Biology > QUESTIONS and ANSWERS > 566 Midterm Study Guide (All)
566 Midterm Study Guide
Document Content and Description Below
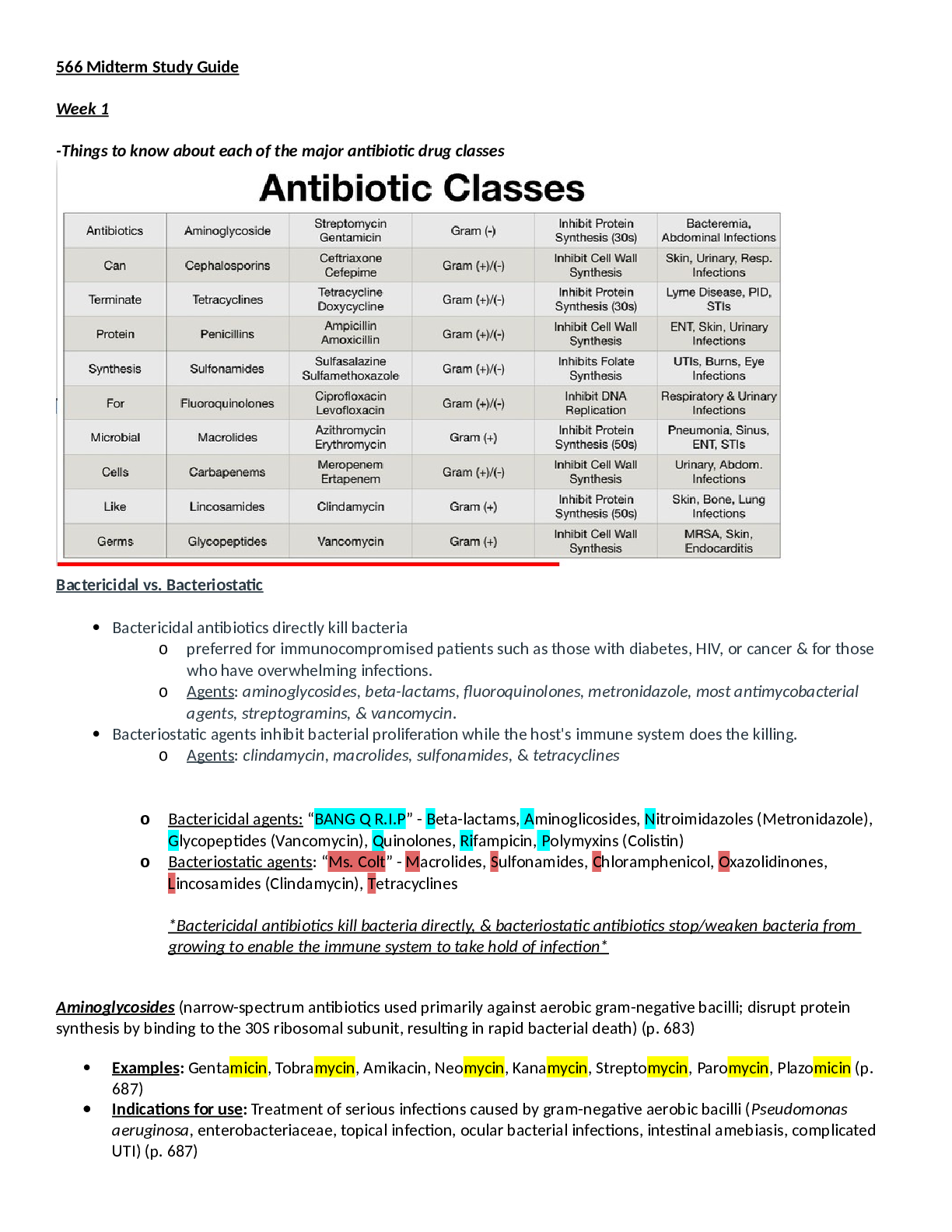
-Things to know about each of the major antibiotic drug classes Bactericidal vs. Bacteriostatic Bactericidal antibiotics directly kill bacteria o preferred for immunocompromised patients such a... s those with diabetes, HIV, or cancer & for those who have overwhelming infections. o Agents: aminoglycosides, beta-lactams, fluoroquinolones, metronidazole, most antimycobacterial agents, streptogramins, & vancomycin. Bacteriostatic agents inhibit bacterial proliferation while the host's immune system does the killing. o Agents: clindamycin, macrolides, sulfonamides, & tetracyclines o Bactericidal agents: “BANG Q R.I.P” - Beta-lactams, Aminoglicosides, Nitroimidazoles (Metronidazole), Glycopeptides (Vancomycin), Quinolones, Rifampicin, Polymyxins (Colistin) o Bacteriostatic agents: “Ms. Colt” - Macrolides, Sulfonamides, Chloramphenicol, Oxazolidinones, Lincosamides (Clindamycin), Tetracyclines *Bactericidal antibiotics kill bacteria directly, & bacteriostatic antibiotics stop/weaken bacteria from growing to enable the immune system to take hold of infection* Aminoglycosides (narrow-spectrum antibiotics used primarily against aerobic gram-negative bacilli; disrupt protein synthesis by binding to the 30S ribosomal subunit, resulting in rapid bacterial death) (p. 683) Examples: Gentamicin, Tobramycin, Amikacin, Neomycin, Kanamycin, Streptomycin, Paromycin, Plazomicin (p. 687) Indications for use: Treatment of serious infections caused by gram-negative aerobic bacilli (Pseudomonas aeruginosa, enterobacteriaceae, topical infection, ocular bacterial infections, intestinal amebiasis, complicated UTI) (p. 687) Contraindications & high-risk patients: Aminoglycosides should be used with caution in patients with renal impairment, preexisting hearing impairment, & those receiving ototoxic & nephrotoxic drugs. (pp. 685-687) Monitoring needs: Aminoglycoside levels (peaks & troughs) & renal function must be monitored. Monitor for neurotoxicity, ototoxicity, & nephrotoxicity. Which ones require renal dosing adjustments and how much (i.e., 25%, 50%, etc.): To avoid serious toxicity, we must reduce dosage size or increase the dosing interval in patients with kidney disease. (p. 685) *Clarithromycin Patient education: *Patients should be informed about the symptoms of vestibular & cochlear damage & instructed to report them. Lifespan considerations: (p. 685) Infants: Aminoglycosides are approved to treat bacterial infections in infants younger than 8 days. Dosing is based on weight & length of gestation. Children/adolescents: Aminoglycosides are safe for use against bacterial infections in children & adolescents. Pregnant women: There is evidence that use of aminoglycosides in pregnancy can harm the fetus. Breastfeeding women: Gentamicin is probably safe to use during lactation. There is limited information regarding its use in this way. Older adults: Caution must be used regarding decreased renal function in the older adult. Cephalosporins (Beta-lactam antibiotics similar in structure & actions to the penicillins; bactericidal; often resistant to beta-lactamases, & active against a broad spectrum of pathogens; most widely used group of antibiotics) (p. 669) Examples: 1 st generation: Cephalexin (Keflex); 2 nd generation: Cefoxitin, Cefaclor (Ceclor); 3 rd generation: Cefotaxime, Cefdinir, Ceftriaxone (Rocephin); 4 th generation: Cefepime, 5 th generation: Ceftaroline Indications for use: 1 st generation: Staphylococci or streptococci (Use in patients with mild PCN allergy, strep pharyngitis, skin infections, & surgical prophylaxis) 2 nd generation: Haemophilus influenzae, Klebsiella, pneumococci, & staphylococci (Otitis, sinusitis, & respiratory tract infections) 3 rd generation: Pseudomonas aeruginosa, Neisseria gonorrhoeae, & Klebsiella, Serratia (Meningitis, gramnegative nosocomial infections) 4 th generation: Pseudomonas aeruginosa (Hospital-acquired pneumonia & complicated intra-abdominal & UTIs due to resistant pseudomonas) 5 th generation: Methicillin-resistant Staphylococcus aureus (MRSA-associated infections). (p. 671) Contraindications & high-risk patients: Cephalosporins are contraindicated for patients with a history of allergic reactions to cephalosporins or severe reactions to penicillin. Patients using cefazolin & cefotetan must not consume alcohol. Use cefotetan, cefazolin, & ceftriaxone cautiously in patients taking other agents that also promote bleeding (anticoagulants, thrombolytics, NSAIDS, etc). (pp. 670-671) Monitoring needs: Monitor for signs of C. dif infection & renal function in patients with renal impairment and/or prolonged use. Which ones require renal dosing adjustments and how much (i.e., 25%, 50%, etc.): In patients with renal insufficiency, dosages of most cephalosporins must be reduced to prevent accumulation to toxic levels. (EXCEPTION: Ceftriaxone (3 rd generation) is eliminated largely by the liver, so dosage reduction is unnecessary in patients with renal impairment) (p. 669) Patient education: *All cephalosporins can promote C. dif infection, so patients should be instructed to report an increase in stool frequency. Lifespan considerations: Infants: 3 rd generation cephalosporins are used to treat bacterial infections in neonates as well as infants. Children/adolescents: Cephalosporins are commonly used to treat bacterial infections in children, including otitis media & gonococcal & pneumococcal infections. Pregnant women: All cephalosporins appear safe for use in pregnancy. Breastfeeding women: Cephalosporins are generally not expected to cause adverse effects in breastfed infants. Older adults: Doses should be adjusted in older adults with decreased renal function. Tetracyclines (broad-spectrum antibiotics active against a wide variety of gram-positive & gram-negative bacteria; suppress bacterial growth by binding to the 30S ribosomal subunit & inhibiting protein synthesis, extensive use has resulted in increasing bacterial resistance—because of this & the availability of other antibiotics with greater selectivity & less toxicity, their use has declined & they are rarely drugs of 1st choice) (p. 676) Examples: Tetracycline, Demeclocycline, Doxycycline, Eravacycline, Minocycline, Omadacycline, Sarecycline Indications for use: Treatment of tetracycline-sensitive infections, acne, & periodontal disease. 1st line drugs for rickettsial diseases (Rocky Mountain spotted fever, typhus fever, Q fever); infections caused by Chlamydia trachomatis (trachoma, lymphogranuloma venereum, urethritis, cervicitis); brucellosis; cholera; pneumonia caused by Mycoplasma pneumoniae; Lyme disease; anthrax; & gastric infection with H. pylori. Contraindications & high-risk patients: Contraindicated in pregnant women & in children younger than 8 years. Monitoring needs: None recommended. Which ones require renal dosing adjustments and how much (i.e., 25%, 50%, etc.): Tetracyclines may exacerbate renal impairment in patients with preexisting kidney disease. Because tetracycline & demeclocycline are eliminated by the kidneys, these agents should not be given to patients with renal impairment. If a patient with renal impairment requires a tetracycline, either doxycycline or minocycline should be used because these drugs are eliminated primarily by the liver. (p. 677) Patient education: *Should not be taken with calcium supplements, milk products, iron supplements, magnesium-containing laxatives, or most antacids because they can decrease tetracycline absorption. *GI distress can be reduced by taking tetracycline with meals. *Advise patients to avoid prolonged exposure to sunlight, wear protective clothing, & apply a sunscreen to exposed skin. *Patients should notify provider if significant diarrhea occurs so that the possibility of bacterial superinfection can be evaluated. (pp. 676-678) Lifespan considerations: (p. 678) Children/adolescents: Tetracyclines should not be used in children younger than 8 years because they may cause permanent discoloration of the teeth. Pregnant women: Animal studies reveal that tetracyclines can cause fetal harm in pregnancy. Thus, this class of drugs should be avoided in pregnant women. Breastfeeding women: Use of tetracyclines during tooth development can cause permanent staining. Tetracyclines should be avoided by breastfeeding women. Older adults: Tetracyclines can interact with drugs, including digoxin. In the older adult who takes many medications, check for interactions. [Show More]
Last updated: 1 year ago
Preview 1 out of 34 pages
Instant download
Buy this document to get the full access instantly
Instant Download Access after purchase
Add to cartInstant download
Reviews( 0 )
Document information
Connected school, study & course
About the document
Uploaded On
May 03, 2022
Number of pages
34
Written in
Additional information
This document has been written for:
Uploaded
May 03, 2022
Downloads
0
Views
49









.png)










 – Chamberlain College of Nursing.png)
 – Chamberlain College of Nursing.png)

