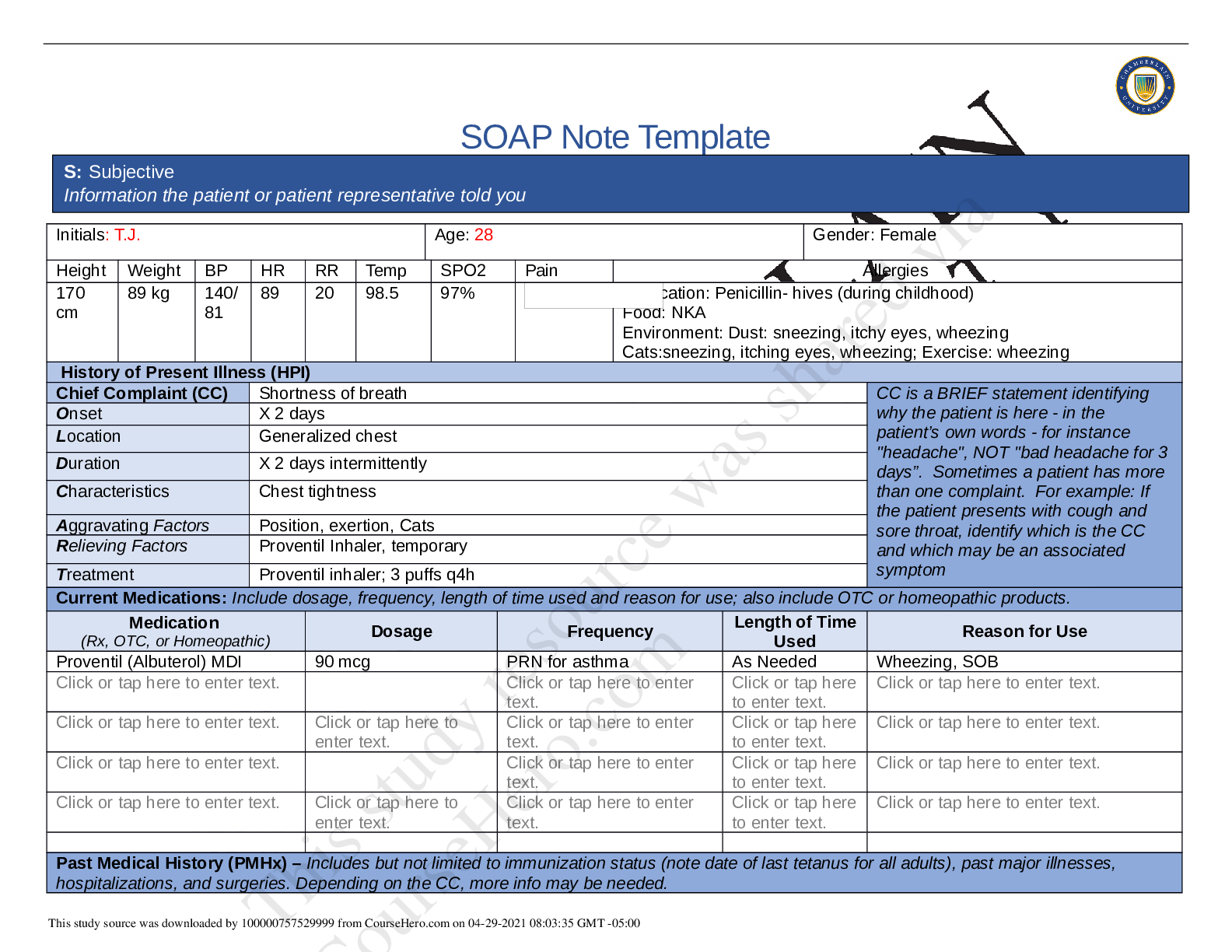
S.O.A.P. Note Template Case ID#: Assignment 10.1 Subjective Objective Assessment (diagnosis [primary and differential diagnosis]) Plan (treatment, education, and follow up plan) Basic Informatio... n Female 36 years old Subjective History Chief Complaint Chief complaint of burning with urination as well as increased urinary frequency for 24 hours. History of Present Illness This is a pleasant 36 your old Caucasian female who presents to the clinic with a chief complaint of dysuria and increased urinary frequency for approximately 24 hours. She was in her usual state of health until yester [Show More]
Last updated: 1 year ago
Preview 1 out of 5 pages
Instant download

Buy this document to get the full access instantly
Instant Download Access after purchase
Add to cartInstant download
Reviews( 0 )
Document information
Connected school, study & course
About the document
Uploaded On
Oct 06, 2022
Number of pages
5
Written in
Additional information
This document has been written for:
Uploaded
Oct 06, 2022
Downloads
0
Views
58