*NURSING > STUDY GUIDE > NUR 265 Exam 2 Study Guide. Latest 2020/21 (All)
NUR 265 Exam 2 Study Guide. Latest 2020/21
Document Content and Description Below
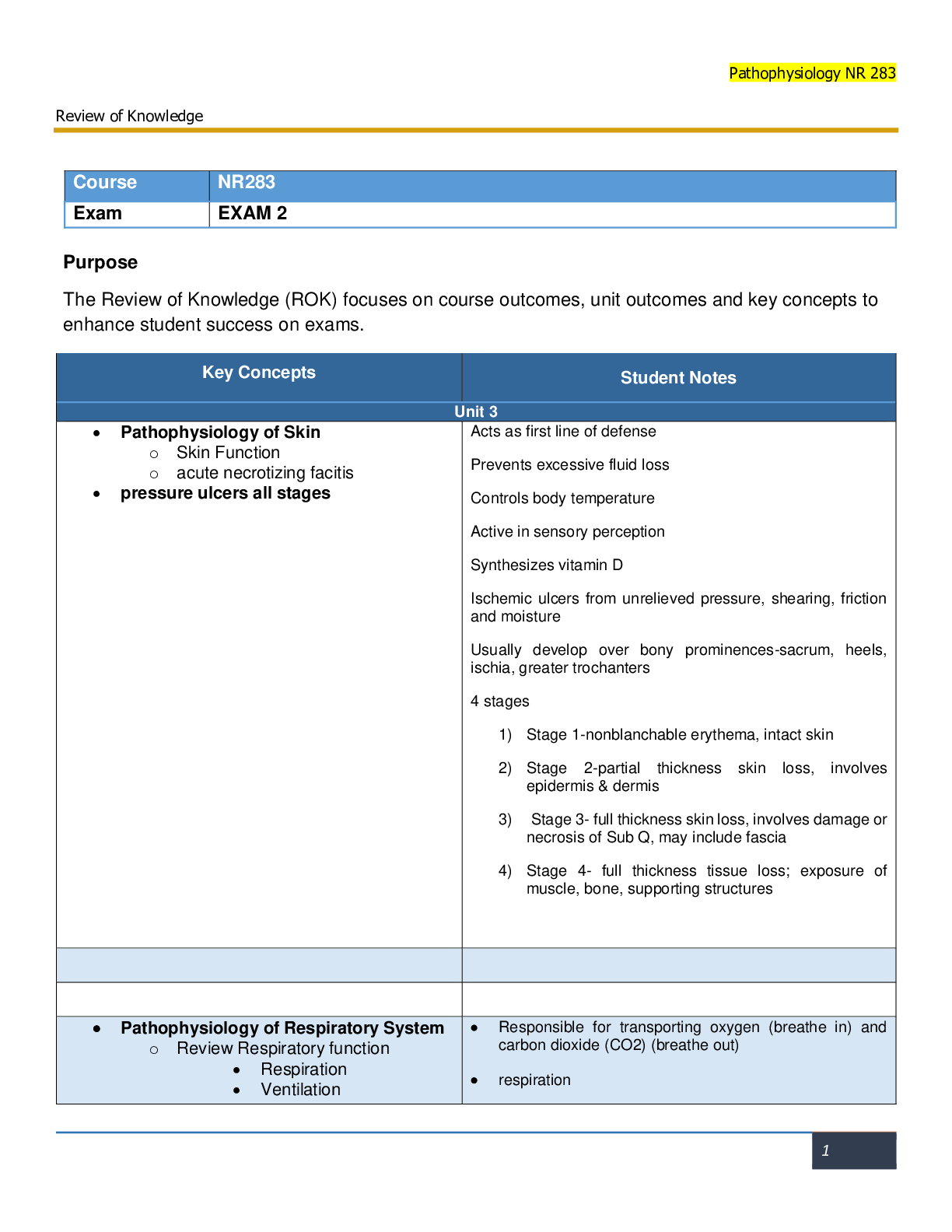
NUR 265 Exam 2 Study Guide. Latest 2020/21.Lungs Physiology • 2 Pleural, 1 attached to outside of lungs and 1 attached to inside of ribs. • Space between the 2 pleural is negative to atmosphere ... • When inhale becomes more positive and atmosphere more negative. Exhaling is passive • Most of lower lobes are posterior, must listen to lungs posteriorly • Breath sounds o Bronchial: High pitched & loud, normal in tracheal & larynx o Bronchovesicular: Moderate pitched & amplitude, normal over major bronchi o Vesicular: Low pitched & soft, like wind through trees, normal in lower lung fields where smaller bronchioles & alveoli are. Pulmonary Emboli (P 603) • Occlusion of portion of pulmonary artery by a blood clot – from venous circulation – lower extremities or heart. • Causes ventilation-perfusion mismatch (V/Q) – Ventilated alveoli no longer perfused due to clotted artery. • Risk Factors o Venous stasis (w/prolonged immobility); Central venous catheters; Surgery (NPO, dehydrated, immobilized pts); Obesity; Advanced age; Hypercoagulability (Platelets >400K and not enough fluids; sticky blood); Hx of thromboembolism. o Greatest r/f in the young is the combo of smoking and hormone based contraceptives. • Nursing Assessment Findings o Respiratory Classic Manifestations (Hypoxia drives all s/s) Dyspnea (sudden onset); Chest pain (sharp & stabbing); Apprehension, restlessness; Feeling of impending doom; Cough; Hemoptysis (blood in sputum). o Respiratory Signs Pleural friction rub (scratching sounds from pleura rubbing together & pain on deep inspiration); Tachypnea; Crackles (or normal); S3 or S4; Diaphoresis; Low grade fever; Petechiae over chest and axillae; Decreased arterial oxygen saturation (SaO2) o Many pts w/ a PE do not have “classic” sx (i.e. hypoxia), but instead have vague sx resembling the flu (n/v & general malaise) o Cardiac Manifestations Decreased tissue perfusion: tachycardia, JVD, Syncope (loss of consciousness), Cyanosis, & Hypotension. o In patients with r/f for PE, JVD (RSHF), syncope (decreased blood flow to brain), cyanosis (severe hypoxia) and hypotension together, NEED RAPID RESPONSE TEAM CALLED. HAVE HELP ON WAY B4 O2 APPLIED o When pt has sudden onset of dyspnea, chest pain, and/or hypotension, immediately notify Rapid Response Team. Reassure pt. and elevate HOB. Prepare for O2 therapy and ABG analysis o Saddle Emboli – Embolism at split of pulmonary artery that blocks both branches to the lungs • Medical Dx o Chest X-ray – May show PE if large but will help r/o other things o CT scan – Most often used to dx PE o TEE (Transesophageal Echocardiography) – See if there are clots in the atria o Ventilation Perfusion scan (V/Q) Considered if pt is allergic to contrast dye done w/CT scan Radioactive substance to see if air is getting into the alveoli; injected into blood to look at clot and can also detect pneumothorax. Done 2x o ABGs Respiratory Alkalosis FIRST from hyperventilation THEN Respiratory Acidosis from shunting • Shunting of blood from the right side of the heart to the left side w/o picking up O2 from lungs – causes PaCO2 level to rise resulting in respiratory acidosis. LATER Metabolic Acidosis & lactic acid buildup from tissue hypoxia Even if ABGs & Pulse Ox shows hypoxemia it is not enough to dx PE alone as PE is not the only cause of hypoxemia. • Medical Management o GIVE O2, IV FLUIDS, INOTROPES (DOBUTAMINE/MILRINONE) Oxygen therapy to maintain O2 sat at 95% or patient baseline Hypotension - Tx w/ IV fluids (isotonic) & Inotropes (Dobutamine/Milrinone, make heart contract more forcefully); vasopressors (norepi, epi, dopamine) when hypotension persists after fluids. o Anticoagulation w/ Heparin drip – Goal is PTT 1.5-2.5 x normal (60-70 sec) = 90-175 sec Minimize growth of existing clots and prevent new ones Antidote Protamine Sulfate Do not use w/salicylates (Aspirin) o Convert to Warfarin when stable – On 3rd day of Heparin use, overlap – INR target 2-3 (0.9-1.2 normal) Antidote – Vit K – phytonadione (Mephyton) Teach pts to avoid foods high in K (leafy dark green vegis, herbs, spring onions, Brussel sprouts, broccoli, cabbage, asparagus, potatoes, & winter squash). o Enoxaparin or dalteparin o Fibrinolytic (tPA) to tx massive PE or hemodynamic instability Antidotes – clotting factors, FFP, & aminocaproic acid (Amicar) Dissolve the clot itself o Embolectomy – surgical removal of the embolus – When tPA can’t be used or for massive PE w/shock o Inferior Vena Cava Filter – to prevent [Show More]
Last updated: 1 year ago
Preview 1 out of 35 pages
Instant download

Buy this document to get the full access instantly
Instant Download Access after purchase
Add to cartInstant download
Reviews( 0 )
Document information
Connected school, study & course
About the document
Uploaded On
Feb 21, 2021
Number of pages
35
Written in
Additional information
This document has been written for:
Uploaded
Feb 21, 2021
Downloads
0
Views
39