*NURSING > NCLEX-RN > Cardiovascular - Summary Saunders Comprehensive Review for the Nclex-Rn Examination Cardiovascular N (All)
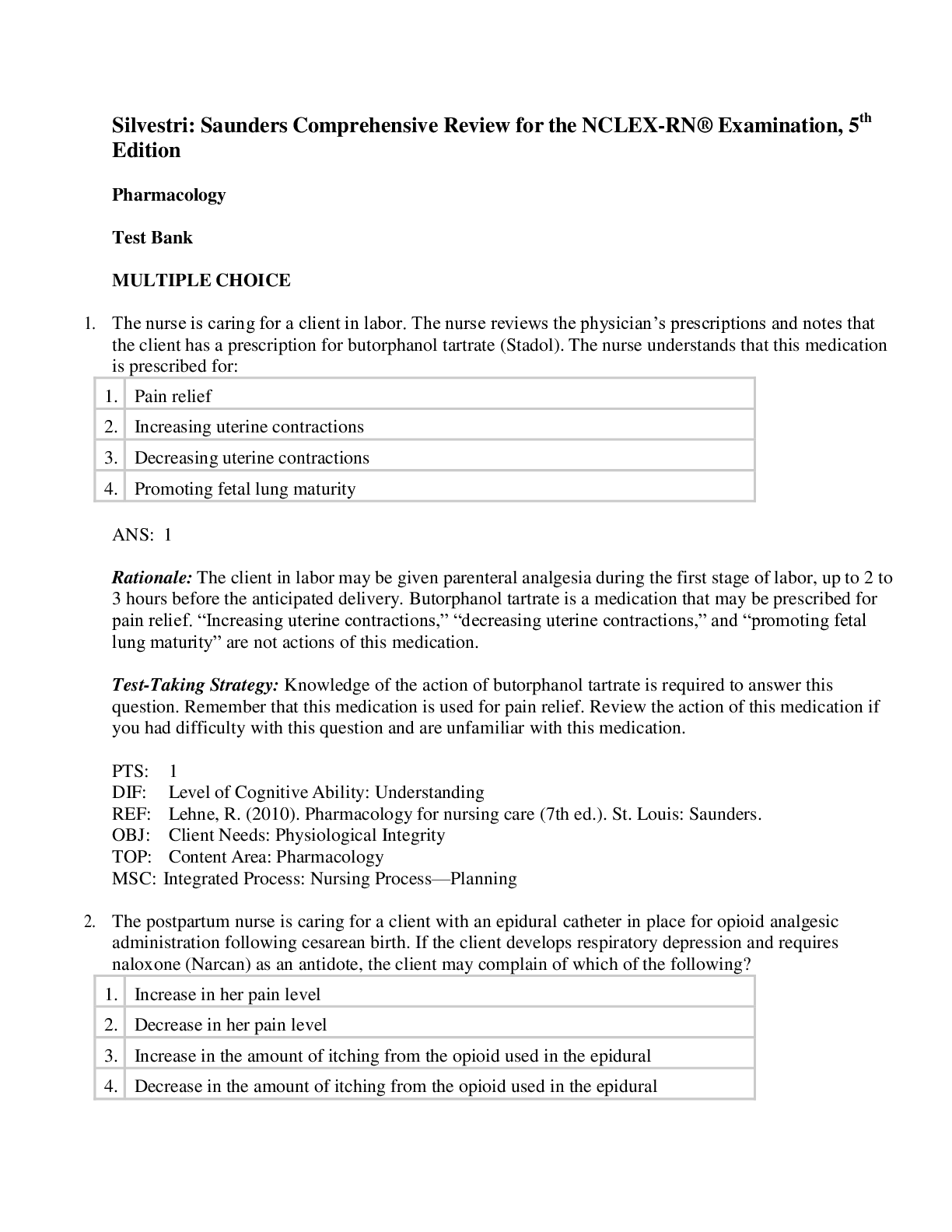
Cardiovascular - Summary Saunders Comprehensive Review for the Nclex-Rn Examination Cardiovascular Nursing. Everything you need to know about cardiovascular nursing (excluding pharmacology) based on lecture notes and Saunders Comprehensive Review for the NCLEX-RN Examination.
Document Content and Description Below
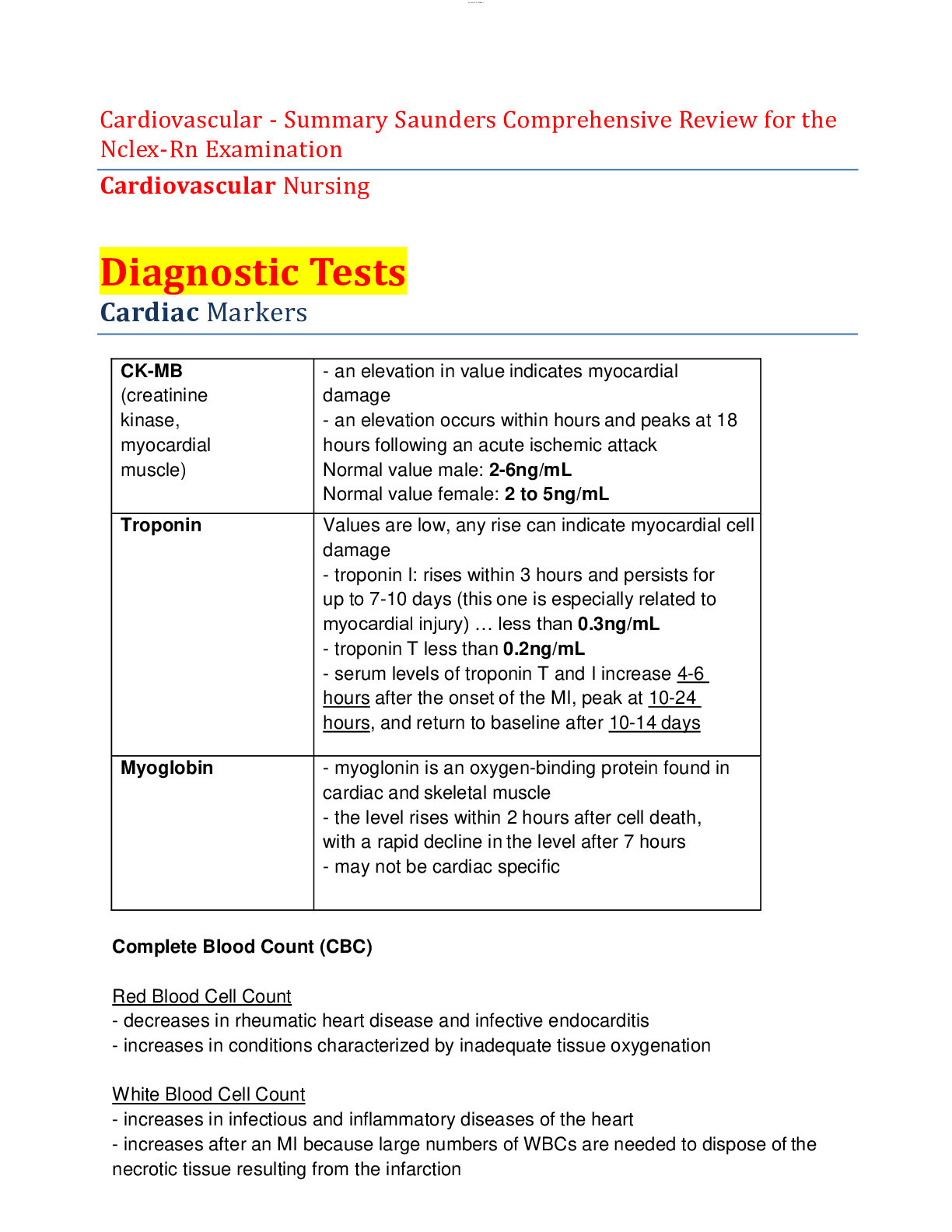
Cardiovascular - Summary Saunders Comprehensive Review for the Nclex-Rn Examination Cardiovascular Nursing Diagnostic Tests Cardiac Markers CK-MB (creatinine kinase, myocardial muscle) - an ele... vation in value indicates myocardial damage - an elevation occurs within hours and peaks at 18 hours following an acute ischemic attack Normal value male: 2-6ng/mL Normal value female: 2 to 5ng/mL Troponin Values are low, any rise can indicate myocardial cell damage - troponin I: rises within 3 hours and persists for up to 7-10 days (this one is especially related to myocardial injury) … less than 0.3ng/mL - troponin T less than 0.2ng/mL - serum levels of troponin T and I increase 4-6 hours after the onset of the MI, peak at 10-24 hours, and return to baseline after 10-14 days Myoglobin - myoglonin is an oxygen-binding protein found in cardiac and skeletal muscle - the level rises within 2 hours after cell death, with a rapid decline in the level after 7 hours - may not be cardiac specific Complete Blood Count (CBC) Red Blood Cell Count - decreases in rheumatic heart disease and infective endocarditis - increases in conditions characterized by inadequate tissue oxygenation White Blood Cell Count - increases in infectious and inflammatory diseases of the heart - increases after an MI because large numbers of WBCs are needed to dispose of the necrotic tissue resulting from the infarction Hemocysteine - elevated levels may increase the risk of cardiovascular disease - normal value: 0.54 to 1.9 mg/L Highly Sensitive C-Reactive Protein - detects an inflammatory process (e.g. atherothrombosis) - less than 1mg/dL is considered low risk - greater than 3mg/dL Blood Coagulation Factors - an increase can occur during and after an MI, which places the patient at greater risk for thrombophlebitis and formation of clots in the coronary arteries Serum Lipids - the lipid profile measures serum cholesterol, triglyceride, and lipoprotein levels - lipid profile is used to assess the risk of developing coronary artery disease - lipoprotein-a or Lp(a) increases atherosclerotic plaques and increases clots…. Normal value should be less than 30mg/dl Electrolytes * electrolyte and mineral imbalances can cause cardiac electrical instability that can result in life-threatening dysrhythmias Potassium Hypokalemia - causes increased cardiac electrical instability, ventricular dysrhythmias, and increased risk of digoxin toxicity - ECG shows flattening and inversion of the T wave, the appearance of a U wave, and ST depression Hyperkalemia - causes asystole and ventricular dysrhythmias - ECG shows tall, peaked T waves, widened QRS, or flat P waves Sodium - the serum sodium level decreases with the use of diuretics - the serum sodium level decreases in heart failure, indicating water excess Calcium Hypocalcaemia - can cause ventricular dysrhythmias, prolonged ST and QT intervals, and cardiac arrest Hypercalcemia - can cause atrioventricular block, tachycardia or bradycardia, digitalis hypersensitivity, cardiac arrest Phosphorus - should be interpreted with calcium levels because the kidneys retain or excrete one electrolyte in an inverse relationship to the other Magnesium - low level can cause ventricular tachycardia and fibrillation Blood Urea Nitrogen - BUN is elevated in heart disorders that adversely affect renal circulation, such as heart failure and cardiogenic shock - range: B-type Natriuretic peptide (BNP) - BNP is released in response to atrial and ventricular stretch; it serves as a marker for heart failure - should be less than 100pg/mL… the higher the level, the more severe the heart failure Diagnostic Procedures Chest X-Ray - done to determine anatomical changes such as size, silhouette, and position of the heart Holter Monitoring - noninvasive test where the client wears a monitor and an electrocardiographic tracing is recorded over 24 or more hours while the client performs their activities of daily living - the monitor identifies dysrhythmias and evaluates the effectiveness of anti-dysrhythmic or pacemaker therapy Echocardiography - non-invasive procedure that evaluates structural and functional changes in the heart - used to detect vulvar abnormalities, congenital heart defects, cardiac function Exercise Electrocardiography Testing (stress test) - studies the heart during activity and detects and evaluates coronary artery disease - treadmill testing is the most common - if the client is unable to tolerate exercise, an IV infusion of dipyridamole or dobutamine hydrochloride is given to dilate the coronary arteries and stimulate the effects of exercise (NPO for 3-6 hours before) Cardiac Catheterization - an invasive test involving the insertion of a catheter into the heart and surrounding vessels - obtains information about the structure and performance of the heart chambers and valves and the coronary circulation Pre-procedure interventions: - obtain informed consent *****************************************CONTINUED**************************************** [Show More]
Last updated: 1 year ago
Preview 1 out of 61 pages

Reviews( 0 )
Document information
Connected school, study & course
About the document
Uploaded On
Sep 02, 2020
Number of pages
61
Written in
Additional information
This document has been written for:
Uploaded
Sep 02, 2020
Downloads
1
Views
313