*NURSING > SOAP NOTE > Chamberlain College of Nursing NR 590 SOAP Note Week 1| Complete Physical Assessment (All)
Chamberlain College of Nursing NR 590 SOAP Note Week 1| Complete Physical Assessment
Document Content and Description Below
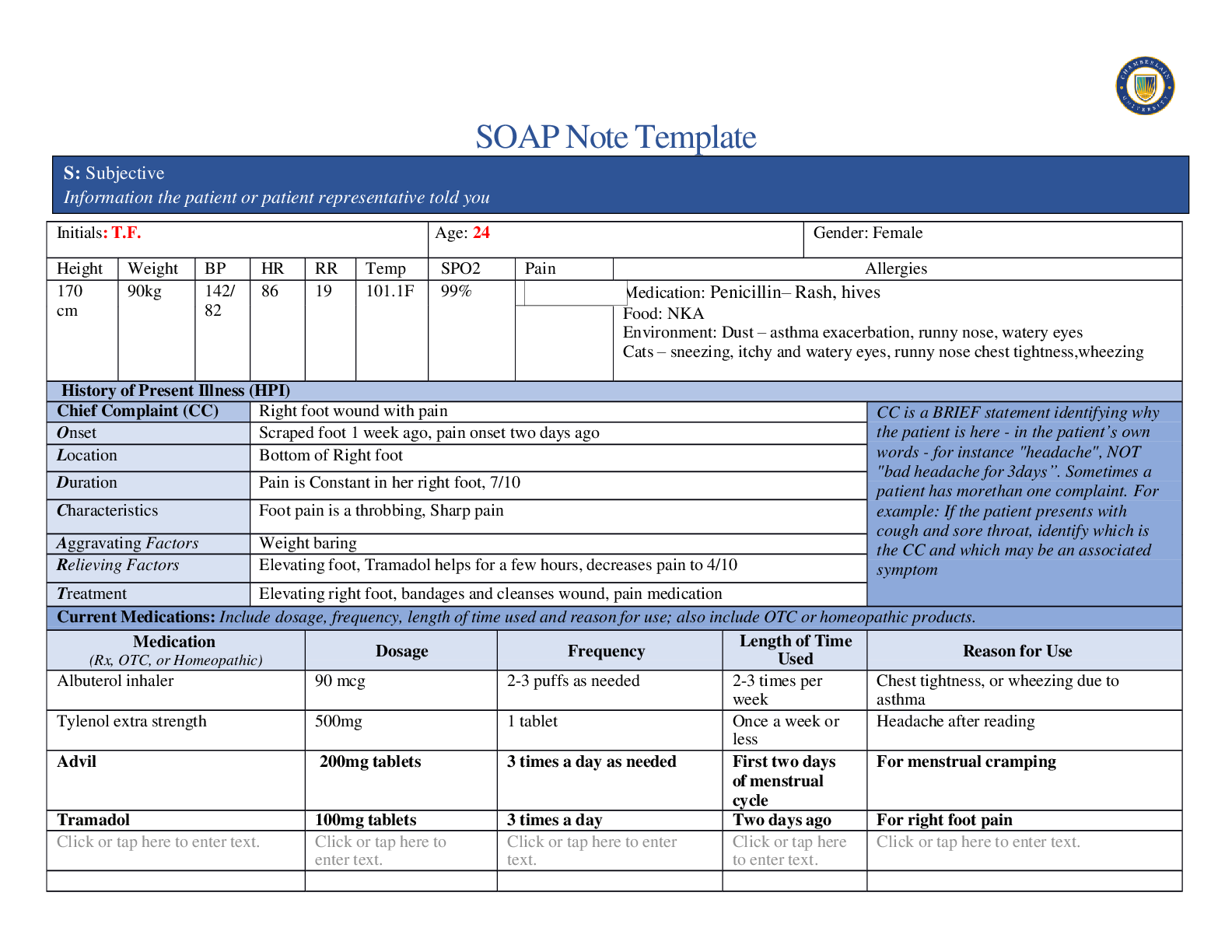
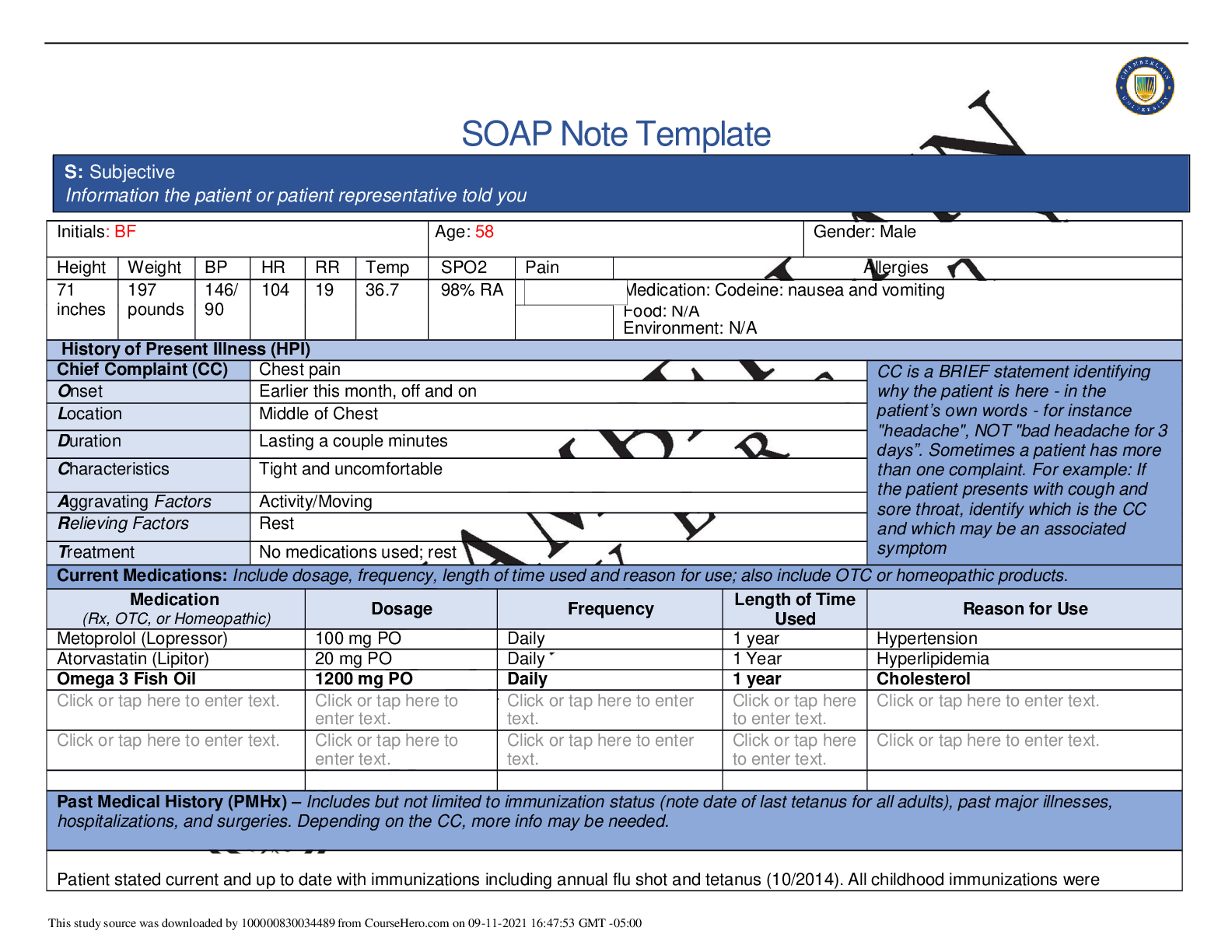
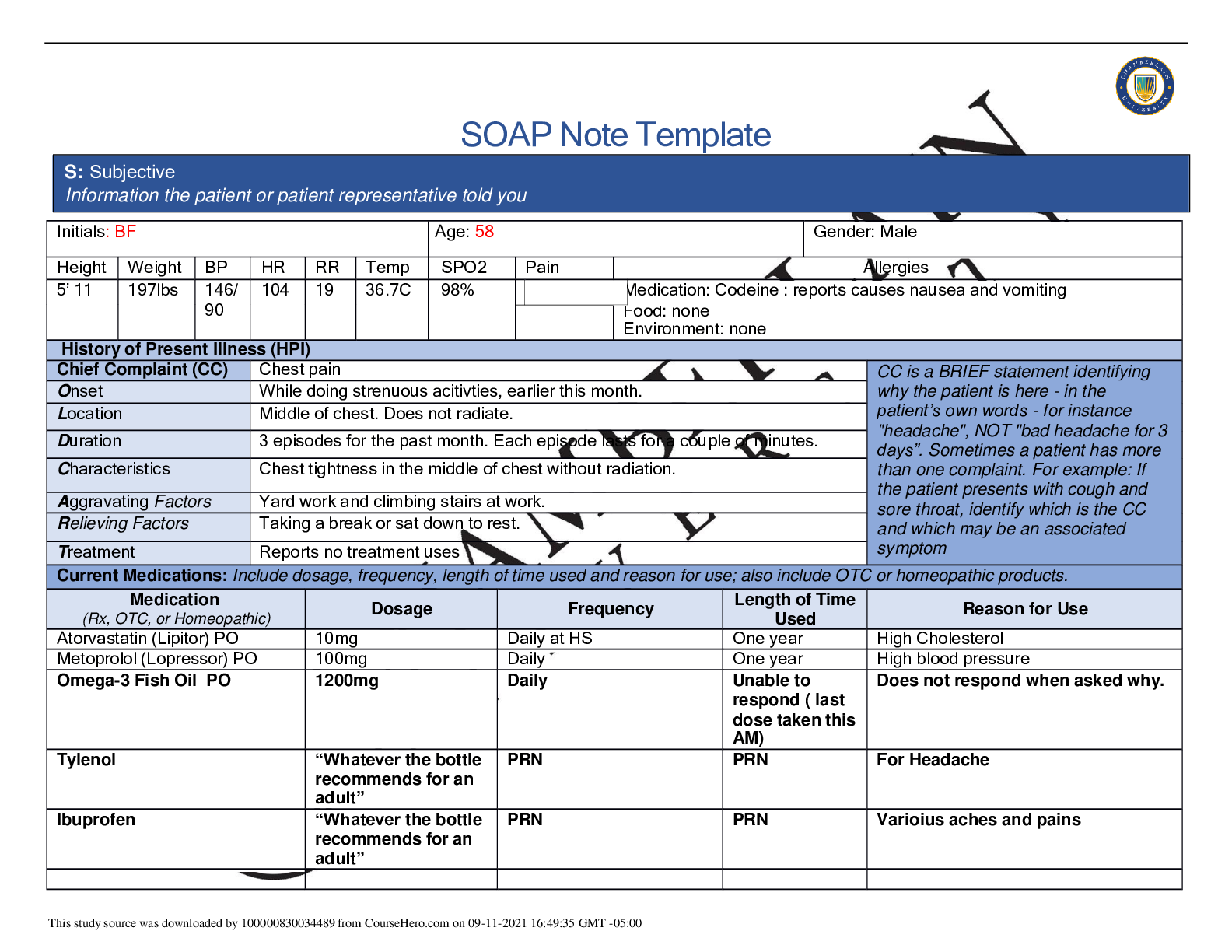
SOAP Note Template Initials: T.F. Age: 24 Gender: Female Height Weight BP HR RR Temp SPO2 Pain Allergies 170 cm 90kg 142/ 82 86 19 101.1F 99% Medication: Penicillin– Rash, hives ... Food: NKA Environment: Dust – asthma exacerbation, runny nose, watery eyes Cats – sneezing, itchy and watery eyes, runny nose chest tightness, wheezing History of Present Illness (HPI) Chief Complaint (CC) Right foot wound with pain CC is a BRIEF statement identifying why the patient is here - in the patient’s own words - for instance "headache", NOT "bad headache for 3 days”. Sometimes a patient has more than one complaint. For example: If the patient presents with cough and sore throat, identify which is the CC and which may be an associated symptom Onset Scraped foot 1 week ago, pain onset two days ago Location Bottom of Right foot Duration Pain is Constant in her right foot, 7/10 Characteristics Foot pain is a throbbing, Sharp pain Aggravating Factors Weight baring Relieving Factors Elevating foot, Tramadol helps for a few hours, decreases pain to 4/10 Treatment Elevating right foot, bandages and cleanses wound, pain medication Current Medications: Include dosage, frequency, length of time used and reason for use; also include OTC or homeopathic products. [Show More]
Last updated: 1 year ago
Preview 1 out of 12 pages

Reviews( 0 )
Document information
Connected school, study & course
About the document
Uploaded On
May 25, 2021
Number of pages
12
Written in
Additional information
This document has been written for:
Uploaded
May 25, 2021
Downloads
0
Views
47














.png)
.png)
.png)
.png)
.png)






.png)






