*NURSING > STUDY GUIDE > NR 602 Primary Care Of The Childbearing Family Practicum. Midterm Study Guide (All)
NR 602 Primary Care Of The Childbearing Family Practicum. Midterm Study Guide
Document Content and Description Below
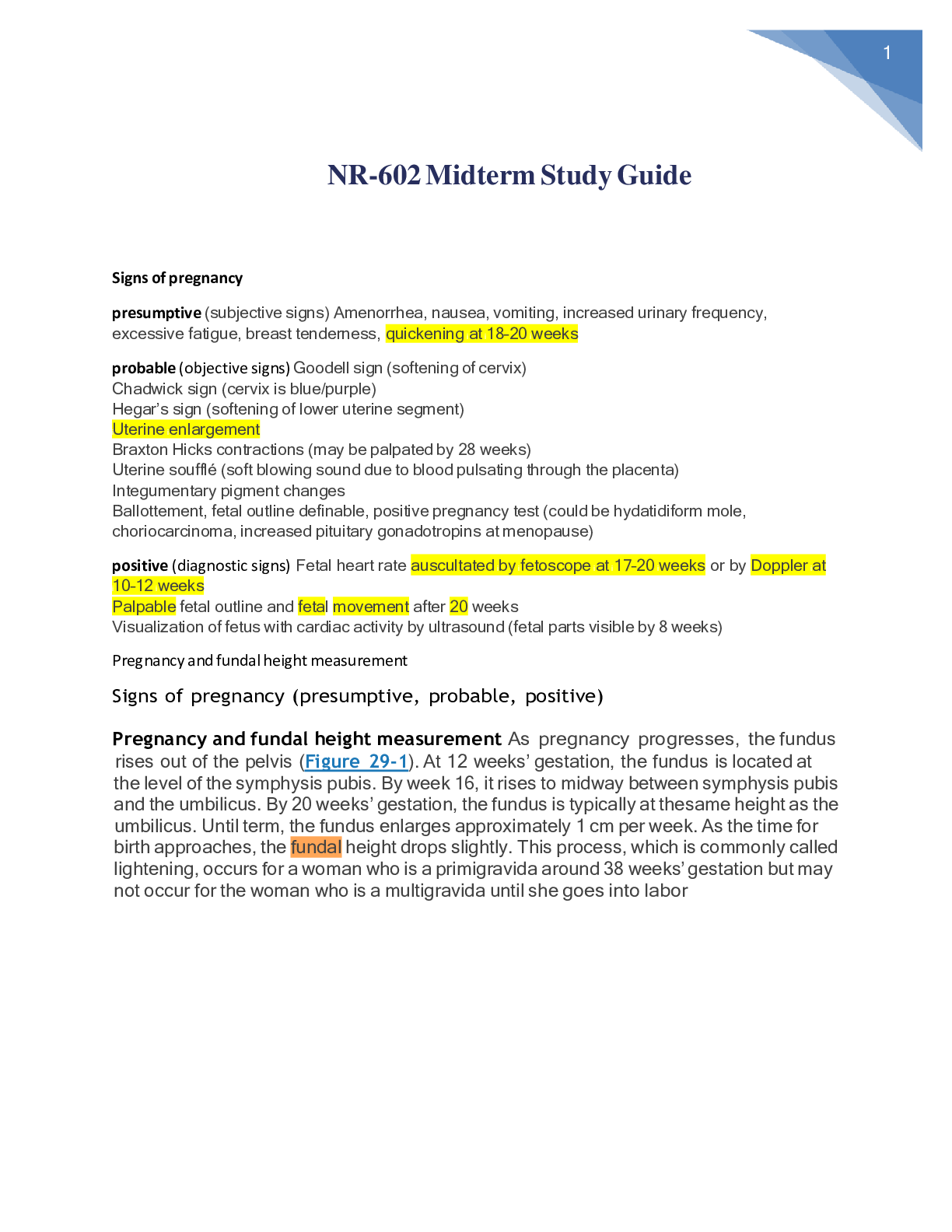
Signs of pregnancy presumptive (subjective signs) Amenorrhea, nausea, vomiting, increased urinary frequency, excessive fatigue, breast tenderness, quickening at 18–20 weeks probable (objective si... gns) Goodell sign (softening of cervix) Chadwick sign (cervix is blue/purple) Hegar’s sign (softening of lower uterine segment) Uterine enlargement Braxton Hicks contractions (may be palpated by 28 weeks) Uterine soufflé (soft blowing sound due to blood pulsating through the placenta) Integumentary pigment changes Ballottement, fetal outline definable, positive pregnancy test (could be hydatidiform mole, choriocarcinoma, increased pituitary gonadotropins at menopause) positive (diagnostic signs) Fetal heart rate auscultated by fetoscope at 17–20 weeks or by Doppler at 10–12 weeks Palpable fetal outline and fetal movement after 20 weeks Visualization of fetus with cardiac activity by ultrasound (fetal parts visible by 8 weeks) Pregnancy and fundal height measurement Signs of pregnancy (presumptive, probable, positive) Pregnancy and fundal height measurement As pregnancy progresses, the fundus rises out of the pelvis (Figure 29-1). At 12 weeks’ gestation, the fundus is located at the level of the symphysis pubis. By week 16, it rises to midway between symphysis pubis and the umbilicus. By 20 weeks’ gestation, the fundus is typically at the same height as the umbilicus. Until term, the fundus enlarges approximately 1 cm per week. As the time for birth approaches, the fundal height drops slightly. This process, which is commonly called lightening, occurs for a woman who is a primigravida around 38 weeks’ gestation but may not occur for the woman who is a multigravida until she goes into labor Naegele’s rule Add seven days to the first day of your LMP and then subtract three months. For example, if your LMP was November 1, 2017: Add seven days (November 8, 2017). Subtract three months (August 8, 2017). The EDD is calculated by adding seven days to the first day of the last menstrual period, subtracting three months and adding one year. This formula is known as Naegele's Rule. For example, if the patient's last menstrual period, LMP, was on August 10, 2019, the EDD would be calculated as follows. LMP equals August 10, 2019 plus seven days. August 17, 2019, minus three months. May 17, 2019 plus one year and that equals May 17, 2020. Hematological changes during pregnancy During pregnancy, the heart is displaced upward and to the left within the chest cavity by the gravid uterus’s pressure on the diaphragm. As pregnancy progresses, the risk for inferior vena cava and aortic compression leading to supine hypotension increases when the woman lies in a supine position. To avoid hypotension and potential syncope, the woman should be advised to lie in a left lateral position. Hemodynamic changes and anatomic changes also may alter vital signs in the pregnant woman (Table 29-2). Cardiac output in pregnancy increases by 30% to 50% over that in women who are not pregnant (Blackburn, 2013; Ouziunian & Elkayam, 2012). This increase peaks in the early third trimester and is maintained until birth. Half of the total increase in cardiac output, however, occurs by the eighth week of pregnancy (Blackburn, 2013). Therefore, women with cardiac disease may become symptomatic during the first trimester. Stroke volume is also increased during pregnancy by 20% to 30%. These increases in cardiac output and stroke volume allow for the 30% increase in oxygen consumption observed during pregnancy. TABLE 29-2 Vital Sign Changes in Pregnancy Vital Sign Changes in Pregnancy Measurement Alterations in Pregnancy Heart rate and heart sounds Volume of the first heart sound may be increased with splitting. Third heart sound may be detected. Systolic murmurs may be detected. Increases by 15–20 beats/min by 32 weeks’ gestation. Palpate the maternal pulse when auscultating the fetal heart rate to be able to distinguish between the two. Respiratory rate Increases by 1–2 breaths/min None BP First trimester: same as prepregnancy values Second trimester: systolic BP decreases by 2–8 mm Hg and diastolic BP decreases by 5–15 mm Hg due to peripheral vascular resistance Third trimester: gradually returns to prepregnancy values Use of an automated cuff may improve accuracy of measurement, as some pregnant women do not have a fifth Korotkoff sound. Systolic and diastolic BP may be 16 mm Hg higher when taken while the woman is sitting. BP readings may decrease in the maternal left lateral position. Abbreviation: BP, blood pressure. Data from Jarvis, C. (2016). Physical examination and health assessment (7th ed.). St. Louis, MO: Saunders Elsevier; Ouziunian, J., & Elkayam, U. (2012). Physiologic changes during normal pregnancy and delivery. Cardiology Clinics, 30, 317–329; Tan, E., & Tan, E. (2013). Alterations in physiology and anatomy during pregnancy. Best Practice & Research Clinical Obstetrics & Gynaecology, 27, 791–802. During pregnancy, blood volume increases by 30% to 50%, or 1,100 to 1,600 mL (Ouziunian & Elkayam, 2012), and peaks at 30 to 34 weeks’ gestation. The increase in blood volume improves blood flow to the vital organs and protects against excessive blood loss during birth. Fetal growth during pregnancy and newborn weight are correlated with the degree of blood volume expansion. Of the blood volume expansion occurring during pregnancy, 75% is considered to be plasma (King et al., 2015). There is also a slight increase in red blood cell volume (RBC). The blood volume changes result in hemodilution, which leads to a state of physiologic anemia during pregnancy. As the RBC volume increases, iron demands also increase. Leukocytosis occurs in pregnancy, with white blood cell counts increasing to as much as 14,000 to 17,000 cells per mm3 of blood (Table 29-3). Clotting factors increase as well, creating a risk for clotting events during pregnancy. Systemic vascular resistance is reduced due to the effects of progesterone, prostaglandins, estrogen, and prolactin. This lowered systemic vascular resistance, in combination with inferior vena cava compression, is partly responsible for the dependent edema that occurs in pregnancy. Epulis of pregnancy, or hypertrophy of the gums accompanied by bleeding, may also occur and is due to decreased vascular resistance and increase in the growth of capillaries during pregnancy [Show More]
Last updated: 1 month ago
Preview 1 out of 64 pages

Reviews( 0 )
Document information
Connected school, study & course
About the document
Uploaded On
Nov 19, 2020
Number of pages
64
Written in
Additional information
This document has been written for:
Uploaded
Nov 19, 2020
Downloads
1
Views
46




















.png)