*NURSING > SOAP NOTE > Monroe College NURSING 812 Adult Assessment Soap Note: Follow up BP visit Patient initials and ag (All)
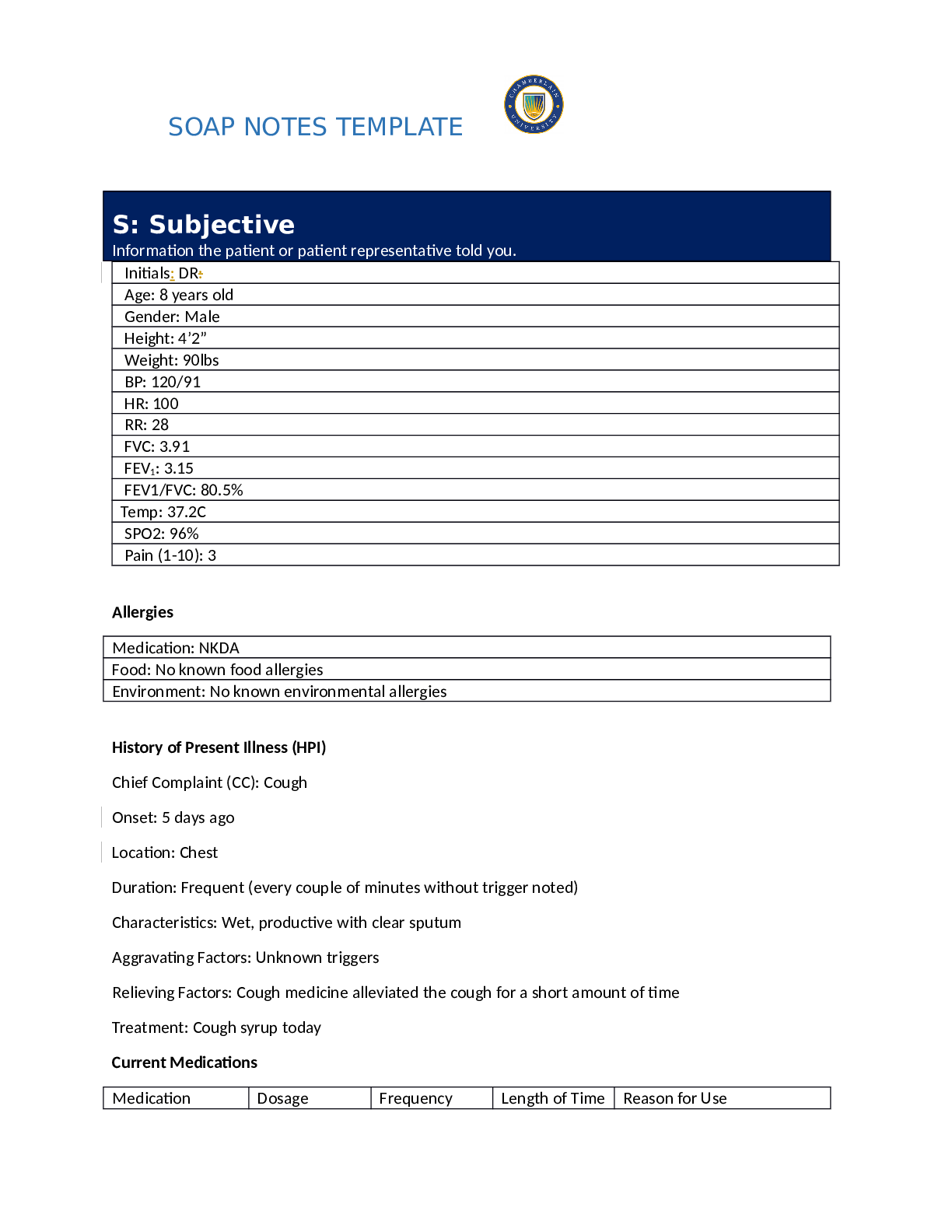
Monroe College NURSING 812 Adult Assessment Soap Note: Follow up BP visit Patient initials and age: MD, 47 Subjective Data: Chief complaint: Patient states he is, “following up on my high blood pressure.”
Document Content and Description Below
Monroe College NURSING 812 Adult Assessment Soap Note: Follow up BP visit Patient initials and age: MD, 47 Subjective Data: Chief complaint: Patient states he is, “following up on my high bloo... d pressure.” History of present illness: Mr. D is following up from a visit 3 months ago in which he was noted to have possible hypertension. Today’s blood pressure is 140/92, which is an improvement from previous visit with a blood pressure of 154/100. Patient is a marathon runner. He states he exercises daily by running 6+ miles a day. He denies any current stressors in his life. He also denies any chest pain or palpitations. He states he cannot tell when his blood pressure is high. He does not check his blood pressure at home. He does have a familial history of hypertension of both the mother and father. He states he “tries to eat well,” but does enjoy salty foods. He also states he used to drink many energy drinks and now has tried to cut back on those. He has never taken any medication for hypertension. He also denies taking routine NSAIDs or OTC cold or sinus medications. Past medical history: None Family history: 1. Father: living, hypertension, hyperlipidemia, arthritis, cardiac stents 2. Mother: living, hypertension, hyperlipidemia, hypothyroidism 3. Younger sister: living, no known medical history Social history: 1. Denies any tobacco use 2. Reports occasional social alcohol use 3. Denies any elicit drug use 4. Enjoys running and participating in marathons 5. Denies currently being sexually active 6. Played basketball in college Medications: 1. Multivitamin OTC, 1 P.O. daily 2. Fish oil OTC, 1 gram, P.O. daily Immunizations: 1. Influenza: October 2016 2. Tetanus: patient cannot recall date, states has been within past 10 years. 3. Patient cannot recall any other previous immunizations Allergies: No known drug allergies. Review of systems: ROS General: denies any fever, chills, sweats, or fatigue. Does report a 20+ pound weight loss over past year. Patient relates this to increased exercise over the past year. HEENT: denies any headaches, dizziness, changes in vision, blurry vision, ear pain, hearing difficulties, nasal drainage, changes or difficulty with smell, sore throat, changes in taste, or dental complaints. Patient states he annually sees ophthalmologist. Cardiovascular: denies any chest pain, SOB, palpitations, edema, claudication, or ever seeing a cardiologist. Reports family history hypertension, hyperlipidemia, and cardiac stents. Only cardiac testing he has had was his last office visit with EKG. Respiratory: denies any difficulty breathing, SOB, cough, sputum, wheezing, does not recall last chest x-ray, and states all previous PPDs have been negative. GI/GU: denies any reflux, nausea, vomiting, abdominal pain, diarrhea, constipation, changes in bowel habits, blood in stool, or gall stones. Patient has never had colonoscopy. Denies any changes in urinary habits, changes in urine flow or color, problems starting or stopping stream, testicular pain, and history of STIs, UTIs, or kidney stones. [Show More]
Last updated: 1 year ago
Preview 1 out of 3 pages

Reviews( 0 )
Document information
Connected school, study & course
About the document
Uploaded On
Nov 07, 2022
Number of pages
3
Written in
Additional information
This document has been written for:
Uploaded
Nov 07, 2022
Downloads
0
Views
44


















.png)